The Medicine Chests
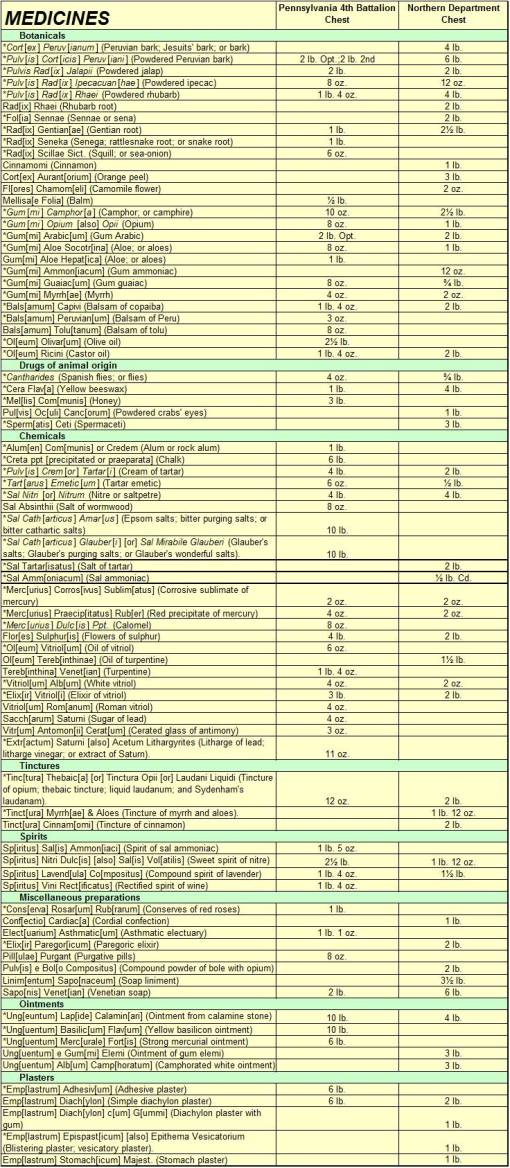
The following list depicts the contents of the two medicine chests reviewed by Griffenhagen.
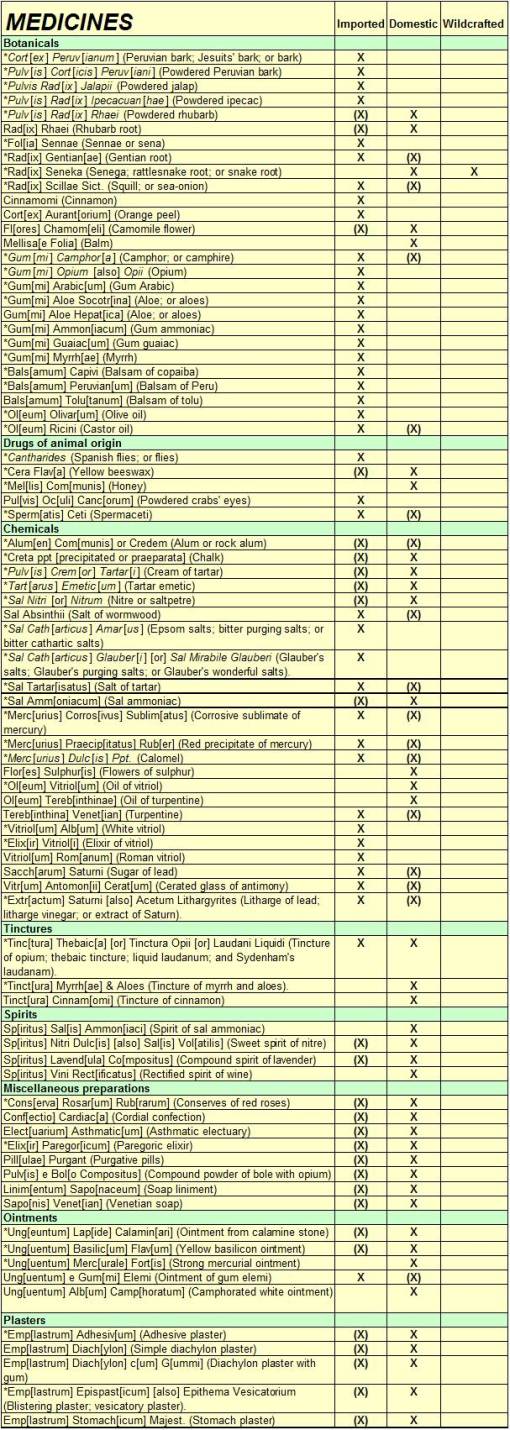
The sources for these medicines are noted in the next table in the last 3 columns. Important to note is the prevalence of imported medicines on this supply list, and the near absence of locally wildcrafted medicines. Since these ingredients were decided upon based on early reviews of the storage, shipping and manufacturing industries related to the import of these valuable remedies, there was limited concern for future supplies and no experience to base any final decisions upon. In the months and years ahead, it would become clear that many of the original actions taken in preparation for the War would have to change. The impact of the war in terms of battle-related injuries were far surpassed by the problems soldiers faced due to bad weather and poor food, clothing and ultimately medical supplies designed to treat non-war related problems. The crowded conditions that were endured at times made highly contagious infectious disease spread quite rapidly through nearly all of the ranks. The unsanitary living habits made diarrhea and dysentery a constant concer for those trying to prevent the onslaught of a new disease within the local camp settings. The heavy dependence upon imported, foreign-produced medicines at times made dealing with local fever epidemics an almost impossible task.
The following is a review of the above medicines in terms of their origins and sources. Note the implied dependency on many of these as import products, and those for which some accomodations could perhaps be made. Very few of the medicines on this list are completely local in origin.
The first thing to note from the above list is that nearly all medicines were probably received as imports before the war, and that as the war progressed, they either had to be substituted for, or produced locally whenever possible. According to MacQuer’s Elements of the Theory of Chemistry (English translation, 1758), some of these products could be manufactured at home or in a special lab-like setting, assuming the equipment needed to engage in such a task could be afforded and were allowed to be imported. According to historical documents on some of the chemical manufacturing procedures engaged in during