Osler Library image of William Aitken (1825-1892)(http://digital.library.mcgill.ca/oslerprints/fullrecord.php)
.

.
In 1872, the above third edition of The Science and Practice of Medicine by William Aitken was published. This book contained a colored fold-out map depicting the author’s interpretation of diseases of the world.
The idea of global disease mapping was now 80 years old, with the successful production of global disease maps depicting endemic and epidemic regions about 50 years of age by now. This much shorter history of the existence of a global disease map was in part due to the lack of interest in global concepts regarding disease until some time from about 1795 to 1800 perhaps, but more than likely was due to the rapid advancement of Asiatic cholera out of Bangladesh and into western Europe between 1810 and 1817. Until Asiatic cholera began behaving more like a disease that was becoming pandemic in nature, the diffusion of more understandable diseases like malaria in various forms, yellow fever and typhoid seemed to be dominating the medical topography and climatology writings. Asiatic cholera added demographics and sanitation to the list of primary causes for recurring periods of high mortality.
William Aitken’s biography includes the tale of a doctor in the military to which can be added several career changes in life and several important accomplishments. One of his largest, his few and his final publications, The Science and Practice of Medicine is an example of this.
Dundee Royal Infirmary, 1865
He was the eldest son of father William Aitken, Sr., and was born in Dundee, Scotland. After competing high school he became an apprentice under his father who was a physician practicing at Dundee Royal Infirmary. William Jr. attended the University of Edinburgh beginning in 1842, completed his education in 1848, and during his apprenticeship penned a theseis entitled ‘On Inflammatory Effusions into the Substance of the Lungs as modified by Contagious Fevers’. This was later presented for which he received a gold medal.
Professor and Military Epidemiologist William Aitken Junior
Upon completion of his medical training, William Aitken Jr. began work as a demonstrator in human anatomy at the University of Glasgow serving under Prof. Allen Thomson. During this time he also worked as a pathologist for the Royal Infirmary until 1855, when his skills in epidemiology were tested for the first time in the field as he was sent to the Crimea to serve as an assistant pathologist under Dr. Robert S. D. Lyons.
The Commission had just been appointed to investigate the diseases striking troops in the field in the Crimea (Parl. Papers, 1856). It was William Jr’s responsibility to investigate the situation. The war with Russia at the time had resulted in typical losses, until the battles at the Crimea, when dozens of soldiers were dying per day during the lulls between battles, followed by hundreds to more than a thousand deaths incurred during each of the two major skirmishes that resulted. The majority of deaths at the Crimea occurred during the second skirmish (location?), and the question became ‘did these soldiers die due to poor training, poor health or simply their constitution as it related to the local environment and topography?’. Such was a typical medical geography question asked by physicians like William Aitken around 1855/1857.
William Aitken’s study resulted in an article published in 1859 in Medico-Chirurgical Transactions entitled “On the Effects of Twelve Weeks’ Residence in Bulgaria (during the months of June, July and August, 1854) on the Subsequent Health of the British Troops in the Crimea”, (vol. 14, pp. 179-199, 1 chart, published by Royal Medical and Chirurgical Society of London). He sent his essay for review for publication to William Jenner (1815-1898), the Physician-in-ordinary to the Queen at the time. [See L. S. Jacyna, A Tale of Three Cities (London 1989) for more.] In this article, Aitkens drew the following conclusions from his study:
. . . the inactive residence in Bulgaria during three months exercised a persistent pernicious influence upon the health of the troops in the Crimea; and which contained to make itself felt, more or less, throughout the campaign. but more especially during the first seven months; nay, it may even now be doubted whether many who passed through the campaign in Bulgaria are as well able to resist disease and sickness as their constitutions were wont to do.
Aitken’s observations led him to define three periods of this war:
- the period of residence in Bulgaria from June to September of 1854,
- “the period of the first seen months’ occupation in the camp before Sebastopol during which the losses sustained by the allied troops from disease alone, have not been suprassed by any army in the history of the world.” and
- “The period after April 1855, characterized by a gradual return of the army to a state of health and efficiency equally unsurpassed.”
