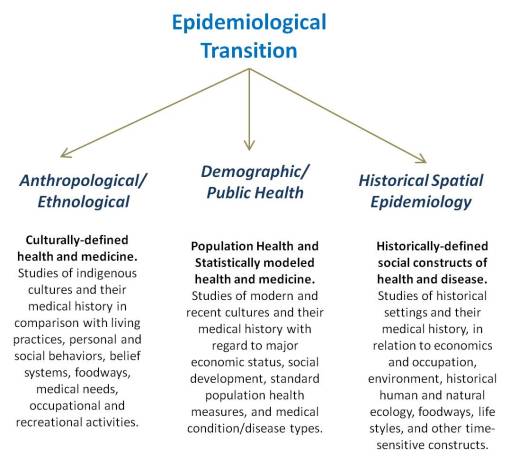
Introduction
There are two approaches to reviewing socioculturalism and health in the United States. The most common, a traditional interpretation of this topic, is to review the different groups noted to exist in the overall health system based on the US Census method of subdividing people into sociocultural communities. Each of these sub-populations is treated independently and reviewed as if it exists in a sterile observational setting. Once this sociocultural medical system is better understood, researchers then try to understand how other cultures in the same system influence the study population and vice versa.
These reviews of cultural medicine in the United States tend to be engaged in and presented as some ethnological or anthropological study of the observations. Researchers interject just a little bit of ethnocentricity however into how they engage in this process. With each step taken to integrate such a study into the standard medical practices of the country as a whole, the more ethnocentric this study becomes.
When ICDs are added to such studies, this potential problem with ethnocentricity is at its worst state. Still, such a biasness is anticipated, accepted and considered the norm for most medical and public health studies. Researchers argue that United States medical practice (or for other countries, their own governmentally approved system) is the best way to engage in this process, and uses this standard medical system’s “guidelines” to judge the cultural practices being researched.
As noted in several other pages at this site, time plays an important role in how the medical system defines its standards, norms and accepted healthy outcomes. As these preferred outcomes become less physical in nature, as many ailments or conditions are, the more ethnocentric the research results become. Researchers like to apply western medical thinking to their work whenever it deals with something psychological or psychiatric in nature. The more fluid of researchers and thinkers will accept the options that various mind-body processes are involved in the culturally-defined health promotion/health maintenance programs. The less physical the ICD-defined condition is, the more culturally-biased this study becomes. It limits its outcomes to the western medical set of ICDs out there for diagnosticians to based much of this work upon. The importance of culture in turn is forgotten.
For example, the most culturally-centered evaluation of health status pertains to mental health. Many mental health conditions are in fact very subjective in nature and based on theories or hypotheses that are only valid for the time period they are employed as a part of the ICD system. In 1800, a divine somniferant state of consciousness and thinking was defined as a normal emotional state someone goes through, by expressing behaviors and activities today referred to as hyperreligiosity, emotional detachment, obsessive compulsiveness, or psychologically-induced somniferant states. Even these modern terms for the person who has claimed to come to grips with his/her religion is very much culturally-defined, and culturally-biased.
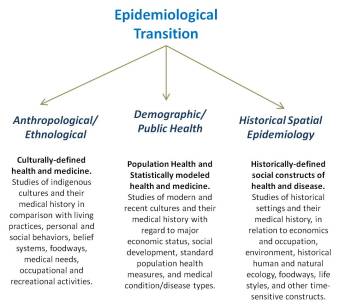
Epidemiological Transition
One of the most popular ways for conceptualizing and making sense of population health makes use of epidemiological transition (ET) theory. First defined in 1976, epidemiological transition was a concept independently developed by experts in population health statistics. Prior to the development of this concept was the sequent occupance theory of 75 years earlier, a concept pulled together by classical geographers teaching in the midwest. Between the time when sequent occupance was defined and modified several times in geography history, and the more recent definition of epidemiological transition, sequent occupance [SO] theory underwent several applications that helped to set the stage for the logic required for the development of the ET theory.
.