the war, in particular for the production of gunpowder ingredients like saltpeter, large scale manufacturing was possible within the colonial setting. Likewise it seems reasonable to assume that some remedies or medical ingredients, requiring simple extraction and separation techniques for their production, could be produced within the local colonial settings, even in rural factory-grade facilities. For this reason, the above table notes with either an ‘(X)’ or ‘X’ in the Domestic column suggests that such a process was either perhaps possible = (X), or most likely engaged in = ‘X’, respectively. Many of the ingredients in the Chemicals section of the table may have been produced in this fashion. Items like alum, chalk, cream of tartar, flower of sulphur, oil of vitriol, oil of terebinth, sal tartar, sal ammoniac, sal nitrum, saccharum saturni, vitriol albus, and the assorted mercury compounds, could have been produced from start to finish using just the local materials. The same was true for many of the “spirits”, ointments, and plasters. Certain medicines, such as “crab’s eye” and cantharides had to be imported. For most of the complex recipes like Conserve of Red Rose and Compound Spirit of Lavender, the entire pre-manufactured proprietary product had to be imported. Even many of the plant sources such as ipecac, opium, gum ammoniac (Dorema ammoniacum) and orange were not native to North America and could be harvested only in certain climatic or environmental settings. The same was true for a number of tinctures and plasters made using the foreign-derived gum elemi, cinnamon, myrrh and aloe.
In terms of availability, many of these medicines had limits to their renewability due to their reliance on exported products. These can therefore be considered non-renewable medical resources, which due to their large numbers had the potential of significantly limiting the forms and amounts of services that could be provided within the local field and hospital settings. Large stores of these supplies would have been an essential step taken in preparation for the War. Some attempts were made to produce some of these products locally, but for the most part, only a select few botanical medicines could be produced in fairly substantial amounts within local garden settings, and a number of the mineral remedies produced through some sort of small scale, semi-industrial means.