This event was a repeat of a prior impact on epidemiological history during a war that was experienced by Napolean’s army. Following such a military event that took place around 1800, the following map was produced depicting the effects of disease upon the army as it marched back to its homelands.
(See wikipedia page for more on this)
Time and fatigue seemed to be the major cause for deaths related to the Napolean march, but life in the camps and battlefields were no doubt the major reasons for this fatique, and even though these troops were moving fairly regularly from region to region, sanitation was a major issue at most military camps in general for much of the last century. Too long a stay next to flat marshy lands made for unhealthy living conditions due to diarrhea followed by dysentery, the onset of infectious diseases brought about by close living conditions, and the onset of epidemics on a regular basis due to the various kinds of fevers that existed in these esttings, such as the fevers related to typhus, or in the worst of circumstances malignant (yellow) fever, varous forms of intermittent, remittent and ague, and what had come to be known as the malaria-chlorosis.
One of Aitken’s most important questions was what was the cause for all of these “pernicious endemic influences”. A number of potential causes were already published in a Parliamentary Paper No. 247 (p. 253) circulated in 1855. In this paper, the author Dr. Mapleton defined the following possible causes for these diseases: the “sickliness” of the soldiers, their “used up” nature, their general weakness and poor bodies which “lost flesh rapidly”, their depressed spirits due to lack of military engagement, their long drills and “bad and unwholesome tents”, the “great heat during the day, followed by cold and dewy nights, fog, and evening and morning mists”, “great range in temperature”, “sour brown bread and ill-assorted food”, and the lack of strength in these men, all of which he claimed led to a state of anaemia or malaria-chlorosis. Add to this the consequences of such a poor encampment, their inability to march after all of these events, and in Mapleton’s interpretation of events we have the deciding factor for many of those able to serve during the wartime period.
These conditions no doubt resulted in a staggering number of deaths during all stage before and during battle. But in Aitken’s interpretation of these events, three were two distinct troops of soldiers whose diseases were not differentiated from one another. There were the initial troops who operated in Bulgaria and then merged later with other soldiers to fight in the Crimea. Then there were the more recent recruits brought in solely for the Crimean battles. Aitken’s goal was to differentiate the losses for these two groups of soldiers to determine if any significant differenes existed in how the final events led to all of their deahts. The results Aitken produced from this study demonstrated that what he called the Ex-Bulgarian troops were already susceptible to disease and death in the encampments at the Crimea, even before any war related activities commenced. this set the stage for their weakness that resulted in their subsequent deaths on the battlefield, their weakness and inability to defend themselves against a stronger more durable enemy.
Aitken’s evidence for this was as follows. The march to the Crimea or “flank movement” took just 22 days, during which 5053 men are said to have died or made seriously ill. In the first battle 353 were lost and 1867 wounded. The remaining 2237 now terribly weak and ill went on to the next battle, where nearly 600 were the lost. The questions this led Aitkens to ask were ‘did the march make these soldier’s weak.’ or ‘was it the environment they were in?’
Aitkens made an aggressive use of math to prove his point that the causes for these deaths depended upon the sources for those who died—the Ex-Bulgarian group who fought in Bulgaria before removing to the Crimea, and the Crimean group which served only during the Crimean War. Using percentages of admissions for soldiers from each of these two groups, Aitken was able to demonstrate that the Ex-Bulgarian group experienced more morbidity and mortality than the Crimean group. Aitken based these claims on their disease types. Diseases like cholera, typhus and fevers were shown to take place is less sanitary settings and scorbutus (Vit C depravation) was the most common cause for death associated with the “used up” condition. The ability of the diseases from unsanitary environments to spread to new settings was proven by the spread of these diseases between battles by the Bulgarian group. All of this was in turn blamed on the unhealthy nature of the place of residency for the troops in Bulgaria, who resided adjacent to marshy or paludal settings.