Due to their histories and manners in subjectively defining (to some judging) the end results of a study, the applications of ET and SO are very different. ET is the more commonly accepted paradigm, not due necessarily to correctness, but more due to familiarity with the concept and its history in United States educational system. For a variety of culturally-defined reasons, United States students were hesitant, slow and unwilling to accept the teachings of geography, especially during the third and fourth quartiles of the 20th century. During this period in science and education, the social and natural sciences were separated from geography and treated as highly scientific specialties. The subject of Geography during this time lost any scientific value it may have possessed, being treated and qualified as a study of unique paradigms and teachings related to social systems and places. Several unique philosophies were generated in large part due to the geography profession, and several beliefs which are today considered taboo. Geography is often associated with the belief in determinism, which stated that place played a major role in defining the anthropological features, nature, intellect, trypes of living practices, and long term fates of particular cultural systems growing and evolving within specific parts of the globe’s surface. There were a number of racial and ethnic, and even eugenic, related applications of this philosophy that helped to reduce the popularity and academic respect the field of geography had in general by many American educational systems. Whereas geography was traditionally a study of space and time when it came to people’s behaviors, by the 1960s it had evolved into a study primarily of place and place-related nomenclature over time. The focus on culture was reallocated to such fields as history, anthropology and ethnography.
In modern medicine, ET tends to follow the objectives of the central example of approaches defined above.
Sequent Occupance theory and Epidemiological Transition can be integrated into a single set of paradigms used to better interpret population health history. The ICD9 categories provide opportunity for specific cultural assessment to be made about disease, along with specific income- and quality-of-care (QOC) related population health outcomes. Individual strongly influenced by the writings about poverty and health for example tend to focus on population disease states as they relate to socioeconomic inequality. In theory this means that if we study diseases areally with regions defined based on median income for an area in combination with types of work engaged in by region, that somehow we can also define certain anthropological features for a given setting, such as the presence of a low-income hispanic population, an urban-suburban exceptionally low income African American population, or a mixed high-low income predominantly Native American or Southeast Asian setting. These sociocultural, economic definitions for a region can in turn be used to determine certain disease types or ICDs to be evaluated and compared. [Examples of these sociocultural syndromes nad medical histories are reviewed on the prior page in this series.]
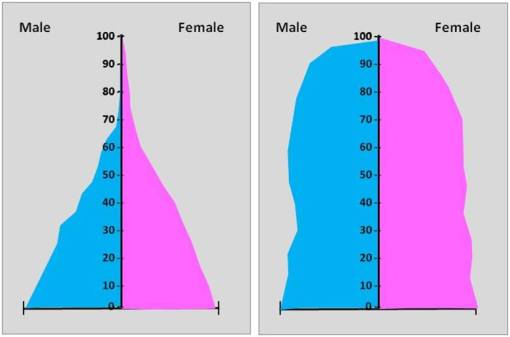
Two theoretical pyramids: Developing Country and Developed Country
Results of Epidemiological Transition
One of the results of epidemiological transition is the production of exceptionally different population pyramids for base populations and in turn impacting the typical disease age-gender prevalence distributions common to that population. Earlier stage populations tend to show a much larger percentage and number of children than population pyramids for developed countries. Later populations tend to show much more costs incurred due to the need for elders’ care. In developing countries the elders are much fewer in numbers and at times even rare. In developed countries the elders are all too common in terms of numbers, needs and ultimately financial stresses placed upon the health care system.
Interpreting the same features in just one kind of country setting–the developed country such as the United States–we find that certain features of the developing population still exist in low income community settings. Even though lifespans are much longer, and the elder to newborn child ratio more like that of the many other developed countries, our poor community settings still demonstrate some of the population health features expected of developing countries surviving in some sort of financially emerging status.
The types of ICDs that involve the poorer populations and communities differ from those of middle to upper class settings. Natural history and environmentally-linked disease patterns play a more important role on the medical conditions or diseases states of people surviving in low income settings. For this reason, another method of viewing and interpreting disease patterns as a temporal feature, we can make use of the Sequent Occupancy model defined by geographers, a method of defining stages of popul;ation health and disease patterns based on styles of living, occupational patterns, and ultimately financial background.
The fishing industry for example is vastly diferent in lower income developing countries than highly developed technologically sufficient countries like Japan or Finland. The related changes in workplace activities, settings and equipment manufacture result in new sets of diseases.