Making sense of the above remedies
It helps to review the above list of medicines in terms of how diseases were defined at the time, and how they were felt to be correlated with each other. The definition of a disease depended heavily upon its presentation, and less so upon its internal physiological or anatomically (organ) related appearances. Many medicines treated primarily the symptoms an individual was experiencing, and at times were effecting if treating the disease should its primary problems be directly related to these symptoms being abated. For the fever for example, the goal of a treatment was to tame heat impacting the body’s temperature. Depending upon how this heat was able to increase and result in a fever, according to contemporary theories on this matter, determined how one was going to treat the condition. In cases of exceptionally high temperatures, cooling was usually recommended of course, whereas intermittant or cycling fever-non-fever states required some form of treatment designed to eliminate the chills experienced whenever the fever subsides. In the case of chest pains and tightness (heart attack of severe asthmatic osnet), the goal was to enable the excess energy contained therein (i.e. the passion related tight feeling) to be expelled, to allow the blood to flow better, and to open up the air passages enabling air to come in and excess ‘humours’ to pass out. The same philosophy would be the case for treating someone with severe edema, such as ascites in which fluids build up in the abdomen between the various organs causing the stomach to expand and appear bloated, or in the case of what is today known as congestive heart failure, in which the feet and legs swell considerable to to a build up of fluids in these lower structures. In either case, the goal of treatment would be to stimulate the body’s normal activities designed to bring these fluids along in the blood stream and out of the body in a much more effective manner. For the ascites, this was done with diuretics and even strong purgatives and laxatives, with hopes that reducing the water in the body would again result in a balancing out of excess abdominal fluids. For the case of peripheral (leg-foot) edema, practices designed to reduce the water and blood volume were employed, primarily diuretics. When water couldn’t pass out of the body, the abdomen was drained through surgery–a small incision enabled some of the fluids to be discharged. In the case of peripheral edema, a weak heart and body energy is the concern, so blood-letting (usually by the feet) is performed to reduce the volume, but not in excessive amounts for fear of resulting in a loss of “animal spirit”.
For both ascites and edema, the more effectively treated problems will be related to some sort of mechanical or chemical, non-infectious disease problem in the body. But these cases can also happen in cases of severe infection. Without knowledge of the “germ” in such a way that these forms of ascites and edema could be differentiated from the rest, it was up to the physician to be aware of cases in which weak animal spirits were not as much a problem as other potential causes were. Without knowledge of how to treat infection-related cases, these physicians could only rely upon methods already in use, as stated above, with extra attention paid to whether or not such practices could be detrimental to the overall health and animal spirit that makes the body work. A number of times, physicians also related the soul or vital spirit (associated with the brain and psyche) to some diseases. The typical example of this is diseases in which tightness of the chest are not at all related to such things as a true heart attack or a severe pneumonia, bronchitis, or asthmatic attack. In cases like pleurisy (painful breathing due to infection of the cavity between the lung and inner chest wall/ribs), sudden difficulty breathing (of a psychological or “passion” related nature), and ascites brought on by internal infection, the cause was not mechanical but organismal. Being that this feature was not known, the most likely treatable of these three conditions would be that due to the psychological or passion-related cause. Depending upon the course of the infection and whether or not effective surgery was performed which had some remediation effect, the resulting pleurisy, edema or ascites may or may not be cured.
Of course, none of these outcomes really had much to do with medicines applied to each patient. At best these medicines were identified based upon some symptomatology, appearances and past experiences that made the physician use them in whatever way he/she did. In some cases, the medicines did eliminate symptoms, such as the the use of opium to eliminate the continuous passage of liquidy stools, but in many cases they did everything from nothing to being fairly effective at diminishing one or more symptoms. Depending upon how the physician observed the patient and analyzed any treatment related outcomes that were produced, the patient may of may not be diagnosed and treated correctly in the contemporary sense. In some cases, many of which become fatal, a hastened heartbeat (a typical sign of physiological shock, just before fatality) might be interpreted as too much passion, resulting in the administration of a medicine that slows depresses the body and down the heart, thereby allows the patient to fall into a deep state of shock even more quickly that without such a treatment, just before dying.
