Socioculturalism and Health
Introduction
Throughout the ICDs that can be evaluated are those of a sociocultural nature. Any study of socioculturalism and disease is complex due to the subjectivity of how this field was initially developed and since then has been subsequently re-defined and re-adapted several times. One of the major outcomes of this controversy are questions regarding lack of objectivity. The development of DSM and ICD systems has been somewhat culturally-based. This has prevented these methods of coding diseases to be effective when it comes to relying upon ICD-9 codes to identify culturally-bound syndromes.
Like the nosologies of medicine during the 19th century, the current taxonomy (a more detailed and binary logic-based nosology) has relied upon an ever changing flowchart to define each and every diagnosis. A physician familiar with this system for coding disease is familiar more with the global or western philosophy of disease, not always any true cause for certain diseases. For this reason, the new ICD-10 about to be implemented partially corrects for many of these failures produced by the ICD-9. As multiculturalism becomes more respected socially, so too does the need for better understanding any other cultural traditions and beliefs that make a disease develop. Some diseases are purely cultural in that they are psychosomatic in nature and a consequence of the belief system the patient has towards his/her disease. This may even result in new labels given to the disease, as well as new names, new expectations, and even new responsibilities. In one social setting, a child with Tourette’s Syndrome is considered to have some sort of age-link tic-related disorder, and yet in another considered to be chanelling with extracoporeal or past spirits, and in another a victim of loss of soul followed by replacement of a past soul. The old ICD-9 system has just a few ways to define this condition, noting it with neurological and psychiatric and perhaps psychological, psychosomatic ICDs. The newer system has a more detailed cultural definition for the original state and its various components or axes, ranging from direct to indirect physiological and non-physiological linkages to other conditions or behaviors.
The newer ICD system manages to provide a way to identify certain cultural differences that exist in disease progression. But it doesn’t necessarily change the interpretation of disease at all. Instead, it provides us with a way to define why some ICDs which have been assigned to a medical condition fail to meet the age-gender distribution features of that particular psychiatric, mental, psychosomatic, or physical disease. This review of population pyramids demonstrates how the current ICD system still misses the boat often when it comes to exactness in details. The new ICD assignments for culturally bound syndromes still lack in demonstrating any direct age-gender link to the traditional ICD and the actual appearance of a particular medical condition. In addition, this new system still lacks some of the associations being made betwen particular conditions and the possible application of the terms “culturally-bound” to these Western Medicine, Developed Country related medical conditions or diseases. A disease like anorexia nervosa is in some ways just as culturally bound as a possession of soul believed in by Hmong parents with children who demonstrate a history of epilepsy.
For this reason, we have to dissect “culturally-bound” diseases further. These sociocultural-linked diseases are of several forms. Some are completely physical in nature, meaning they are physical changes and manifestations of a health condition in the body that is due completely to heredity. There are also physical diseases that develop due to cultural behaviors, and are often related to morees and taboos such as restrictions in diet, restrictions in physical social engagements (sports, groups meeting behaviors, religious practices involving interperson contact and the like), restrictions in how we must behave in terms of selecting spouses and marriages. Thirdly, there are behavioral psychological and biopsychological (even biological and psychiatric related) conditions that at times have an important physical science component, for example schizophrenia is an inherited trait common to the German speaking Amish communities. Finally, there are those primarily sociocultural or simply socially defined diseases, which are behavioral and psychological problems defined as such by the traditional culture, such as the Amok suicidal problem experienced by South Asian communities, or the unique stress syndromes many cultures have due to moving to a new setting.
Culturally-linked diseases excluded from this review are those with an ecological component to their social, regional or even ethnic history. Examples of conditions excluded from this review include some very biological sociocultural-linked conditions also common to Western Society, but with different incidence rates, such as
- numerous zoonotic pathogens, for example
- intestinal organisms like the African tapeworm (Taenia solis) ,
- the Mexican-borne version of Syphilis strain resulting in pinta
- the unique occupational disease Chiclero’s Ear.
- “Old World” versus “New World” STDs, due to the controversy over the true origins of certain STDs during the colonial era
- Recreational or religious natural products use, including cocaine leaf chewing, the Kat of Somalia, Betel Leaf consumption, India’s Hashish, Island Community nutmeg- or salap-related consumption, etc.
Culturally-bound Syndromes
Those most interesting diseases, conditions, or states to review are those which have distinct cultural definitions. In many cases these are defined as “diseases” or maladies only due to the way in which the Western Physician making use of these ICD systems defines a lack of normality, and subsequently identifies someone as “not normal”. These conditions are atypical to Western Culture, and at times could be likened to someone claiming a pattient is sick due to some misbehaved chakra or acupuncture point, reasoning not at all different from the “hot spots” or sensitive points philosophy used to explain something as western medicine-defined as fibromyalgia.
The result of this philosophical approach used in western medicine by way of certain portions of the ICD system is the creation of certain conditions or diseases that are assumed to be proper and in need of such identification. The most commonly known results of such subjectivity and individual beliefs in medicine are those ICDs used, once used, or considered for the explanation in such human conditions and behaviors as the “Psychosomatically-induced” Irritable Bowel Syndrome identified as such by the 1950s, or the reason an individual becomes a criminal, or engages in unique sexual acts. Each of these has past and present pathological definitions attached to them, some considered solely psychiatrc, others considered biological, still others behavioral and as a result of “social detachment.” Culturally-bound syndromes change in definition over time. Most of the currently accepted syndromes for this category have some unique traits that define them as not a consequence of what western culture defines to be illness-inducing conditions or behaviors.
