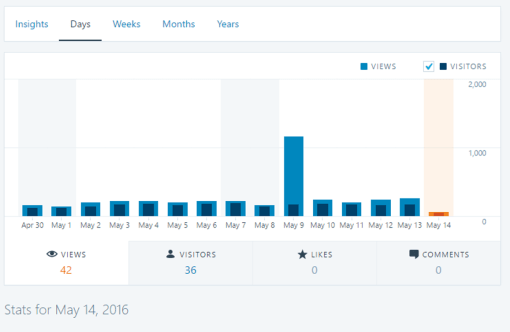
About twice a year I get these huge spikes in people visiting my site.
What does it mean?
The first time this happened, I had about 3000 hits in 24 hours. Totally unexpected, it led me to contract the company that provides the place where my site and information are housed. Their response . . . . normal traffic, due likely to a recommendation to visit my site by a place with regular visitors or a list of subscribers.
At times, there is no telling why these people visit. If I am lucky, I can link the surge in visitors to a single page and topic. One day, a few years ago, I was able to find a web page indicating that a conference was being held at the moment, and my site was possibly referred to as an example of what is out there. The topic . . . medical GIS.
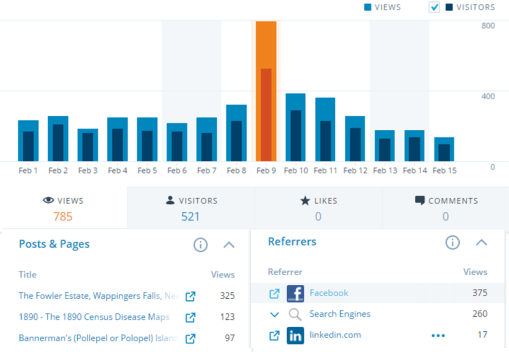
Several times I have been able to link the masses of visitors to a specific topic or course related to medical GIS. My hexagonal grid mapping is the most common page frequented now by medical GIS students. Interestingly, it also suggest that professors and practitioners in the field of medical GIS have yet to adopt this new methodology.
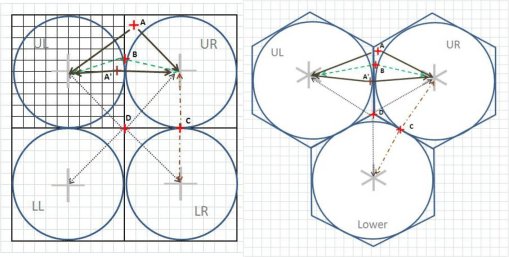
My illustration for the math behind hexagonal grid mapping.
There are some things that the health profession cannot do. They cannot treat everyone perfectly. They cannot prevent the most basic iatrogenic illnesses and surgical mistakes from happening. The evolution of new disease and illness, due to the clinical setting, are natural events–the profession’s decision to focus on just the insured at the risk of ignoring the uninsured is the reason we are having immunizable disease outbreaks. relying upon false assumptions and grandiose conclusion drawn about the success of your 98% effective immunization program, is like turning your back to the plank fence blocking your view of all those poorer communities you have missed.
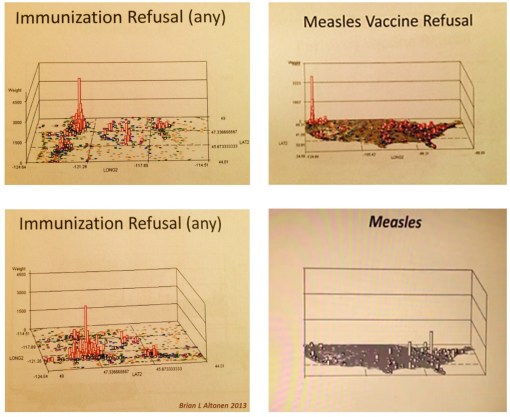
The recent resurgence in in-migrating vectored diseases is an indication that public health and the world health were taken by surprise by the ability of old diseases to travel to new places. Why the errors?

Understaffing at the WHO level, and those whom were employed weren’t experts at all compared to some of the leaders in this field, and the questionable ability of United States, CDC, and even NIH leaders to even successfully managed its small pox labs and anti-terrorism teams. We do not know if AIDS was ever borne due to corporate lack of control, but we do know that Anthrax made its way into the public setting due to poor management and leadership, or that old vials of forgotten test samples of small pox could be found, where they were never supposed to be stored these past 50 to 60 years.
Fortunately, what few open minds that there are for new discoveries, are mostly found in the student populations of public health programs.
In just a few months, any system can design a means to managed its population using just five basic query paths for its EMR. This means that while systems struggle to make their EMR systems perform and function at the clinical level, quality improvement teams working on their own at the corporate or institutional level can produce a system that makes more effective use of their data at one or two thousand times the other teams’ productivity level.
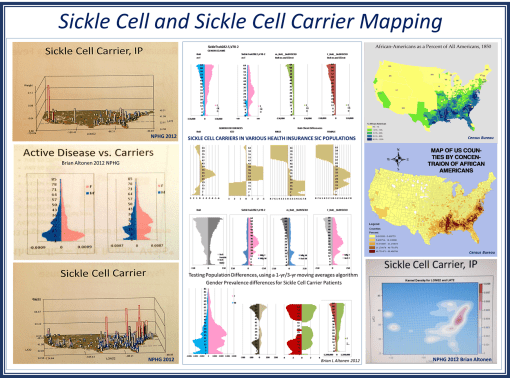
Meaningful use has some meaning. But it tells us little about the prevalence of genetic diseases, the amounts of illegal care practices being performed such as childhood female circumcision, the amount of spousal abuse engaged in by specific religious groups, the amounts of poor nutrition and malnutrition related conditions suffered by low income communities, the amounts of MVAs experienced by kids riding ATVs, the numbers of people who refuse to have their kids immunized and locations of their clusters, the age at which boys are least likely to see a doctor, the kinds of developmental disorders that are surging in certain ethnic groups.
We can brag about about MU attempts and the results of a few of those 40 or 50 measures we’re focused upon. Yet throughout all the hours spent trying to get a perfect outcomes and report generated, we miss nearly 99% of the population still in need of the same type of care and managed care improvement processes.
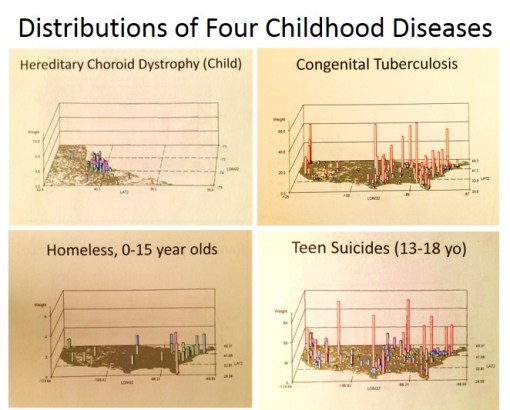
This latter reason is the primary reason Medical GIS has to be implemented as a core part of all managed care programs. But as the evidence shows regarding those that visits my pages devoted to Medical GIS, such a change is perhaps another generation or two away from happening. Leadership, management, directors and VPs are still struggling, trying to make progress about a subject that should have been resolved nearly a decade ago, when medical GIS was ready to become a standard.
