…
Basic Patient Evaluation Process
—
—

—

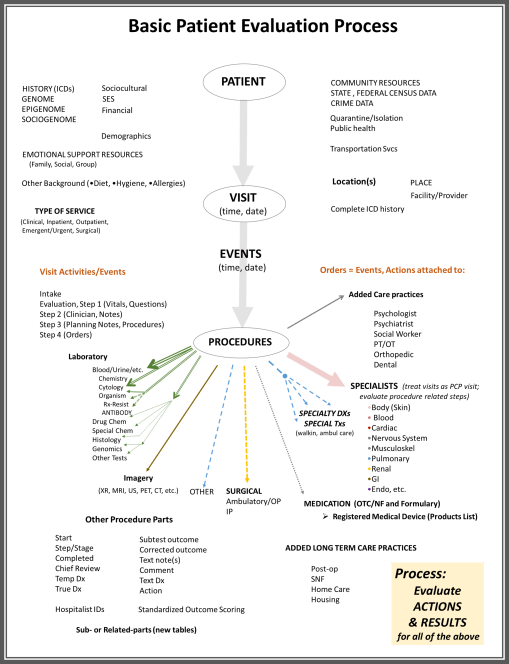
Specialty care undergoes many of the same procedures and PCP care. Many of the same major procedure classes are used, but the details of the test may differ. Additional tests may be included as well. The bulk of specialists’ activities are in the Specialists portion of this table–they are divided by organ system, For each organ system, defined the ICDs and then use this same overall approach from the top down.
—

—

The codes used to differentiate the different procedures include CPT4 codes, ICD 9 and 10, etc. Not all companies may use the HCPC and LOINC codes. Institutional coding needs to be analyzed for every system assessed. ICD Proc codes at the #.## codes used to define surgical procedures.
—

Dollar signs depict $10 units, minus 1. So, $$ – $$,$$$ is interpreted as $10 to $100 (starting range), to $100,000. This is used to relate cost for type of procedure and exact procedure ID to the cost for this Event or Procedure. These show degree that cost is impacted when an event to change cost takes place for certain procedure levels or groups. A review of Procedures by major groups, in detail, is needed to make the best use of these data. For example, whereas typical lab data are $ to $$$ in cost, lab assessment for genomic data are more likely to range from $$ to $$$$ in cost.
—

This is a basic patient, midlife, with a family history of diabetes and obesity, and a genomics pattern suggesting the likelihood for later onset of cardiac disease. This is an evaluation of this patient at a young age when he/she is inactive in seeing a doctor, but also irregularly employed and rarely fully covered. Genomics have not been fully performed, nor are they requested here. This was used to model costs and treatment for younger patients with DM-Ht Disx-HTN-Metabolic Syndrome. Costs were evaluated for this patient, for best care practice, versus patient-defined care practice (to be presented later on the blog for this site).
—
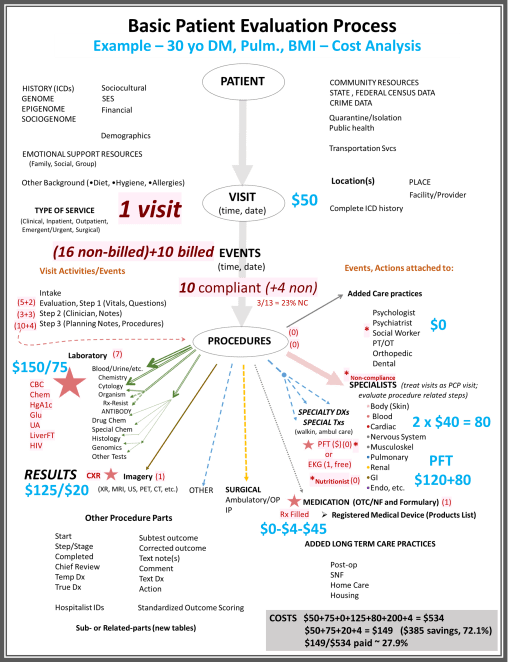
An example of how costs are distributed, and the different types of costs, or ranges of costs, for the same event.
—

HR time is assessed as briefly as possible. Complex care requires more clinicians and visits, so of course the cost accrued by the patient is higher.
—

—

—

—

—
The following numbers were used to generate the graphs above (except for the “Total, ED and Study Populations” work) This is for a theoretical “perfect” one hour annual visit.

—
Recommended therapies are rarely followed, with some steps put off for later days. The above case has a younger patient resistant to spending too much money on his or her “best care practice.” Both the patient and caregiver decide what to do.
The caregiver decides to not continue genomic testing for the time being due to its high expense and lack of complete coverage. The patient then decides what recommended calls and visits to other specialists he or she will be engaged in. A cost estimate for these visits is provided. The patient uses the following logic to make the decision. Cost reductions for being unemployed are then taken into account, to define the “cheapest route”, although not most healthy route for care.
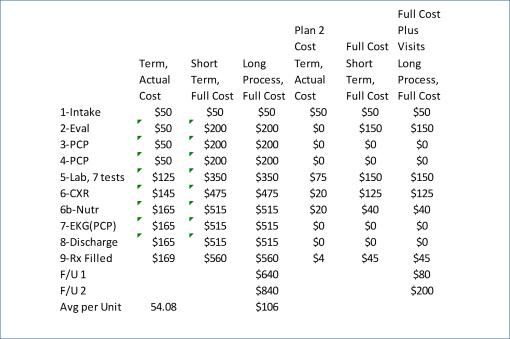
The end row on this table is data for cost units. This is determined by evaluating the time the patient spent to receive all of these services. That time is related to its cost to the payer. The patient spent one hour receiving the care that cost $169. The full cost, full participation would have required 3 hrs 10 mins of the patients time, costing $840. Average per Unit is the average of the care, or total cost divided by per unit of care given, a theoretical cost index.
This is evaluated per procedure part that is actually billed, not all procedure parts. i.e. Visit, lab, xray vs. the same with two additional visits added, and three to four addition costs.
—
Same as above, Version 2
Same as above, version 2
—
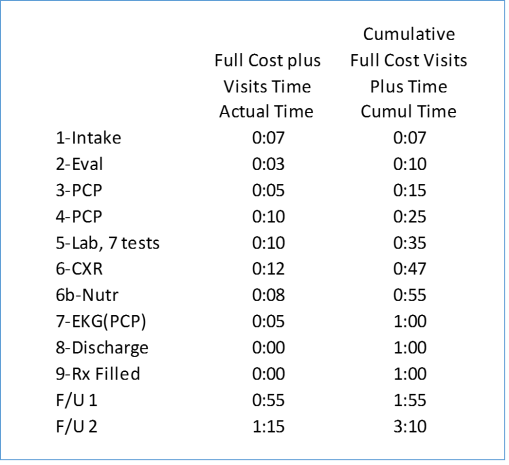
The following are the time allocations required to carry out the original visit, agree to see a nutritionist briefly, and then follow up at some later time or data with two visits of specialists.
For Follow-ups 1 and 2 (F/U1, F/U2): The first specialist concerns the patient’s behavioral health state. A counselor or psychologist has been recommended. The second specialist is devoted to lung health, and was recommended due to the patients asthma or allergy history. That provider would probably want to perform a pulmonary function test.
—