The first list of these syndromes which follows are for ICD defined states that are very much subjective in their representation, causology and health-related outcomes. A certain number of these ICD-defined states or conditions are cultural in nature due to the rarity of what they represent, and the decision made by the medical field in general to categorize these features to just a particular group. The ICD 10 or DSM-IV-TR recognizes the following examples of these syndromes which are most closely linked to the contemporary definition for a “culturally bound” syndrome.
- Amok. Malaysia. Periods of “homicidal frenzy”, brooding, and finally somnolence and amnesia. Afflicts mostly young to middle-aged males living away from home (college students). Often ends in suicide. ICD 10 code = F68.8 Other personality disorders of adult personality and behavior. Associated with Lin-Keh-Ming and hwa-byung of Korea. Other similar culture bound syndromes are perhaps: colerina-Andes Bolivia, Columbia, Ecuador, Peru, iich’aa Southwestern US Indigena, berserkergang-Scandinavia (Saami), cafard-Polynesia, benzi mazarazura– south African Shona, and ahad idze be-New Guinea.
- Ataque de Nervios. Puerto Ricans and certain other Latinos/as. Uncontrollable shouting, trembling, heart palpitations, sense of heat rushing to the head, fainting and seizure like activities, temporary loss of consciousness, purported amnesia. Afflicts socially disadvantages women > 45 yo with no high school education. See “Nerves.”
- Brain Fag. West Africa. Sometimes equated with Chinese equivalent neurasthenia, Korean hwa-byung, or Latino susta. A form of depression, anxiety or somatoform condition.
- Dhat. India, China. Also called dhatu, jiryan, shen k’uei, and shen-kui. Characterized by anxiety, fatigue, somatic pains, “loss of energy”. Philosophically felt to be linked to semen loss, and so due to excess semen loss, leading to imbalances in the body’s five elements/four humours, made worse by bad diet. According to Chinese medical philosophy, the traditional mechanism for developing this condition is excess coitus, with chi loss incurred and loss of the spiritual “energy” or parts involved with making chi. The shen is akin to the essence used to produce the ‘vital force’ of late 18th and early 19th century western medical philosophy. Shen is “the sign of life in someone’s eyes”; loss of shen preceding death results in a very dark appearance of the inner orbit as seen through the pupil. As the Chinese names imply, disturbance and removal of this shen ensues (shen-kui). ICD 10 assignment: F48.8 Other specific Neurotic Disorder, or F45.34 Somatoform autonomic dysfunction of the genitourinary system (this may include autonomic anxiety symptomatology). Western medical collquial terms identify this as a sexual neurosis.
- Hwa-byung. Korea. “Firey illness”. Anger or rage manifesting with pressure on the chest, movement of heat about the body, indigestion, fatigue, headache, and a variety of mood changes. Women are perhaps afflicted more than men. Philosophically this syndrome blamed on the oppression of Korean culture.
- Koro. Hainan island of China, India, Singapore, Thailand. From “koro” for turtle. Anxiety and panic resulting in or are caused by a fear that the penis is retracting (like a tortoise head) into the abdomen. For women, breasts and genitalia are thought to contract. Excess coitus, exposure to cold, illness induce the signs (related appearances). Devices are used to prevent the retraction. Cantonese refer to this as suk-yeong, Mandarins as suo-yang, Assams as jinjinia bamar, Thai as rok-joo, Eastern Indians as rabt. ICD 10 assignment: F48.8 Other specific Neurotic Disorder, or F45.34 Somatoform autonomic dysfunction of the genitourinary system (this may include autonomic anxiety symptomatology). ICD9 – any combination of: Psychosexual dysfunction (302.7*), Impotence/Frigidity (302.72), Anorgasmia (302.73, 302.74)
- Latah. Malays. Startle or fright reflex responses characterized by exageration, such as overesponse to stimuli (recall autonomics and the fight or flight responses in relation to fright). Echopraxia, echolalia, and command obedience behaviors can ensue. Patient seems trancelike or even dissociative. Most often associated with women of low economic status. Similar syndromes in other cultures include amurakh (Siberia), iekunii, ikota, okan, myriachit, menkeiti, Lapp panic (Lapps), bachtschhi (Thailand), imu (Ainu indigena of Japan), mali-mali (Philippines), silok, susto (Mexico), yuan (Myanmar, formerly Burma), jumping (French Canada). ICD 10 – F48.8 Other Specified Neurotic Disorders, F48.88 Other Specified Dissociative [Conversion] disorders.
- “Nerves.” Nerfiza (Egypt), Nevra (Greece), nervios (Mexico, Central and South America), nerves (northern Europe). Sorrow or anxiety, leading to head and muscle pain, reactivity, nausea, appetite loss, insomnia, fatigue, agitation. Linked to stress and low self-esteem. Women experience this more than men. ICD 10 F32.11 Moderate Depressive Episode with somatic syndrome, F48.0 Neurasthenia, F 45.1 Undifferentiated Somatoform Disorder. Related syndromes include: anfechtung (Hutterites), brain fag (Nigeria), colerina, pension and bilis (Mexico, Central America, South America), hsieh-bing or xie -bing (China), hwa-byung (Korean peninsula), qissaatuq (Inuits in Arctic territories), narahati-e a sa or maraz-e a-sab (Islamic Republic of Iran).
- Pa-leng. China, esp. Taiwan, parts of southeast Asia. A frigiphobia, or fear of the cold or winds, due to association of these natural features with fatigue, impotence and death. Belief in the humoral theory for illness is an important part of these cultures. Fear is accompanied by onset of anxiety and obsessiveness. ICD 10- F40.2 Specific Phobias. Mexico and Central and South America have the related disorders agua frio, aire frio and frio.