A major result of Aitken’s work was the implied need for sanitary police whenever military camps were established. Sanitation had finally become the primary focus of camp related health, and this wasn’t due to just a classical interpretation of disease and how it originates due to local topography and climatology. Aitken’s conclusions were drawn based upon his belief in the zymotic theory for disease.
This study was performed during a time when place and disease were already felt to be strongly correlated. The reasons for this correlation were unclear and forever changing due to lack of sufficient data and sufficient understanding of diseases and their potential causes. The zymotic theory for disease provided a new interpretation of disease causality that focused on the newest understanding of chemistry and disease. The toxin theory for some diseases was once again prevailing in the literature and the zymotic basis for the production of these toxins developed as an explanation for such events.
The fact that a long inactive residence by troops in Bulgaria could facilitate their passage of any disease to the Crimea was a controversial claim Aitkens was making. Yet this explanation explained the math results behind Aitken’s statistical review of the cases and mortalities for each of these troops and their various epidemics over the months and years. Aikens offers the following detailed description as to how and why such a regionally born disease behavior can result in new topographic disease patterns.
From these details I think it is very clearly apparent that the long inactive residence in Bulgaria consituted a very prime element of causation in the induction of disease in the Crimea; and that its influence long continued to be felt as an influence of a most persistent and pernicious kind, although it is well known that while in Bulgaria many would not say they suffered from any well-defined disease to which a name could be given. They became, however, the subjects of impaired health, which showed itself by imperfect digestion, flatulence, diarrhoea, loss of muscular strength, sallow looks, morbid susceptibility to external impressions of cold or heat, with night sweats, loaded turbid urine, and an unhealthy state of the cutaneous and mucous circulation, but without any manifest local disease–a form of anaemia to which Vogel has given the name of malaria-chlorosis. Such a condition frequently came under my own obserrvation while at Scutari, and although in such caess an apparent restoration to health is effected, yet the constitution is so impaired, that the application of any external cause, such as wet, cold, privation, or fatigue, at once brings about the edvelopment of some zymotic disease, such as fevers, dysentery, diarrhoea, cholera, scorbutus.
It is important to note here that there are points made by Aitken’s writing in terms of our current understanding of disease. The first is that chlorosis or chlorosis-like diagnostic events and malaria were merged together by Vogel into a single diagnosis malaria-chlorosis. The second is that a disease that today we know is completely nutritionally based, scorbutus, is merged with diseases that today we know have more of an infection related causality, like fevers, dysentery and cholera. To these events can be added a third supposition, not directly made by Aitken, the fact that there are the more simplistic symptoms that seemed to resemble precursors to the devastating epidemics that at times prevailed, problems due to simple diarrhea and other simpler causes for fever, also of zymotic origin.
During the second half of the 19th century, zymosis was a go-between for the older fermentation theory for disease, which states that chemical reactions occur that are responsible for a given condition, and the infection theory for disease, which precedes the bacterial theory by only a slight difference in interprtation and meaning. With zymosis, the cause is not identifiable and visible, and interpreted as a poison, chemical or toxin. With bacterial theory, the cause is visualized under the microscope and is a physical object that is easily defined and able to be duplicated upon inspection of other cases.
The zymoses responsible for these diseases were very much a result of a place. One can visualize this cause and effect description as defining place to be a cause due to certain places known to have certain unique features and differences from other nearby or visibly similar places. Topography is the means by which physicians began their interpretation of healthy places versus unhealthy places. In the case of fungal diseases during this time, one writer clearly understands the differenes between the sunny side and shady side of a mountain when it came to pathogenesis, or the upwind side of a creek or river versus the downwind side. In the first case, sun and climate play a role in the ecology of the disease setting, in the second case, the condition of the air before versus after it crosses a water body is a deciding factor for pathogenesis. Most importantly, note that With a belief in the zymosis theory, all of this logic can be surmised without knowing an actual organismal or chemical cause for a disease.