Fever Medicines
One of the most important “diseases” many of the soldiers regularly and commonly faced in the Fishkill setting were simply referred to as fever cases. The most common causes for fevers in the Fishkill setting were, in seasonal order: influenza and colds, food poisoning, mosquito-borne malaria and yellow fever, and autumnal and winter typhus or typhoid fevers. These fevers were not known by these names at the time, but rather were referred to in terms of their related symptoms and temporal behaviors. Fevers related to influenza, often winter-borne, were simply interpreted as fevers due to their relative lack of cyclicity. In cases of sweating, they may be referred to as fevers with ague. Malarial fevers of mosquito origin (which they did not know) and which tended to occur in damp environments, next to swamps and marshes, a few days or more following a heavy rain, were often referred to simply as some form of miasmatic fever, unless they showed a tendency to have periods of flucatating febrile temperatures, in which case they were referred to as intermittent and remittent fevers. In Dr. Osborn’s manuscript, a reference made to such a fever refers to it as “3-day agues.”
Yellow fever, referred to as bilious fever during the American Revolution, was also mosquito-borne (again unknowingly so in the minds of colonial physicians), and therefore, common again to humid settings and the like when and where ague is born. The primary difference with this fever, versus the malaria, is its tendency to yellow the skin.
Spotted Fever rarely called such during the Revolution) was in actuality typhus, and at times a completely different disease typhoid fever. Whereas typhus is often spread by rodent and lice, typhoid fever is actually brought on by a form of bacteria. Both had similar events preceding them, such as poor sanitation, over crowding and poor health on behalf of the potential victims, and typically were spread msot often during the colder climates when crowding and poor nutrition were at their worst; then, this typhus was primarily of rodent cause and therefore was the true form of typhus. Other names for this winter fever include Ship Fever, Jail Fever and Camp Fever.
The only successful remedy for fevers at this time was Peruvian bark for the treatment of Fever with Agues or Malaria. This is due to the chemical make-up of this plant remedy (contains quinine). However, because physicians were unable to distinguish between thevarious forms of fevers at times, the only guiding post to recognizing a fever treatable with Peruvian bark was its ague-like feature, which many doctors claimed to be related to other diseases as well. As a result, we find Peruvian bark in heavy use for all types of fevers. Its complementary herbal remedies for the time, such as the above Chamomile and Melissa, were included in order to supplement its anti-febrile use. A number of other aromatic plant medicines above may have been emplyed with similar uses in mind. This was also a use closely linked to the Seneca Snakeroot (‘Radix Seneka’ above). Fortunately for the staff and patients, adequate sources of fever agents could be found in the imported, domestic and wildcrafted plant medicine lists, with Peruvian bark remaining the necessary plant to work more aggressively about in order to maintain an adequate supply.
Diarrhea, Dysentery and Cholera Morbus
The single most common public health epidemic to strike the soldiers in their camp was dysentery. This is a severe diarrhea in which cases which last more than just a few days tend to begin producing bloody stools and significant amounts of stomach pain and cramping. Unlike diarrhea, a ‘flux” that usually lasted just a short while (<1 day to a couple of days), dysentery can last for weeks and take their toll due more to fluids loss in association with poor nutrition uptake. One of the most popular uses of opium during the colonial period was as an effective agent for stopping the flux. A natural consequence of taking opium is the reduction in intestinal tract activity and a slowing of the passage of solids and fluids through the intestines, thereby providing more time for the body to reabsorb some of its fluids.