- Pibloktoq. Arctic and Subarctic Inuit. Arctic hysteria. Primarily associated with women. Preceded by tiredness, lack of facial expression, social extreme quietness, confusions. Events begin as “extreme excitement”, followed by convulsions and pseudo-coma like states. Peak attacks demonstrate adrenalin-like effects including significant strength and abberant physical and verbal behaviors. Indicative actions include removal of clothing, fleeing, jumping in water, rolling in snow, mimetic acts, choreiform movement, glossolalia, and coprophagia. Events end with fatigue, sleep and return to typical states following reawakening (see ref1., ref2; ICD 10 possibly: 1) F44.7 Mixed Dissociative (Conversion) Disorder or 2) F44.88 Other specific dissociative (conversion) disorder. Related to amok (Indonesia, Malaysia), banga or misala (Congo, Malawi, formerly Nyasaland), ebenzi (southern Africa, esp., Shona and affiliates), grisi siknis (Miskito, Honduran Indigena), imu (Ainu, indigena of Japan), latah (Indonesia, Malaysia), mali-mali (Philippines), nangiarpok, kayak angst, quajimaillituq (Inuit), ufufuyane (southern Africa, esp. Bantu, Zulu and affilated groups). Blood and physiological biochemical findings have led to numerous theories, including Vitamin A overdose. Episodes last for several minutes, and may have some relation to hypocalcemia-induced tetany cases. Interpersonal anxieities and cultural stressors play an important role, along with the meaning and purpose of this event.
- Shenjing Shuairuo. China. Sense of mental and physical exhaustion, memory loss, inability to concentrate, irritability, headaches, weakening of nervous activities or nervous system (“neurasthenia”).
- Susto. Also called Espanto. Mexico, Central and South America. “Soul loss” induced by the supernatural. Chief emotional result is fright, with minimal traumatic events physically experienced. Symptoms include agitation, anorexia, insomnia, fever, diarrhea, mental confusion, apathy, depression, introversion. Hypoglycemic states related to some events. Anxiety due to social stressors is a major contributor. Related to grief-loss events in life. ICD 10 is F45.1 Undifferentiated somatoform disorders, or F48.8 Other Specified Neurotic Disorders. Related to lanti (Philippines), latah (Indonesia, Malaysia), malgri (Australian aborigines), mogo laya (New Guinea), narahati (Islamic Republic of Iran), and saladera (Amazonian region).
- Taijin Kyofusho. Japan. Other names: shinkeishitshu, or anthropophobia (fear of people, people interactions, and contracting disease). Social phobia about how one appears of presents himself/herself, behaviorally and somatically. Avoidance of close contacts may result. Feelings of embarassment, blushing; concerns that appearance, facial expressions, smell, words stated, might cause social unrest. Mostly afflicts younger people. Perfectionism may be a behavioral feature that results, with cultural influences upon younger populations resulting in “over-socilization” accompanied by perfectionism and then followed by breakage of social bonds due to feelings of inferiority and anxiety about personal presentation. ICD 10 – F40 Social Phobias, or F40.8 Other Phobic Anxiety Disorders. Other conditions with similar presentation: anfechtung (Hutterites), and itiju (Nigeria).
- Ufufuyane. South Africa, esp. Bantu, Zulu and allies, and Kenya. Also referred to as saka. Anxiety state attributed to magic potions administered by rejected lovers, or due to spirit possession. Akin to voodoo (voodu) beliefs in part. Shouting, sobbing, paralysis, convulsions, trance-like stupor and loss of consciouness is associated with these spells. Young unmarried women are most often afflicted. Can relate to nightmares and night horrors with sexual themes, somnambulism, temporary blindness. Attacks last from days to weeks, and have a psychosomatic onset triggered by the sight of certain men or foreigners. ICD 10 codes are F44.3 Trance and possession disorders, or F44.7 Mixed dissociative [conversion] disorders. Other syndromes related to this include aluro (Nigeria), phii pob (Thailand), and zar (Egypt, Ethiopia and Sudan).
- Uqamairineq. Inuits in the Arctic region. Paralysis of sudden onset with borderline sleep states; anxiety, agitation and hallucinations are related. Prodromal indicators are noted such as transient sound or smell (taste as well?). Chronic disease, resulting in attacks that last for several minutes at a time. Syndrome is related to “soul loss” experiences, “soul wandering” or spiritual possession. Dissociative hysteria cases have been realted to this, along with narcolepsy-catalepsy syndromes. ICD 10 is F44.88 Other Specific Dissociative [Conversion] Disorders and G47.4 Narcolepsy and Catalepsy (including sleep paralysis). Related to aluro (Nigeria), old hag (Newfoundland), and phii pob (Thailand).
- Windigo. Northeastern Indigena of North America. Traditionally considered a form of psychosis. Rare cases have cannibalistic obsession. Traditional beliefs blame this on possession, usually of males, turning them into “cannibal monsters.” Depression, homicidal or suicidal thinking, and delusions are common, The ‘wish to eat human flesh’ is an indicator. Typical of people ostracized by their immediate peers and/or society. Chronic food shortages and cultural myths support the belief system leading to these states. Some studies suggest this medical illness is a made up syndrome meant to ostracise or execute governmental changes. ICD 10 suggested is F68.8 Other Specific disorders of adult personality and behavior. Related to amok (Malaysia), hseih-ping (China, esp. Taiwan), and zar (Egypt, Ethiopia and Sudan).
The new ICD 10s for the above states are from the WHO ICD-10 classification of mental and behavioural disorders (see also Hirsch and Weinberger’s (eds.) Schizophrenia (2003)); a partial list of possible ICD9s appear in brackets. These diagnoses are as follows.