Aitken’s geographic interpretation of this endemic disease pattern led him to compare the Crimean experience with other similar events that took place historically in “the Lower Alps, in the Lower Roman territory and Maremma of Italy, the Carolinas and Virginia of North America, the great district of the Sunderbund near Calcutta, as well as many other similar localities.” Dr. James Johnson, his colleague, noted that people who occupy the malaria districts demonstrate “a range of disorders produecd by the poison of malaria.”
This study was a matter of the vitality and longevity of British troops occupying a part of Eastern Europe during the Russian War. Even changes in residency with such a region, like from Bulgaria to the Crimea was noted to have an impact on the survival of the soldiers. Aitkens would later visualize these observations as part of a map of Europe, the topic for this page.
Following his service as an epidemiologist, William Aitken took on a position as a professor of pathology for the new medical school in Fort Pitt, Chatham in 1860. Soon after, the first edition of his The Science and Practice of Medicine was published in London, which over the next few years underwent improvements in presentation and content, until the most successful third edition was produced by 1868.
My copy
Disease mapping was a natural product of the philosophy of disease that Aitken had developed. By the 1860s, the zymotic disease theory was popular, a belief system that remained active well into the end of the century. As the bacterial theory for disease came about in the late 1870s and its undeniable proofs inarguably demonstrated a decade later (the older generation had to die off basically), the zymotic disease became the common cause related to anything could not easily have some microorganism attached to its cause.
In some of the first 20th century maps of disease we see diseases of zymotic origin referred to as such. This only meant that the cause for disease had not been established, not that its spatial behavior was misunderstood. With the maps produced during this time (1890-1910) we can tell that the diseases were finally becoming well understood as public health related topics of a geographical nature. In due time, the old teachings of regionalism that lacked zymotic evidence and came to be interpreted as more behavioral and eve Mendelian and deterministic in nature, were dropped from the disease maps, as disease maps came to represent single pathologies each with their own unique demographic, topographic or climatic causes.
The History of Disease Mapping
To review Aitkens 1880 map of disease, it helps to review some of the more important maps that existed the century before.
The geography of disease became a primary theoretical discipline in medicine by the 1790s. Whereas 80 years earlier it was fighting with numerous other philosophies out there about disease, by the end of the century we paid less attention to the inner and often less controllable fatalistic, predeterministic causes that prevailed throughout much of the religio-medical years of western European medical philosophy history. Knowing the elements of nature taught us that we could protect ourselves from ailing winds or too much sun, and that we could develop habits that expose us to much healthier foods and beverages, climates and topographic settings, or that we could select the healthiest places for us to reside or vacation in as valetudinarians searching for a more healthy and complete life.
It was during these years that travel increased considerably, and the importance of knowing and recognizing epidemic and endemic disease patterns became important. The three ‘zones of health’–the arctic, temperate and torrid–were well known due to their very ancient Greek origins and continued promotion ever since. Exactly how these related to climate, topography and the places in which we live and work, in the grand scheme of things, became more popular with each passing generation from this point on in medical history.
The first such map is recognized to be that of L. L. Finke from his Versuch einer allgemeinen medicinishe-praktischen Geographie, which translates as ‘Essay on General medico-Practical Geography’. (3 vols. Leipzig, Weidmann, 1792-5.) [see also Frank A. Barrett’s Finke’s 1792 Map of Human Diseases: The First World Disease Map?, Social Science and Medicine, 2000, vol. 50, pp. 915-921.] [REF]. It is important to note that even though Finke is known as the first disease cartographer, he actually lacked a map in his initial publication. (A similar history is demonstrated for John Snow’s map history as well; he made his discoveries prior to 1850, but didn’t published a proof for his theory as a map until several years later.)
This very early medical climatology-topography description detailed by Finke’s work is perpetuated by the immediate writers following in his footsteps. A number of these maps focus primarily on occupied parts of the world, not the world as a whole, and their detailed disease notes focused on known pathologies already present and endemic to regions, engaging less activities and writings devoted to mapping the migration of epidemic diseases. The following preliminary map of these regions I developed after perusing this Finke’s book demonstrated the following limited distribution of discussions about disease geography, and noso-geography.