Whereas diarrhea could often be the consequence of contaminated or spoiled food, dysentery was due to a bacterial organism, which again was a fact that local physicians and surgeons had no knowledge about. Physicians and surgeons tended to interpret dysentery as either a new disease erupting in the body or the consequence of some other illness already being experienced elsewhere in the body, such as a case of pleurisy or hepatitis. Their treatment modalities therefore tended to focus on a combination of activities meant to balance out the body’s state, thereby eliminating the imbalance that other illnesses may be caused by impacting other parts of the body. Relying upon the above listing of medicines, this means that aside from opium, they would probably try to administer certain mineral remedies that do the opposite of being a laxative (i.e. chalk and rock alum), administer something to either completely purge the body of its problems such as an epsom or glauber’s salt, and provide some sort of tonifying or strengthening agent (i.e. a very bitter gentian-based tonic). Accompanying this regimen would be whatever medicines the person was already taking, for whatever else was ailing him at the time. This usually meant the continuation of such remedies as a cardiac tonic being taken for an ailing heart (Cordial or Cardiac Confection), compound spirit of Lavendar (to strengthen a weak state of mind and/or emotions, the opposite of passions), asthmatic electuary (to strengthen breathing and more effectively improve the blood and balance out the excess alkali), or pulvis e bolo compositus (for very sick bodies in general).
The severest forms of diarrhea-related conditions result in so much fluid loss that the body is becoming weak and closer to death. This choelra morbus state is typically diagnosed by prolonged diarrhea or dysentery, or the expulsion of very dark (almost lack) material. Whereas the passage of blood from the stomach down to the colon usually results in black, grainy stools, the development of severe decay in the colon or intestines may result in a stool that is rather pasty in nature; where both of these may be considered cholera morbus, the latter is often more prolonged and fatal, and the former fairly short-acting or fatal in much shorter time (such as due to a cancer-induced bleed of the stomach, or a degrading peptic ulcer, both of which were often referred to as dyspepsia during the colonial years).
Rheumatism
We think of rheumatism as a joint disease, charcterized by the long term consequences of arthritis. Historically, rheumatism in its purest sense was initiated due to the onset of a fever condition during childhood–rheumatic fever–which over the years had long term consequences on the body due to a prolonged autoimmune syndrome that developed due to this infectious disease history. The most common consequences of of rheumatic fever were joint pain and malformation due to inflammation of the joint space and surrounding tissues through the implantation of the disease causing organism into these tissues. A characteristic arthritis of the knee (genu-arthralgia) often developed in these people during their mid-age years, often during the peak of their professional practice. Years later, this organism had the tendency to cause valve-problems in the heart, leading to weakness followed by heart failure and congestion of the limbs or lungs due to poor cardiac function.
It is possible that physicians noted some correlation between the childhood fevre and the effects it had on the overall body in later years, but during the colonial period such observations seem few, if any actually existed. For this reason, the Rheumatoid Arthritis of the colonial years was perhaps more a symptom of arthritis or rheumatoid in general. Since rheuma tends to refer to inflammation in general, it was the inflammation associated with this arthritis that took center stage, not the reason a particular part of the body had become inflamed. As was typical of colonial period medical philosophy, this meant that a physician could take any of several routes in his philosophical reasoning for this type of arthritis, in order to describe its “true cause” in the most modern sense. Aside from humours-based thinking, which constituted a fairly small part of the reasoning for this time, there was the theory of alkalinity and theory of heat (fire) that could be related to rheumatoid onset. Due to Boerhaave’s teachings, alkalinity prevailed as a theory for Rheumatoid of the joints, and were a physician to link the joint inflammation to a subsequent heart condition, it is even possible that the flow of this alkalinity from one organ system to another could be used to define how later consequences of this disease arose. This philosophy of disease change, transgression or transmutation is very much supported by the essays on disease penned by Dr. Osborn. Osborn uses this reasoning to explain why one condition can lead to the next, such as gout, to pleurisy, to ascites, and finally to consumption.
In some of the above formulas for treating Rheumatism, we find the use of plasters and oils to be recommended due to their theoretical ability to draw out the alkalinity from the joints, balance the heat, and reduce or rebalance the erratic humours infecting the overall joint and joint space.