- F32.11 Moderate Depressive Episode with somatic syndrome [296.2-3?] – Ataque de Nervios, Nerves
- F40 Social Phobias [300.23] – Taijin Kyofusho
- F40.2 Specific Phobias [300.2*] – Pa-leng
- F40.8 Other Phobic Anxiety Disorders [300.2*, 300.20] – Taijin Kyofusho
- F44.3 Trance and possession disorders – Possession Disorder, Ufufuyane
- F44.7 Mixed dissociative [conversion] disorders [ICD9 300.1*, 300.11] – Pibloktoq, Possession Disorder, Ufufuyane
- F48.8 Other specific Neurotic Disorder – Dhat, Koro
- F44.88 Other specific dissociative (conversion) disorder [ICD9 300.1*, 300.11] – Latah, Pibloktoq, Uqamairineq
- F45.1 Undifferentiated somatoform disorders [308.*?] – Nerves, Susto
- F45.34 Somatoform autonomic dysfunction of the genitourinary system (this may include autonomic anxiety symptomatology) [306?] – Dhat, Koro
- F48.0 Neurasthenia – Nerves
- F48.8 Other Specified Neurotic Disorders – Susto
- F68.8 Other Specific disorders of adult personality and behavior [301.5?, 301.50?] – Amok, Windigo
- G47.4 Narcolepsy and Catalepsy (including sleep paralysis) [306.0] – Uqamairineq
Some of the ICD graphs for these syndromes are as follows.
Dissociative States, Bipolar Disorders, Delusional Behavior, Narcolepsy/Catalepsy, and Social Phobia are several ICDs related to Sociocultural Syndromes in recent decades.
Mixed Cultural and Multicultural Perspectives
Cultural bound syndromes represent a set of conditions in which socioculturalism and western medical philosophy come face to face as people and doctors, both traditional and modern, try to understand the cause for an “illness” and the most effective remedial process. “Modern” medicine also bears beliefs about diseases, some which are centered on its own culture. How people with specific illnesses are treated plays a very important role in their long term progress. In the early 1800s, people with specific conditions such as epilepsy were treated like criminals and housed in jails or prisons. A few decades into the 19th century these legal practices were diminished or ceased due to the work of various humanitarian groups. In spite of these successes, however, public and professional views about certain diseases continue to exist thereby influencing greatly the life and future of people with such diagnoses. When western medical thought prevails over alternative philosophies for a disease, and as a result reduces the quality of life for these people, we have to question sometimes the values of such practices. Western societies and western medicine for example treat elders much differently than many developing countries.
- Epilepsy. Multicultural. For example “Spirit Captures you and you fall down” of the Hmong. (see 1997 book with same title). ICD 9 = 345.*
- Schizophrenia. For example Amish.
- Possession Disorder. Multicultural. Individual sense his/her body is taken over by another entity. Disturbance of consciousness, identity or memory, changes in voice patterns or speech, loss of awareness of surroundings, with a high tolerance for pain and other environmental stimuli. ICD 10 codes are F44.3 Trance and possession disorders, or F44.7 Mixed dissociative [conversion] disorders. Relates closely to fuufuyane or saka.
“Modern” medicine isn’t exact. In fact it is filled with medical conditions and ailments that could more accurately be defined as the “best fit” for the present time. This inherent trait of disease classification systems begins with the premise that the individual who defines the diseases in such a way is correct, even if his philosophy differs from others in the field.
Nosology of disease is a specialty that was developed in the late 18th century, modified in the first half of the 19th century, modified and slightly modernized following the discovery of the bacterium and pharmaceutical means for disposing of pathologies during the early 1900s, and finally developed into a system of classification much like that of today some time in the 1960s or 1970s. This late 20th century nosology is not at all “perfected”.
Even with this method of classifying disease, we are left with the culturally accepted assumption that the bifurcating system used to produce this methodology is very approporiate and most correct, and that the links drawn are “correct”. This subjectivity of human classification methods is what adds ‘cultural bias errors’ back into the classification system each time we cannot define the complete and total reasons for a particular medical condition existing. Examples of how these types of self-created, self or ethno-centered ideologies played out in the past are demonstrated by the histories of past diseases, such as the following:
- The “Divine Somnambulism” of 1800
- The “Mania” demonstrated by Jesus, a diagnosis published by French physicians ca. 1830-1840
- Agua frio, or Aire frio, an illness still experienced by some Mexican nationals today
- Iich’aa (southwestern US) and the native American philosophy
- Hypoglycemia and fasting, to MDs a concerning health condition, to others a religious experience and an important part of shamanics
- Temporary Blindness – a reason for the miracle cure of blindness?
- Nightmares/Night Horrors and “having visions”
- Tics and Tourette’s Syndrome, in the past a manifestation of nerves and nervous energy; today the consequence of personal growth and psychology, or to some, adolescent/teenage neurochemicals
One of the more interesting issues is cultural medicine today pertains to these “health practices”, reactions to stress and change, and “illnesses” experienced by patients of the United States medical care system. Equally interesting is the attraction we have to certain historical tales about these illnesses and very strange activities. Porphyrism for example was used to claims possible truths for and assign meaning to the 14th century story of vampires of Eastern Europe. Bread tainted with ergot is used to explain why towns might have had a history of being possessed by evil spirits. Epilepsy is used to define the signs of demonic possession.
The following culturally bound syndromes or behaviors important to US culture are reviewed in detail. These are examples of physicians in the current US paradigm trying to make other culturally defined interpretations of illness fit into their perspectives on health, behavior and disease.