We also see some of these effects with certain Natural Products industries such as oil and textiles. Technology changes add to the disease profile of such work settings, and at times do little to remove the much older health-related threats that still exist. In the coal mining industry for example, a pneumoconiosis state is more likely to be identified and classified as such in the developed country medical setting, with secondary and tertiary care facilities more likely to recognize and quantify such states than lower income, rural health care settings. This is not because lower income settings cannot diagnose these problems, but rather because they are more likely to refer such a possible case for verification of diagnosis to a secondary or tertiary care facility where adequate testing apparati and technologies exist.
The population pyramid above for a theoretical developing country (left) suggests a population that will have increased numbers of child-care related events, and very little old-age events. That of a developed country demonstrates the possibility that fewer of those diseases common to very old age population will present. Just how an ICD prevalence pyramid compares with the overall population pyramid shape or form is what defines this relationship.
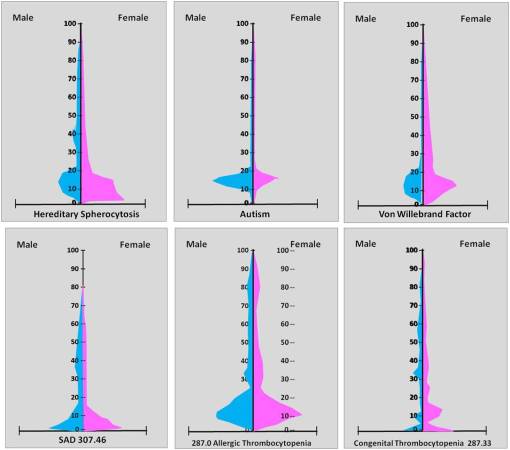
Autism, SAD, and Allergy-induced blood dyscrasia, and 3 Genetically-linked Childhood Disorders
Childhood Diseases.
Note: Childhood diseases are reviewed as well on another page.
.
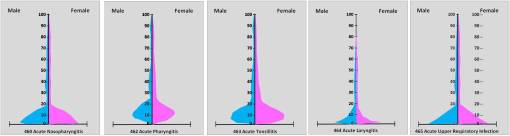
Five very common ailments in children: acute post-nasal drip, sore throat, tonsillitis, laryngitis, and acute upper respiratory infection
Midlife-Adult Diseases
Two categories of disease must be considered to understand the differences between intrasocial or intranational disease comparisons and intersocial or international disease comparisons. The first are comparisons of diseases experienced by the rich versus the poor, the urban versus the rural community. The second is a comparison made between two different sociocultural systems, with rich versus poor, and lifestyle type 1 versus lifestyle type 2 as the major comparitive features.
With developing countries and social systems, it is the childhood population that undergoes significant change over time in terms of percentage and needs for health care services. Developing countries like underpriviledged social settings tend to have larger numbers of children, and when these underpriviledged communities are non-traditional in terms of national expectations, they are even more underpriviledged than others that have a certain amount of widespread social acceptance. With regard to old-age adults, underpriviledged communities tend to demonstrate more respect for the elderly community and engage in making the best use of this small part of the population. In other community settings, old age adults are more commonplace and popular, and tend to lose some of the respect from those of younger years, and at times event those involved with community leadership positions. This means the mid-life adult population can have some very important differences in terms of value and meaning, and consequently physical and social health status and overall community meaning or purpose.
Epidemiological transition events as they pertain to the mid-life adult years are those changes we most often learn about with international comparisons. In a developing country setting, mid-life medical crises center around some of the more basic survival-related medical problems and needs; things like receiving a complete immunization, obtaining adequate care for injuries, working in a safe environment without concerns for environmental exposure, engaging in safer dietary habits accompanied by a fully nutritious diet, living in a household where exposure to the elements and vermin will not be so conducive to infectious disease propagation, are all features that typify the underpriviledged life in a theoretical non-developed sociocultural setting or a low income developed country sociocultural setting. Opposing this is the status of a developed country, moderate to high income sociocultural setting, where physical diseases are allowed to develop due to life’s experiences, and where mental disease changes and develops due to soci0culturally induced psychological and emotional change. Whereas childhood diseases represent one set of unique physical environment and cognitive/psychological environment series of conditions and their potential treatments, and old-age adults diseases yet another such socioculturally-defined series of life experiences with or without respect, mid-life medical events are very much a consequence of one’s personal response to the current lifestyle and socioeconomic conditions.