[INSERT MAP]
.
As noted elsewhere on this site, it was the yellow fever epidemics that struck harbor of New York that resulted in the first disease maps produced by an American physician in the early 1800s, Valentine Seaman. Even though the knowledge base for this map was derived pretty much from 1797 events that took place in the local epidemiological history of southern tip of Manhattan Island in New York, this map was sufficiently published in 1805 by the Medical Repository magazine of New York.
The yellow fever epidemics served as an indicator to physicians and scientists about the need for a better review disease patterns and behaviors through the use of mapping in combination with natural history knowledge and skills. For this reason, science as a whole took on such a task in detail once the second major series of epidemics involving Asiatic cholera made their way out of their endemic regions near what is now India, heading westwards toward Europe. This disease changed from endemic to epidemic in nature when it struck Western Europe for the first time in 1817. This led to the first production of a map, onto which notes, not cartographic symbols, were added to described these endemic and epidemic patterns. This map was produced by Dr. Christian Friedrich Schnurrer’s (1742-1822) and focused on the cholera epidemic.
Charte der die Geographische Ausbreitung der Krankheiten, by Schnurrer, 1822/9.
Schnurrer’s map promoted the idea of disease mapping more than its method. On this map, disease names are noted over their areas of influence, but with minimal large areas defined along with the expected latitude features related to disease like the Equator and Tropics of Cancer and Capricorn.
Twenty years later, in 1842, Adolph Muhry began developing his philosophy of noso-geography, a combination of the studies of nosology or knowledge of disease taxonomy in relation to cause and effect. To accomplish this he performed a detailed study of disease geography which later his production of one of his first disease maps printed in 1856 as follows:
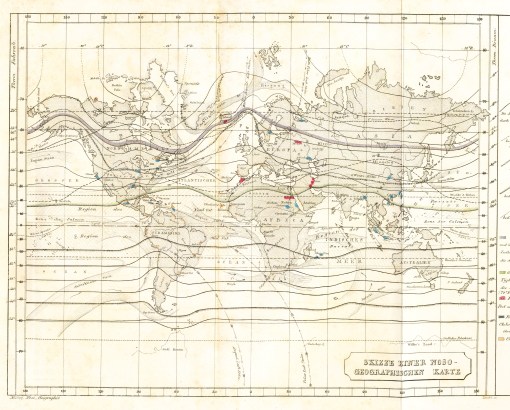
Muhry’s Global Disease map, 1856
[click here for a review of Muhry’s map]
1848, another German medical cartographer, Heinrich Berghaus, produced his disease map, the content and presentation of which helped define how subsquent maps would be produced by British medical cartographers.
.
Berghaus’s Global Disease Map, 1848 (link to map, link to page)
Berghaus’s and Muhry’s works were followed by the important work by Alexander Keith Johnston, whose 1856/7 map on the global distribution of disease was probably first presented in one or more semi-formal gatherings within the profession locally, before being presented and then published in his report on the same one year later as a part of his Physical Atlas of Natural Phenomena (1857). [Note: A.K. Johnston’s map also has a page devoted to that part of it on North American medical geography; see also the extensive site on maps www.davidrumsey.com.]

Johnston’s Global Disease Map, 1856/7
.
Realms of Men
The major differences between the above three maps and Aitken’s map is that Aitken’s demonstrates a considerable degree of fine tuning and concentration on numerous smaller regions. The large area details for Aitken’s map still pertain to the three primary “zones” of the world, namely the arctic or frigid, warm or temperate, and hot or torrid zones, but the small area details are now much more helpful. Colorization of the map and better isolines and isopleth differentiation are now the standards, enabling basic endemic and epidemic disease pattern information to be displayed in a more useful fashion.