-
African Infibulation [ICD9 729.2*]
-
Demonic Possession and the like
-
Takotsubo
-
Genetic Blood Dyscrasias
-
SUNDS
African Infibulation [ICD9 729.2*]
Note: “Genetic” should read “Genitalic”
When specific cultures migrate into the United States, there are medical beliefs and syndromes that accompany these migrations. In the case of in-migration of certain parts of the African tradition, a commonly accepted practice in parts of Africa is female genital surgical manipulation or change in the form of one or more of the following surgical procedures: clitorectomy, labiectomy, and infibulation. The end result is the removal of female genital parts and closure of the vaginal passage, symbolizing a young female’s passage into her menstruation stage in life. These surgeries, according to cultural beliefs, “prepare her” for later marriage in a virginal state; it symbolized her “promise” of not engaging in any premarital promiscuity.
These cultural practices are not accepted as humane practices by most “Western” and United States practitioners. In recent years, this sensitive sociocultural rite of passage related “health care method” has undergone intense professional scrutiny, legally as well as medically. The procedure and end result of this surgical practice are a part of ICD9 classification system, enabling this review of age-gender patterns to be completed.
The ICD9s for these processes are as follows:
- 729.2 – all of the below combined
- 729.20 – unspecified mutilation process
- 729.21 – involving a clitorectomy only
- 729.22 – clitoris and labia removal or modification
- 729.23 – clitoris and labia modification along with an infibulation process
- 729.29 – all others
The surgical processes typical of certain African societies includes a clitorectomy, labial removal and closure process (infibulation). Different ICDs are provided based on the degree to which this surgical procedures completes all three of these tasks. Although infibulation and its precursors are extremely rare events, rarely noted in the medical records along with use of the appropriate ICDs, these processes are found in exceptionally large population studies (>50M). They therefore provide us with some insight into the very poorly studied age-specific sociocultural behavior problem.
The above age-gender curves of two of these processes demonstrate the possibility of 3 age ranges of distribution for this diagnosis. These three peaks are defined as follows, based upon the history and location for the performance of this procedure:
- a) 70-100 yo-primarily individual who immigrated into this country with a history of experiencing this procedure,
- b) individuals between 25 and 50 years of age, with peaks at 25-30 and 40-50 yo, with the possibility that the older age group received this procedure in their native lands before immigrating to the United States, or as a result of social pressure after their arrival into this country, and
- c) individuals < 15 years of age, who are most likely experiencing this process either just before a recent migration into this country, or who have received this process as a result of cultural pressure to perform this act while residing in the United States.
The following symbol is a link to more on this topic.
Ã
Psychiatric or Culturally-bound?
Demons and Physicians
Demonic possession, hyperreligiosity, group hysteria, and pibloktoq or arctic hysteria are all psychological changes in individuals and people which physicians have historically tried to associate with personality disorders, and sometimes even biochemical disorders. This “branding” behavior (“the scarlet letter”) in medicine is especially true with certain disease types. History has allowed us to imagine new diagnoses for people who never seemed to fit in. This is because society forms its definitions of medical conditions or psychological states and then tries to place that person in some sort of category that is assigned based opn the most socially accepted profiles of these individuals.
During the Salem witchcraft trials for example, young women with schizophrenia, dissociative disorder, certain forms of epilepsy, tics or tourette’s syndrome, epilepsy, or even some sort of ergot poisoning had the potential of ending up in the next farm pond dead from total immersion in water. A half century later the same events recurring briefly in the Hudson Valley around 1720 led a local elderly women to be accused of practicing the same sort of dissociative behaviors accompanied due to her poor social practices and her non-traditional religious upbringing. Likewise several decades later, around the turn of the century, an old woman near North Salem was accused of many things due to her loner style of living along the mountain face facing New York; but because she attended church on a regular basis she never received the punishment that society could have given her had she been labelled a witch by the local children.
In the lower part of the Hudson Valley another young girl was suffering from a unique form of mental illness, one that made her pseudo-hallucinate whilst laying in bed, as if she were asleep. During her “events” she would recite bible passages and appear to be communicating with spirits from above. This behavior was an offshoot of an increasingly popular behavior Emanuel Swedenborg demonstrate just a could of decades earlier–whilst talking with angles visiting each of his body parts. Swedenborg’s schizophrenia was socially defined to be a consequence of his skills as a seer, and was supported more as time passed due to peoples’ curiosities about the metaphysical world. What Swedenborg then introduced to the United States by the end of the 18th century, a spirit seeker like Rachel brought into the next stage of social behaviors with metaphysics. About the same time, when the spoons started flying in Thorn house down in Fishkill, the daughter of this family was considered to be communicating with another spirit floating about in the vicinity, someone whose spirit was later found to be locked within the Thorn’s home attack in the form of an old stone that was finally discarded much later, as the daughter’s demonic possession also decided to leave this home behind.
Further north in New York State, we see this same story re-juvenated such a following when the daughters of a farming family began spirit rapping with past spirits, thus making popular once again the possibility of channeling with old time family members, making your own necessary personal connections with the matron or patron of several generations back.
All of these practices require some sort of imagination and belief to become active and effective in influencing how society looked upon such conditions as diseases or disasters for someone’s spirit, mind and personality. Many of the illnesses of this form are mostly define by cultural means. It is the beliefs of people that define whether or not a particular practice is good or bad, or can be assigned some name indiciating it is a curse or a gift. Even today, culture defines not only the type of condition a person has–good or bad–by which ICDs are assigned to a particular behavior or condition, but modern medicine is also guilty of mislabelling and misclassifying some of these conditions. Medicine in general limits its ability to categorize someone along a certain pre-approved dischotomous path of diagnostics when various unique culturally defined syndromes have to be classified using the ICD system. It is possible that the majority of the diagnoses developed using this method might even be misdiagnoses, or conditions redefined and erroneously rewritten in other words in order to best fit the category the diagnostician wishes to place someone’s behavior in.
How does a regular physician define a shaman for example? Is he simply a delusional very old man? a child who had hyperreligiosity brought about due to temporal lobe epilepsy? someone with so much grandiosity and incongruent argumentativeness that he must be a schizophrenic?