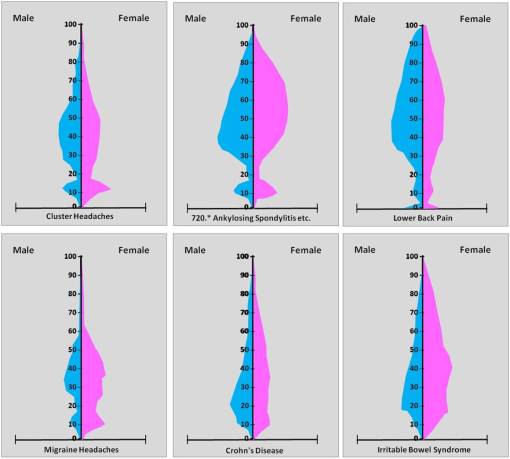
The epidemiological transition diseases associated with mid-age groups are of numerous types. Due to highly varying social and environmental factors playing their role in how these diseases develop, are treated, and undergo change over time (usually worsening as chronic conditions), we can find sets of diseases possessing apparently identical age-gender distributions, with age-gender inequality introduced due primarily to regionally, nationally and/or culturally defined differences, or we can find what we expect to be similar diseases with similar distributions bearing completely different age-gender distributions due primarily to age-gender generated differences in social response and in turn personal responses to these social behaviors.
Mid-age Disease Patterns with sociocultural and biological similarities
.
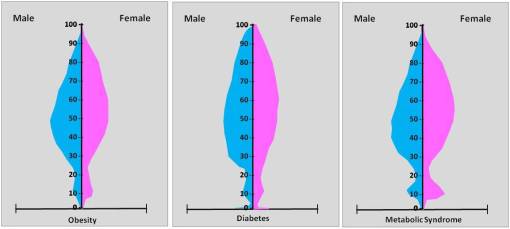
Diabetes and Metabolic Syndrome
Metabolic Syndrome – Diabetes Disease Complex
From “Survival Gene” to “New World Syndrome” to “Metabolic Syndrome”
The term “Metabolic Syndrome” for use as a diagnosis for diabetes related ailments and its comorbidities became very popular around 2000. The Metabolic Syndrome ICD is coded as a subset of endocrine disorders and is in close association with such diseases or conditions as . . .
The predecessor to applying the term metabolic syndrome to this particular physiological condition was “New World Syndrome”, a term developed by anthropologists studying the highly pronounced morbid obesity common to Pima Indians. This morbid obesity was theorized to be the result of a genetic selection process of the human genome induced by the migration, weathering and dietary history of the Native American cultures and their migration history as isolated maritime or oceanside communities, followed by ocean-land communities residing more inland from these island communities, followed by the in-migration of numerous later American Indian cultural groups who chose to reside still further inland, ultimately becoming the predecessors to the Great Plains Indians.
These Native American groups were observed to show significant changes in appearance following the stabilization of the trapper-furrier-fort dominated fur trade industry that developed in Canada and parts othe United States between 1850 and 1890. This stabiliztion in part required the cohabitation of Native American groups previously residing distant from each otehr and from the Euro-American and European communities dominating the economic activities that followed and defining any resulting land ownership claims. These land ownership claims in turns changed the lifestyle of the Native American considerably, and as demonstrated by studies of the Hudson’s Bay Trading Post Native American interactions (esp. Inuit or Eskimo), the proximity to adequate food stores of particular processed European form enabled many of these communities to begin to demonstrate an onset of obesity followed by diabetes for the first time. This particular epidemiological transition process clearly demonstrate the impacts of assimilation and lifestyle changes due to changes in lifestyle (in accordance somewhat with sequent occupance teachings) on the form and healthiness of those undergoing such assimilation, acculturation processes.