Aitken uses the term hygiology or the scientific study of hygiene in relation to health as the basis for this conclusions about disease. By the time his map was published, ca. 1876, seventy-five years have passed since the first observations of mosquito behavior and disease were published within the American medical writings, yet, no conclusions have been made linking yellow fever and other diseases like Dengue and Malaria to the mosquito populations.
It is perhaps the seemingly omnipresent nature of the mosquito that may have prevented such a conclusion from being drawn. The ability of mosquitoes to thrive in fairly small aquatic settings made seemingly marsh-free regions capable of generating illness where no obvious source for the infection exists. This invisible nature of the miasma made it difficult for physicians to learn to associate these various diseases, with their varying symptoms, different reactions to the climate and weather, and varying periods of endemic outbreaks in the year, made it almost impossible in fact for such a conclusion to be drawn, as Aitken’s writings demonstrate to us.
Due to this lack of understanding, Aitkens like most other physicians were now favoring the zymotic theory for disease. This philosophy would be maintained and even prevail at times when we visualize the meaning of where he places some of the diseases on his map.
About the same time that Aitken’s map was being produced, Lister had made his discovery of the value of carbolic acid in preventing certain infectious problems from developing following surgery, and scientists were beginning to make the transition from the much broader “animalcule” based interpretation of some diseases with these possible microbiological links to the bacterial theory.
By the 1880s, this made it possible for physicians to define a visibly proveable cause for their theoretical pathogen “miasma” or “zyme.” Now it was a matter of time before the old time pre-bacterial theory thinkers were passed by their younger counterparts more willing to believe in the new disease theory. From about 1883 to 1890, we find evidence for this in the state and county medical association meeting minutes, as new requirements were being developed and passed for one to remain a physician in practice. This final boot to the old fashioned medical topographers and medical climatologists managed to also result in the much reduced focus on geography and medicine typical for most of the nineteenth century in medicine.
As the end of a century neared during the 1890s, this separation of healers into those who believed in the bacterial theory and those who didn’t to form their own separate professional boards and associations. Dr. William Aitkens was also now in his final years of service to his profession and his life in general. His death in 1892, twenty years after producing this medical geography-disease realm map, marks the final period in disease mapping as a regional, and to some deterministic pattern of depicting health and disease patterns. With the advent of microbiological research, the focus turned to the smaller organisms and their unique natural and human ecological behaviors. Future maps were now becoming more like those of modern epidemiological settings, with a focus on the vector, host and microbial pathogen, in relation to the individual human being, and on occasion, more than one individual in a fairly specific type of living or occupational setting. Spatial epidemiology was now a complex specialty focused mostly on the microcosm, and no longer the macrocosm.
.
.
Note latitudinal-based borders for color pattern (torrid, temperate, frigid zones). Diseases defined on the map are hard to read, but include beriberi, dysentery, leprosy, and of course remittent and intermittent fevers (see close-up of this section below)
.
.
More of the diseases defined. The well-inland nature of Small Pox is noted in several other maps on this site (see Mexico). Indigenous cultures were the most susceptible and their regions of occupation were typically blamed. Cholera tended to follow the ship and overland routes inland into Hindoostan.
.
.. . .
article continued at this GOOGLE BOOKS LINK
…..
AITKEN’S MAP
The following are from my copy of Aitken’s map in volume 2 of the stated book. The era of these printings is unfortunately part of the acid rich period in book binding. Some of the worst books, if they still exist today, come from the 1880s into the 1890s. The closer to 1900 the book is, the more yellow and brittle its pages become. In addition, books printed in other countries during these two decades tend to be more acidic than those from the American press. Their inserts, fold-outs, specially produced pages are all exceptionally fragile. Fortunately, the Aitkens book is from the earliest part of this acid paper printing period, so the earlier versions are not badly damaged or decaying.
The sepia tone of the pictures of this map and book is in part due to the tannic acid content of the paper, but also due to indoor lighting for the workspace in use.
Below each section displayed is a listing of the diseases Aitken’s added to the previous maps published. Other comments may be added as well.