Regular medicine cannot answer these questions effectively, in the past, now or even in the future.
.
Cultural beliefs and practice such as those associated with “demons” and religion are not terms that easily found in ICD books. It is even much less possible to find mention of the words like shaman, pibloktoq, chi, vital force, or the like in the medical books. These terms help to define a set of conditions referred to colloquially in the anthropological writings as cultural syndromes. They require the culture that pays close attention to them, believe in them and support this philosophy by way on engaging in expected behavioral responses. When this “illness” is identified in accordance with sociocultural expectations, the individual experiencing these events might even have a better chance of recovery, assuming traditional treatments are properly applied. In Native American tradition, the individual going through a shamanic initiation process might be recommended to spend much of that fasting period under appropriate medical control, by a medically trained individual who is a member of that tribe or cultural group.
It is typically the case that regular physicians spend little time trying to understand these socioculturally-defined prognostical medical conditions. Doctors assign very little value to the alternative views of the world and disease related to these syndromes, and almost always resort to their standards–the use of ICDs to document the social beliefs, practices, behaviors and medical outcomes that result. This suggests that physicians in the western world can be very ethnocentric at times when it comes to understanding people and health. When an individual belief system or faith becomes an offshoot of traditional philosophies, and their practices seem to work for inexplicable reasons, the western physician lacks the understanding and ability to understand what is taking place when a person changes or gets better. A regular physician might even have to resort to his/her unofficial fallbacks for explaining such events, such as spontaneous recovery, or mind-body effects, in turn falling upon whatever pseudo-scientific theory is out there for the time being used to explain the body-to-mind events and abilities (autonomics, psychosomatically induced hormonal change, prostaglandins effect, interferons and enkephalins “natural opiates” responses, psychoneuroimmunological or neuroendocrine causality, etc).
The following are the ICDs closely linked to psychoneuroimmunological and self-induced psychobehavioral reactions to illnesses that otherwise a physician is unable to explain or define (see figure above).
.Τ.
Takotsubo (ICD9 429.83)
“Worrying or crying yourself to death”, or apical balooning of the ventricular walls in Takotsubo cardiomyopathy (ICD9=429.83). The primary theory proposed for this is weakening of the muscle wall due to: a) changes in arterial flow (left anterior descending coronary artery), b) vasospasms of this and/or other coronary arteries, and/or c) microvasculature failure within the cardiac tissue — any or all of these must be accompanied by a period of severe emotional stress resulting in autonomic effects upon the coronary arteries system. http://en.wikipedia.org/wiki/Takotsubo_cardiomyopathy; http://en.wikipedia.org/wiki/File:TakoTsubo_scheme.png. A major problem with this theory is that the age distribution of Takotsubo patients is nearly opposite of the the age gender features for traditional cardiomyopathy.
Takotsubo is a condition associated primarily with Japanese culture, and has its greatest impacts on older populations, with female patients far outnumbering male patients (see population pyramids below). A similar psychosomatic like disorder does exist in the Western World/WHO ICD system — Factitious Disorder [300.16]. By definition and description Factitious disorder is of the 300 series and is therefore a pyschologically induced condition, which does not exactly match the ICD provided for Takutshobo [429.83]. The 400 series ICDs are typically assocaited with cardiological disturbances.
It is interesting to note several similarities between these two ICDs in terms of Age-Gender distributions:
-
Incidence Peaks at ages traditionally related to socially important “elders”, with ages > 65 or even 70 years of age.
-
Female incidence for both ICDs for these older age patients is much greater than incidence/prevalence for males
.
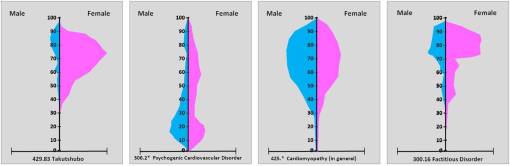
In the above images, the culturally-linked disease that is the focus of this query is on the left. Which of the other 3 best matches it’s form and distribution by both age and gender? There is a formula that can be used to quantify this overlap, but the picture makes it fairly clear which one it is in this case. Takotsubo ~ Factitious Disorder, in that both afflict older populations and are attached to some sort of emotional trigger that impacts women more than men in their older years. The anatomical-physiological theory often posed in the literature has a distribution that is the most equally distributed for the above, in terms of men versus women.
Overall age-gender distributions for these first and last ICDs displayed are remarkable similar, suggesting there is either a psychoneurological-cardiological (hypothalmic-autonomic) feature involved in both processes, or that one system affect is somehow related to the other through a third mechanism, such as stress-induced (endocrine, neurtransmitter, releasing factor?) cardioelectric response for Takotsubo, with this cardiac reaction missing from non Japanese elders. For this reason, the proposed cardiomyopathy based theory does not quite fit in statistical distribution of this disease one the age-gender population pyramid.
It is possible that the 439.83 pyramid is a result of late diagnosis, with early cases misidentified as other forms of myopathies. But the gender difference in takotshubo cannot be explained using this line of reasoning. More importantly, the more specific and unique forms of cardiomyopathy such as Obscure African Cardiomyopathy (425.2), Alcohol Cardiomyopathy (425.5), and Nutritional Cardiomyopathy (425.7) have male age peaks at either mid-life statge (45-55 yo) or the elderly stage (>70 yo). The other common cardiomyopathy–hypertrophic subaortic stenosis (425.1)–has a distribution mimicking the overall 425.* series. The same gender distribution is seen for the various cardiomyopathies, with male onset peaking in the 20-30 age group for both the Acute myocarditis (422.*) and Acute Pericarditis (420.*) series. The subacute endocarditis is not male gender weighted (421.*, this gender equality is also incidentally found for other endocarditis ICDs as well, in particualr valve-related disorders and therapeutic events).