By the 1920s, it was not unusual for articles about the endurance of Native American or American Indian individuals to demonstrate unique survival traits, such as the development of the athlete’s heart and a fairly healthy, simple lifestyle including diet and heavy exercise like activities. These methods of living were in part due to the limited lifestyle indigenous peoples had. By residing on reservations, their activities and potential for experiencing the western disease, European disease process was extremely limited. Due to lifestyle environment and conditions, these communities dsuffered more from the types of problems and conditions noted for 19th century European and Euro-American settlement practices. Infectious diseases and maladies related to very filthy lifestyles were typical for such reservation settings. This turned the Native American communities into the triangular like population pyramid setting noted above, with significantly high mid-age mortality rates,, high fertilization rates and child care related public health needs, and very low old-age related public health needs or developed country-like diseases.
As a result of this paradigm in healthiness versus non-healthiness when it came to reservation lifestyles, the notion of a “survival gene” was invented and fopr the next decade or two was a highly popular medical anthropological take on the Native American age-gender relationships and resulting culturally defined behaviors involving the elders and their important roles in most indigenous societies. By 1988, the understanding of disease etiology and physiological mechanisms was better understood, enabling the “New World Syndrome” theory to be proposed. This theory stated that these particular genetic traits and resulting health related problems, or benefits, were survival-based neodarwinian or social darwinian aspects of the indigenous belief system. Accompanied by cultural beliefs and infleucens, the tendency for individuals to rapidly gain weight ensured survival during long periods of starvation and lack of fodd, but also made it possible for porolonged food consumption over longer periods ot time to ultimately cause a variety of natural consequences of this weight gain process–conditions or diseases like diabetes, gall bladder disease, liver problems, pancreatitis, hypertension, and various forms of cardiac disease. Throughout the 1990s, the “New World Syndrome” concept dominated mostly the anthropological and anthropology medical journals.
Numerous studies of genetically carried diseases in other cultures however enabled a broader more multicultural interpretation of this biological process to be developed. Northern Japanese, Russian, and Scandanavian communities alo demonstrate similar genetic traits facilitating the onset of certain disease patterns, which in turn could be paralleled with many of the teachings of the New World Syndrome. Ultimately, this enabled physiologists and medical researchers to apply the New World Syndrome science and etiology to other times and places in global medical history. Ultimately, this enabled three versions of the study of epidemiological transition to merge into the single theory related to an already well-defined ICD for “metabolic syndrome.” Although not a perfect match with the New World Syndrome cocnept, metabolic syndrome sufficed as an official parallel with metabolic syndrome, and has since become the standard for how we review this kind of medical or epidemiological history.
.
Relying totally upon metabolic syndrome to define what was the New World Syndrome suffices, but is not a perfect match. Metabolic Syndrome implies primarily physiological causes and mechanisms for these medical conditions, and writer who focus on the Metabolic Syndrome way of evaluating these medical states, place less emphasis on such non-endocrine diseases as gall bladder disease and even cardiac disease (although they tend to retain hypertension as part of their philosophical argument). The historical (“survival gene”), anthropological (“new world syndrome”) and ceontemporary public health/epidemiological (“metabolic syndrome”) approaches to defining this set of conditions related to sociocultural change and develop exemplify the reason why epidemiological transition merges well with the sequent occupance view of disease changes over space and time, which in turn can then be related to the mechanisms by which changes in society in general, physically and behaviorally, are in large part responsible for the epidemiological transition process currently promoted.
Midlife disease history and ecology are the primary determinants of later disease development and onset experienced by elders. Epidemiological transition there requires and understanding of disease patterns in these three groups, separately as well as together. Some diseases realted only to one of the three levels defined for disease beahviors. Others demonstrate the transitions that occur as a disease develops and impacts populations first in the childhood popualtion, and again later in the elders’ population, whereas others often show tendencies to change their behaviors over time as people get older and change from one age group realted set of risks to another age-group related set of risks.
Older-aged Adult Diseases.
My review of adult-onset and old-age onset diseases/ICDs reveal maladies that increase in prevalence due to increased longevity. When reviewing this information it is important to note the biological causes and contributors to these patients and the systems-defined sociocultural initiators and confounders that possible exist. In general, symmetric prevalences are natural and ecological in origin. Asymmetric disease is often human ecological in origins.
The following types of adult-onset diseases with minimal mid-age influence are known to exist.
.
