Why is my site with a map devoted the health in Mexico the most popular?
How much will the rise in Hispanic culture medical needs impact U.S. healthcare system over the next decade or two?
What does a 125 year old map of the health in Mexico tell us?
This map is from my most heavily visited page to date on my blog devoted to historical medical geography, spatial epidemiology, cultural medicine, and the history of medicine. (My site surpassed the rate of 100,000 hits per year, or 65,000 people/year, a month or two ago).
Source: brianaltonenmph.com
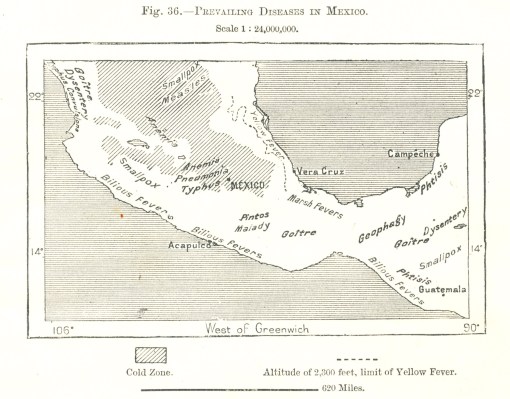
This above map is found on p. 91 of THE EARTH AND ITS INHABITANTS NORTH AMERICA, Vol. 2, by the famous French Geographer Élisée Reclus (1830-1905).
From 1875 to 1894 Reclus published one of the best known series on global populations, a 19 volumes series on "Universal Geography" entitled La Nouvelle Géographie universelle, la terre et les hommes.
This version of the map however comes from another book by Reclus (probably in Universal Geography as well)–THE EARTH and ITS INHABITANTS. NORTH AMERICA (New York by D Appleton & Co., 1891).
According to a population density map contained in this volume (Fig. 71, p. 171, The Density of the Population in Mexico"), the densest population at the time was the darker (cooler) region where anemia, pneumonia, and typhus are mentioned, just north and northwest of the label "MEXICO."
I produced a fairly complete explanation of this map years ago, accessible at my personal blog site (https://brianaltonenmph.com/gis/historical-disease-maps/centralmexico/ ).
The popularity of this map suggests my site is heavily visited by US students and professionals interested in Mexican/Hispanic culture and how this impacts local medical geography, our current health care needs, the history of health related needs amongst Hispanics and their communities.
The popularity of this page also sends an interesting message to the medical profession.
It popularity may also be because members of the Hispanic communities in the United States have a growing interest in their own heritage, or because non-Hispanic people want to learn more, or because meeting the needs of the Hispanic patient is perhaps one of the most important cultural health issues to date in the US healthcare system.
Whatever the reason, we also know that the history and geography of Mexico and Central America are popular topics for classes taught in schools and colleges across this country. One of the least discussed parts of this aspect of American history (all 3 or more Americas) is the long term impact of a rapidly growing Hispanic culture on the United States healthcare system.
Like the American Indian public health dilemma, there are a bunch of popular impressions taught about Europeans, Hispanics and the Indigenous that are not completely true.
These two cultures had impact on each other, in such a way that this topic cannot be taught effectively in any single college level program, except as a discipline.
In terms of medical history, the history of New Spain health is more than just a story of how Europeans wiped out so indigenous groups through the communication of small pox and measles. There is also the tale of how certain venereal diseases were brought back to Europe by sailors venturing deep into the woods of the New World, a New World blessing for the social elite back home. (Diseases do travel both ways, from culture to culture.)
Reclus covers but a small part of this history, mostly superficially, but most importantly, with a focus on Native Mexican-American Hispanic cultural diseases, not on the other diseases that strike this area due to in-migrating African-Americans for nearly two centuries.
Small pox and measles prevail where large numbers of indigenous people reside. Most of the fevers are close to the shorelines, a product of local vectors and ships bearing the contagion in the form of mosquitoes from Jamaica, Cuba, afar. Poor nutrition due to foodways are prevalent in those regions where Goiter is noted. Geophagy (Clay-eaters) is a unique culturally-linked, or culturally-bound behavior (in Jamaica as well). Pintos Malady (today, Pinta), is an ecologically-defined variety of falciparum diseases, characterized by large dark patches and skin mottling.
Most important to note here is the need for a more extensive program devoted to a more comprehensive approach to monitoring cultural health within the US healthcare system. Medicine is not just the practice of health care using solely western philosophy and health paradigms. The basic Western European motif for defining the healthcare is not always clinically perfect for these other cultural groups.
With a rise in the size of the Hispanic population in the U.S. (see the 2020 census predictions), and a matching rise in African/African-American, Caribbean, Asian, Indigenous, Muslim, and other cultural healthcare demands, ad infinitum, the "traditional medicine" everyone is currently encouraged to practice will have to be supplemented by programs devoted to understanding the culturally-bound syndromes (geophagy, the Mexican interpretation of seizures), culturally-linked diagnoses (pinta, chiclero’s ear) and the ongoing culturally-related risks for the most common maladies (i.e. asthma, diabetes, certain heart diseases, blood dyscrasias, through genetics, foodways, etc.)
I review culturally-bound, linked and related diagnoses and disease states at a number of places (start with https://brianaltonenmph.com/gis/populations-and-managed-care/disease-patterns-linked-to-culturally-defined-health-regions/ ). My coverage focuses on how to improve a healthcare program by defining how to improve upon its cultural knowledgebase, awareness and sensitivity, and develop a more efficient, culturally targeted interventions program.
[For more on Reclus, see http://en.wikipedia.org/wiki/%C3%89lis%C3%A9e_Reclus; the book with this map is at http://books.google.com/books?id=dxj3Qr2RIWYC 😉
See on Scoop.it – Medical GIS Guide