.
.
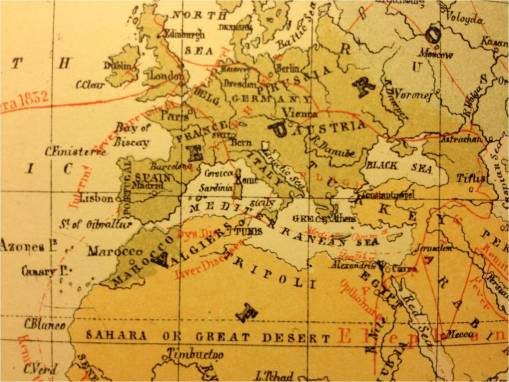
Aitkens added Cretinism, Dysentery, Ophthalmia
.
Aitkens added Liver Diseases by Tripoli; note also the mention of healthy places.
.
Note the narrowness of the temperate zone band on this map.
.
ditto
.
Intestinal worms, dysentery, and beri-beri are new.
From Papua New Guinea south into Australia, the regions become very healthy
.
.
.
Pestilential Diseases making their way towards Madagascar? Note similarities betweeb Cape of Good Hope area and England according to this map. Elephantiasis and Rheumatism are new additions. Guinea Worms on the coast of West Africa is also important to note. Animalcule/organismal geography is becoming an accepted hypothesis for disease to some. Felkin will later write and entire booklet based on this theme for endemic-epidemic diseases about 10 to 15 years later (to be covered elsewhere).
.
.
.
Ignoring the history of its additional settlement by European criminals for the moment, this setting is very healthy, with just a little problem with fevers. Rheumatism is prevalent, however. Cholera behaves more in accordance with its endemic behaviors in this part of the world. It fails to infect people readily once the tropical-temperate zone border is crossed. Its last outbreak region on this map is in and around Java.
.
.
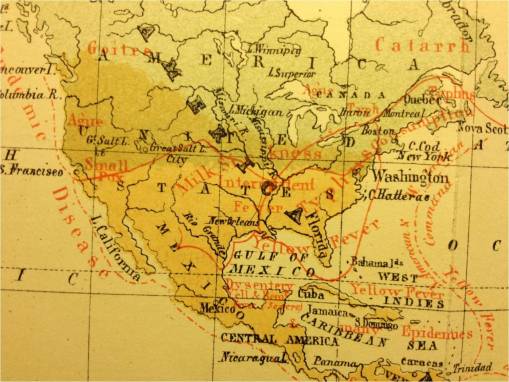
Most of the above are from previously published North American disease geography maps. (This will be reviewed on a separate page.)
.
.
Ague has finally reached the west coast in the Pacific Northwest. Otherwise, this is a very health region acccording to Aitken. Oregon Trail medical history tells us a lot more about the geography of diseases in this part of the country (see my work elsewhere on this). The Sandwich Islands are interpreted as Tropical. Notice there is no mention or inference of a Pacific Rim or trans-Pacific (via Sandwich Islands) disease migration route on this map, nor was this mentioned much in any written materials.
.
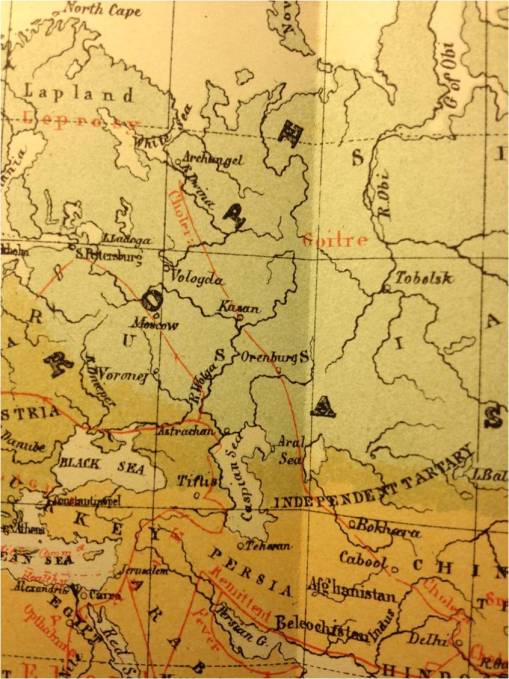
These details about Iceland and Greenland are unique additions for this map.