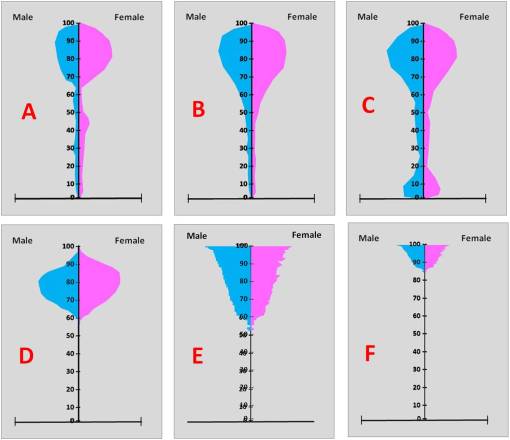
The above 6 pyramid forms depict specific age-gender disease pattern seen to recur in the US population.
Example A represents a disease which has some early cases of onset but which demonstrate little significance in prevalence until the patient is much older. The types of diseases that exhibit this behavior are as follows:
- Conduction Disorders (426.*)
- Cardiac Tamponade (423.3)
- Ventricular Fibrillation (427.41)
- Ventricular Flutter (427.42)
- Atheroembolism (445.*)
- Aplastic Anemia (284.*)
- Septic Arterial Embolism (449.*)
Example B represents a disease which increases fairly regularly with aging, is equally dispersed between genders, and which culminates and perhaps results in mortalities once the patient reaches 85 years of age. The types of diseases that exhibit this behavior are as follows:
- Gout
- Emphysema (492.*)
- Bronchiectasis (494.*)
- Pleurisy (511.*)
- Athersclerosis (440)
- Pneumoconiosis and related conditions (500-508.*)
- Severe Chronic Liver Disease
- Severe Hypertension with cardiac and renal complications (404.*)
- Ischemic Heart Disease (410.*)
- Atrial Flutter (427.32)
- Hereditary Neuropathy (356.*)
- Myasthenia Gravis (358.0)
- Dupuytren’s Contraction (728.6)
- Corns and Calluses (700.*)
- Acute Respiratory Failure
- Osteoporosis (733.*)
- Factitious Disorder (300.16)
Example C represents a disease which has childhood onset, reductions in prevalence for most of the remaining life, followed by a resurgence in prevalence initiated either by the aging process and/or by a reduction in population size due to other old-age onset diseases resulting in mortality. The types of diseases that exhibit this behavior are as follows:
- Other degenerative nervous disorders (333.*)
- Chronic Bronchitis (491.*)
- Functional Responses following Cardiac Surgery (429.4)
- Cardiac Pulmonary Valve Disorder (424.3)
- Degenerative Vascular Disorders (388.0)
- Hip Dislocation (835.*)
- Other Non-organic Psychoses (298.*)
- Acute Psychogenic Paranoia, unspecified (298.4-298.9)
- Other Psychotic Disorders due to Head Trauma (310.8-310.9)
Example D represents a disease which primarily originates in the 60+ year old community, which due to its fatality also results in deaths over the next few decades. Peak ages for this condition are 80 for men, and several years older for women. By 100, nearly everyone who has this condition is deceased, but possibly due to comorbidities as well. The types of diseases that exhibit this behavior are as follows:
- Parkinsonism and allies (332.*)
- Chronic Pulmonary Heart Disease
- Chronic Liver Disease
- Cardiac Aortic Valve Disorder (424.1)
- Aortic Aneurysm with Dissection (441.*)
- Arterial Embolism due to thrombosis (444.*)
- Chronic Pulmonary Heart Disease (416.*)
- Celiac Artery Compression Syndrome (447.4)
- Giant Cell Arthritis (446.5)
- Pelvic or Femur Neck Fracture
- Septicemia
- Disseminated Intravascular Coagulation
- Prostate Hyperplasia
- Benign Prostatic Hyeprtrophy
Example E represents a progressive disease that has an onset between 50 to 60, but by itself is usually non-fatal, thereby increasing in prevalence as the population reduced in size and its presence continues to persist in the surviving population. The types of diseases that exhibit this behavior are as follows:
- Atrial Fibrillation
- Acute Myocardial Infarction
- COPD
- Acute Myocardial Infarction
- Heart Failure (428.*)
- Stroke
- Osteoarthritis
- Chronic Renal Failure
- Hip-Knee Replacement
- Chronic Ulcers (707.*)
- Amyotrophic Lateral Sclerosis (335.20)
- Cardiomegaly (429.3)
- Glaucoma
Example F represents a progressive disease that is generally non-fatal, of late onset in life, with its greatest prevalence found in the oldest age groups. The types of diseases that exhibit this behavior are as follows:
- Dementia (290.*)
- End-stage Renal Disease
- Diabetic Retinopathy
- Glaucoma
- Reactive Confusion (298.2)
.