In sum, based on age distribution alone, cardiomyopathy cannot explain how and why takotshubo’s syndrome prevails primarily in older women. The similarity of form of the population pyramid with 300.16 Factitious Disorder suggests this is very much a pscyhologically based syndrome or condition manifesting itself (psychosomatically- and/or autonomically-induced?) with regards to the cardiac musculature and perhaps conduction system. This synopsis of course is based primarily on just the 1-year age-gender distribution pyramids (and therefore could be totally incorrect).
.
JAPANESE MOYAMOYA
Source: http://en.wikipedia.org/wiki/Moyamoya_disease.
.
.Œ
BLOOD DYSCRASIAS
One of the most classical lessons in biology classes focused on genetics is the Sickle Cell disease and the impact it has on the potential for malaria. Due to a genetic condition, hemoglobin becomes capable of sickle-shpaed (curved) or forming a chain like structure which in turn forces the red blood cell to change its morphology into an elongated, bent sickle-linke form. This in turn changes the 3-dimenstionality of the red blood cell and prevents it from passing through the narrow capillary beds. This failure to pass in turn results in reduced oxygenation and ultimately the death of many solid organ structures and tissues immediately surrounding richly vascularized capillary bed regions.
The effects of malaria on blood include causing the red blood cell to sickle, thereby resulting in the destruction of cells that bear the organism responsible fo this disease. One result of this is the natural selection of sickle cell hybrids, people who carry but do not fully present with sickle cell sickling. These individuals have the chance to live longer lives in spite of the sickle cell gene, and so “select for” those who are hybrids with this condition or bear a version of the sickle cell trait that only partially presents itself.
This sickle cell behavior is different from the living and survival biologies noted for thalassemia and hemophilia victims. Thalassemics live into later years of a normal life, due to lack of organ damage induced by sickling red blood cells. Hemophiliacs have a genetic condition influencing a completely different part of the metabolic path and result in survival curves not at all similar to the other two types of conditions. They bear the greatest longevity of these 3 conditions, four conditions if we separate sickle cell carriers from those actively presenting their sickle cell trait.
We can constrast the Sickle Cell curves with those of Thalassemia and Hemophilia (all are above). There is an inveitably high mortality rate by the age of 65 years for people with Sickle Cell, be it in its active state or partially presenting itself within the bodies of carriers. The latter have a slightly longer longevity rate, and demonstrate male prevalence peaks earlier than female peaks, with females living longer and in greater numbers during their entire reproductive years period. The numerous reasons for socile cell mortality pertain to the effects of sickling cells on the microvasculature of solid organs, the splenomegaly these effects can result in at the organ systems level, and a variety of long term well localized anoxic states.
Contrast these sickle cell disease and carrier curves with those of thalassemia and hemophilia. The latter two lack a demonstration of early mortality. Thalassemia is diagnosed very early on in life (beginning in the neonatal stage). Hemophilia tends to be diagnosed a few years later in life.
.
SUNDS
Which is the above best represents SUNDS (Sudden Unexplained Nocturnal Death Syndrome)
Cultural Shock and SUNDS
After Saigon was attacked during the Vietnam War, a large number of Vietnamese upper class political leaders migrated to the United States. This migration was followed by requests for their assistance submitted by United States military leaders who assisted them in their need for asylum. The immigrants settled in just several parts of the country, usually in close association with the American military leaders who befriended them and made recommendations regarding places to settle.
Following the immigration of these families was the migration of relatives and other immediate family friends and associates. By 1979, a number of Vietnamese, Cambodian and Laotian refugees communities were established, which have ever since remained their own unique sociocultural entities. Some of the more sizeable establishments were placed in unsuspected parts of the country such as Colorado, Iowa and Oregon.
Immediately, the most important disease and public health issue during this time became tuberculosis. A number of the elders in these populations were found to be carriers.
Another common malady experienced by this population was schizophrenia, a diagnosis which remains popular to this day within these southeast Asian American communities, possibly as a result of some familial genetic pattern common to this psychiatric condition.
Several culturally-bound syndromes are also linked to this cultural group. The best known of these southeast asian syndromes is the suicidal state that acculturation and problematic adaptation processes often result in. Very young children are more capable of adapting than older children and young adults, with child bearing adults aged 35 and greater the most difficult group to provide assistance for. As these adults reach 55 years of age and greater, cultural traditions become a stumbling block for families trying to take advantage of government-based assistance. One of the chief problems these governmental programs had over the years was its ability to meet the needs of three or more cultural groups, all lumped into the same category for assistance. Aside from Laotian, versus Cambodian, versus Vietnamese, there were the Hmong emigrated from China who lived in the upper-eastern parts of this territory, a number of southeast asian cultural groups residing in wilderness settings, and the more urban adapted and often Christianized southeast asians residing close to and within the more urban settings of these countries. Such social diversity not only sets the stage for large amounts of political instability to ensue, but also makes it more likely that a number of psychological states and psychiatric and, in western society, criminal-related or developmental and academic related problems from developing in eacho of these populations. Cultural differences only add to these public health concers in that there are some basic statistics that may differ considereably between these groups. Education is found to be higher in social sociocultural groups than others. The likelihood of developing som familiarity with ESL standards is another, and even fertility rates are impacted by these southeast asian subpopulation differences. The Hmong for example have a fertility rate that greatly suprasses the same for nearly all other sociocultural groups in this country, save the Mennonites of the Pacific Northwest perhaps.