.
Aitken reviews the same diseases as prior cartographers, but has more details about their distribution.
.
Notice the large penetration of South America by Small Pox. Elephantiasis is an addition as well.
.
Scarlet Fever and the related Scarlatina is a very new addition to these global disease maps. It is noted with Dysentery and Small Pox. These concur with the breakdown of diseases into the categories proposed by the zymotic theory (noted above and reviewed more extensively elsewhere). Immunization practices are now a standard and there are 6 to 7 diseases being vaccinated against–including scarlet fever, diphtheria, measles, and the pox. The Small Pox tends to be found on this map in distant rural settings. Other infectious diseases were more commonly experiencing outbreaks in rapidly growing towns and heavily populated areas. The differences between childhood versus adult diseases that were infectious were not completely understood as of yet; thus this lumpging of scarlet fever and pox with dysentery.
.
.
.
APPENDIX
Wikipedi (8-30-2012)
Sir William Aitken (1825–1892) was a Scottish pathologist.
Aitken, the eldest son of William Aitken, a medical practitioner of Dundee, was born there on 23 April 1825. Having received his general education at the High School, he was apprenticed to his father, and at the same time attended the practice of the Dundee Royal Infirmary. In 1842, he matriculated at the university of Edinburgh, and in 1848 graduated M.D., obtaining a gold medal for his thesis ‘On Inflammatory Effusions into the Substance of the Lungs as modified by Contagious Fevers’. In October of the same year he was appointed demonstrator of anatomy at the university of Glasgow, under Allen Thomson, and also pathologist to the royal infirmary, which posts he held up to 1855. In that year he was sent out to the Crimea under Dr. Robert S. D. Lyons as assistant pathologist to the commission appointed to investigate the diseases from which our[who?] troops were suffering (Parl. Papers, 1856). In 1860, he was selected for the post of professor of pathology in the newly constituted army medical school at Fort Pitt, Chatham, which was afterwards removed to Isetley. This appointment he held until April 1892, when failing health necessitated his retirement, and he died the same year on 25 June. He had been elected F.R.S. in 1873, and was knighted at the jubilee in 1887. In the following year, he received the honorary degrees of LL.D. from the universities of Edinburgh and Glasgow. He married in 1884 Emily Clara, daughter of Henry Allen, esq., who survived him. His portrait by Symonds is at Netley Hospital.
A Biography also appears in the public domain at: “Aitken, William“. Dictionary of National Biography. London: Smith, Elder & Co. 1885–1900.
Third London Edition
London; Charles Griffin and Co. 1864., 1864. Hardcover. Book Condition: Very Good. 3rd edition, revised and portions re-written. 8.5″ x 5.5″. xxxvi + 939pp. xxxvi + 993pp, illustrated + foldg map. Light foxing to eps and prelims. New title labels, else, very good hardbacks in contemporary half calf with raised bands and faded, gilt decoration.
Second America Edition information:
Philadelphia: Lindsay & Blakiston, 1868. Second American, from the fifth, enlarged and carefully revised, London edition., 1868. Hardcover. Book Condition: Very Good. 2nd Edition. 2 Volumes. With Large Additions by Meredith Clymer. Thick 4tos. xxxii, 33-927 pp. Illustrated; xli, 33-1079 pp. Illustrated. Both volumes bound in original brown cloth. Ex library with minimal markings (“received” stamps front free endpapers and “duplicate” stamps title pages). Spines sunned with some wear at the spinal extremities, occasional light damp stain top edge not affecting text, very good.
Other historical sources:






























Leave a comment