Social Inequalities
The relationship between epidemiological transition and childhood disease has a significant impact on communities with a shared sociocultural upbringing. In recent decades, the return of infectious diseases common to society a century earlier has reduced some of these differences between developing and developed countries, low income and high income communities. Diseases like measles, mumps, scarlet fever and tuberculosis have resurfaced in new strains for which immunity was once very close to 100%. These immunization rates have since reduced due to parental choices made and popular claims regarding the relationship between immunization, post-immunization complications and other medical concerns like ADHD and autism. The “science” behind many of these concerns is lacking and demonstrates how little the general public really knows.
One of the most common diseases linked to immunization behavior and childhood illness is autism, increases in which have been blamed on the use of mercury in certain vaccination products. This public disconcern may be a result of several reasons linked to loss of trust in the health care system in general, combined with any of several unmonitored belief systems that have developed over the years due to lack of adequate public health education programs and the reduction in consumer experience and know-how. Old belief systems are often some of the worst belief systems to change. They can outright conflict with each other and yet the followers of such claims lack the sensibility needed to come up with a reasonable conclusion. Take the belief in homeopathy as an example, and how it parallels in philosophy the immunization theory. It is easier to convince someone that homeopathic remedies might work due to a greatly diluted formula, with soft science theory attached to this ideology, than it is to attempt to prove another soft theory wrong, relying upon experimental results more than equal in caliber to the studies by which homeopathy was developed. For homeopathy, theory is just theory. For immunization, physical science prevails but is a victim of social philosophy and social pyschology. Both philosophies are generated using the same philosophy–one soft science and theory based, the other hard-science and very much results based.
The ways in when we manage disease as professionals and as the everyday domestic citizen are two quite different routes to take with personal health care and prevention. Health in the United States is an aggregate of numerous traditions, philosophies, and belief systems. For many, their victimization is due in part to their own intellectual states and pursuits, but as an entire country operating under one major health care system, they are also victims due to the continued operation of these much smaller belief systems as part of this major health care system. We see evidence for this inequality existing due to the poverty and poor health often attached to this kind of social setting. The United States as a whole is interpreted as adeveloping country whose residents live a longer life than people residing in non-developed countries. But within the United Systems there are also these lower income underdeveloped communities with public health issues that need to be dealt with.
Epidemiological transition is a term applied to the migration of people and cultures from one state to another. Usually this migration happens in the direction of worst to better, like the development of the non-developed country or exceptionally low income culture into a developed country with moderate to high income possibilities. Attached to this economic change are the diseases and lifestyles that people live in these different settings. United States health care systems typically have numerous types of low income versus moderate to high income living settings, with each of these in turn demonstrating disease pattern changes. Accompanying these changes in disease patterns are the related changes in health care options provided to low income versus moderate to high income community settings. In turn, we have the differences in medical opinions that must be dealt with whenever such dichotomies exist in a given setting.
Several levels of change are noted in the epidemiological transition theory that can be related to disease type and sociocultural causes for the diseases that prevail most. The population pyramid provides some important insight into this query into health in that we realize some diseases are simply close to impossible when it comes to trying to manage current disease issues and prepare for future disease change. The shape of the population pyramid alone tells us much about how a developing country with its triangular pyramid and high childhood population can differ from a fairly equally dispersed age-gender relationship noted for the developed country pyramid. Each social setting in the United States has similar issues to deal with regarding epidemiological transition and health. Less developed areas or poorer communities tend to have different behaviors and different lifestyles that in turn define their different epidemiological histories. Childhood diseases and old-age adult diseases are two groups that demonstrate the greatest changes in disease patterns over time, be this change a result of change of a country, or result of change of what sociocultural setting you choose or are economically forced to reside in within the United States.