This condition was typically experienced by the precollege and college age groups, and is characterized bywhat might first appear to be anxiety or fugue-like states or a sense of social detachment and panic; these occur immediately before a suicidal act like jumping through a window is engaged in. Recent studies tend to link the immigrant illness experience to well defined psychiatric and psychological states common to western society, such as agoraphobia, social phobia, depression, avoidant disorder, and anxiety.
But like many studies of sociocultural disease, the Laotian-Cambodian-Vietnamese illness can have its own distinct causes and symptomatology. For this reason, one disease common to elders, manifesting itself primarily at night, was soon identified and linked to the oldest of the old immigrants, and given the name Sudden Unexected Nocturnal Death Syndrome (SUNDS, for which see http://www.deathreference.com/Sh-Sy/Sudden-Unexpected-Nocturnal-Death-Syndrome.html). SUNDS was identified by several authors focused on potential biological causes as a heart-realted death induced by mental anguish, mostly during the nighttime hours and during specific stages of the sleep cycle. Important contributors to the possiblity for SUNDS were sleeping during the dream state, with highly stressful behaviors acted out possibly due to the content of the nightmare or nigth horrors being experienced. These problems in turn resulted in cardia dysarhythmia according to the physicians researching this condition, thus resulting in nocturnally-induced cardiac dysarrhythmias and death. (See http://www.mja.com.au/public/issues/177_08_211002/mck10856_fm.html)
Can SUNDS be detected within an ICD data pull process?
The first problem with pulling SUNDS related conditions is the variability in potential ICD realtionships developed for this culturally-bound illness. To date, the following ICDs already assessed may have some relationship with how these cases get coded in the medical records. No SUNDS ICD exists for ICD9, although it is possible that ICD 446.7 Takotsubo’s disease is incredibly close to the Hmong-Laotian syndrome, including the cardiac physiological events related to Takotsubo’s disease. The strong tendency for Tak0tsubo’s syndrome to influence women over men suggests a sociocultural/psychological component, which if this is true may help to explain the apparent gender difference the other cultural groups with SUNDS may be demonstrate (lesser female, more male elder related events were noted clinically).
- 290.* Dementias
- 300.* Anxiety states
- 300.02 Generalized Anxiety Disorder
- 300.1 Dissociative Disorders
- 300.11 Conversion Disorder
- 300.13 Fugue
- 300.14 Identity
- 300.16 Factitious Disorder
- 300.21-.22 Agoraphobia
- 300.23 Social Phobia (301.7 Antisocial)
- 306.2 Acute Physiological Malfunctions of the Heart due to Mental Factors (306.8 bruxism, 306.6 endocrine)
- 307 Sleep Disorders (307.45 Circadian, 307.46 Arousal)
- 307.46 Sudden Affective Disorder (SAD)
- 308 Acute Reaction to Stress
- 309. 4 Emotion and Conduct Adjustment Disorders
- 309.21 Separation Anxiety
- 309.29 Culture Shock
- 309.81 PTSD
- 309.* Adjustment Disorders
- 309.1 Prolonged Depression
- 310.1 Personality Change due to . . .
- 427.5 Cardiac Arrest
- 446.7 Takotsubo’s Disease (see http://en.wikipedia.org/wiki/Takotsubo_cardiomyopathy)
- 452.2 Obscure Cardiomyopathy of Africa
- Brugada Syndrome or Asian Pseudo-RBBB (http://cvgenetics.med.nyu.edu/genetic-conditions/brugada-syndrome; http://www.cigna.com/customer_care/healthcare_professional/coverage_positions/medical/mm_0052_coveragepositioncriteria_genetic_testing.pdf)
SUNDS is most often linked or related to the above 3 ICDs. This study (and my 2000-2003 field studies for a Quantitative/Qualitative Analysis Certification program) again demonstrate that, like Takotsubo, SUNDS has a tendency to behave most like Factitious Disorder, but with a more equally distributed gender-related pattern for elderly populations.
.
£
OBSCURE AFRICAN CARDIOMYOPATHY
.
There is a mindbody relationship in cardiomyopathy that is worth noting. The following schematic was produced by a researcher attempting to define the causology of cardiomyopathies.
.

http://circ.ahajournals.org/content/113/14/1807.figures-only; see also http://en.wikipedia.org/wiki/Cardiomyopathy
Barry J. Maron, MD, Chair; Jeffrey A. Towbin, MD, FAHA; Gaetano Thiene, MD; Charles Antzelevitch, PhD, FAHA; Domenico Corrado, MD, PhD; Donna Arnett, PhD, FAHA; Arthur J. Moss, MD, FAHA; Christine E. Seidman, MD, FAHA; James B. Young, MD, FAHA. AHA Scientific Statement. Contemporary Definitions and Classification of the Cardiomyopathies. An American Heart Association Scientific Statement From the Council on Clinical Cardiology, Heart Failure and Transplantation Committee; Quality of Care and Outcomes Research and Functional Genomics and Translational Biology Interdisciplinary Working Groups; and Council on Epidemiology and Prevention. Circulation. 2006; 113: 1807-1816.
Even though some of the conclusions these authors present have already been questioned, their overall research methodology is worth noting due to its similarity with the Health Belief Model utilized by many health education/health promotion researchers and employees.

The above flowchart for cardiomyopathies can be integrated with the Health Belief Model. For African cardiomyopathy(425.2) , the age-gender distribution most closely resembles nutritional deficiency cardiomyopathy (425.7). Given the age-gender distribution of Takatsubo versus cardiomyopathy, it appears tak0tsubo is primarily a psychosomatic condition induced primarily through personal perceptions, beliefs and knowledge, more so than a result of a biological phenomenon related mostly to some histological or cellular defect in cardiac tissue. There is no other way to explain why women within their older years manifest this condition so much more than men.

Â
[To be Continued]
.