The Entia or Vital Spirit and Sal Ammoniac
The use of Sal ammoniac (ammonia) has a particularly interesting history related to the philosophy and psychology of disease. Today we think of this as nothing more than smelling salts, which is pretty much what it became by the time to Revolutionary War began. However, the origination of the use of sal ammoniac has a history very much alchemical in nature and philosophy, which deserves a brief review. The evolution of this philosophy begins with Paracelsus and his identification of the fifth element or essence. In subsequent writings, other scientists like Johannes Van Helmont and Hermann Boerhaave came to view these essences or entia (ens) as important metaphysical agents capable of modifying and controlling the animal spirit and health of the body. One goal of alchemy during this time was to figure out a way to produce this essence of life or “philosopher’s stone” capable of controlling one’s health and longevity. The sal ammoniac or salt of ammonia played an important role in this piece of history for the field of chemistry. As this practice of chemistry became an important part of medicine, much of which was due to the influences of Dutch chemist and physician Boerhaave, the field of iatrochemistry was born–a more “modern” way of interpreting alchemy or early chemistry as important to a complete medical training.
The source for Sal Ammoniac traditionally was the horn or antler of an animal, in particular the Cornus Cervi (antler of a deer) and at times any materials considered to be a “Unicorn horn.” By treating these a particular way, this substance was made to emit noxious vapors, producing a powdery substance that would do the same when water or the proper fluids (acids and the like) were added. A traditional use for the sal C:C: (as Cornelius Osborn called it) was for treating conditions that had some sort of animal spirit related cause–in other words, the philosophy for the time claimed the disease was due to stuck humours, or the inability of the spirit to flow through the body along the appropriate channels. Now, there were some disease that came to be associated with this kind of problem, in particular those in which no physical cure could be produced, and so attempts had to made to come up with a metaphysical causality in need of treatment.
The Sal C:C: or Sal Ammoniac had a follower in Massachusetts during the mid-1600s–Christian alchemist George Starkey. Migrating to Harvard from the Caribbean, Starkey had his own unique philosophy which at the time was very popular and famous, but soon after forgotten almost completely by scientists and unfortunately, the first historians for this period in science history published during the mid-1700s. Nineteenth cecntury and twentieth century science and medical history lacked any mention of Starkey’s influence upon medicine or science as a whole. Reviewing Starkey’s work, it appears there were some socially acceptible reasons for excluding Starkey from the scientific discussions. Starkey was a devoted Christian, and his alchemical experiences came to him through metaphysical means, that were through more of a Christian theological route of thinking than a metaphysical natural philosophy way of thinking. Not to say that Starkey was a true Christian, whereas his counterparts like Robert Boyle were not, but rather to say that Starkey was too much attached to God in his lab books. His experiments came to him or were deduced as revelations and revealed secrets, not through much of any scientific logic. The most famous chemist for the time, Robert Boyle, who represented the transition of chemistry from alchemy to a true science, at first respected Starkey’s findings and claims, but later revoked his support and even came up with alternative formulas for Starkey’s methods to produce the same alchemical, now turned-medicine, end product. By 1670, Starkey’s writings went into storage in a library in England (Oxford?), and were since forgotten (knowledge of these resurfaced due to recent historians).
Durign the 1700s, Dutch-English philosophy in New Negland and the mid-Atlantic region did support Starkey’s philosophy. We learn little about this however during this period of American and European history because it was not discussed much in the scientific literature. Yet, Osborn’s use of Sal C:C:, with reference to it as “Ens Veneris” (the essence of Venus), provides us with evidence for the social knowledge of Starkey’s teachings locally, during the decades just before the Revolutionary War.
The last remnants of Starkey alchemical way of thinking and pharmaceuticals therefore formed the basis for some of the medicine practiced by locals during the early Revolutionary War years. Such a philosophy was not a part of the teachings of the upper echelons in command of the hospitals and such, but these beliefs were prevalent in some local colonial physicians more learned in the local traditions. Were a physician active in the War to make mention of this particular archaic piece of his philosophy, he probably would not have been recruited by Samuel Bard to serve as a Regimental Surgeon. Osborn was fortunately in that either his vade mecum eluding to this philosophy was never shown to the commanders for the time, or that his personal take on this philosophical piece was not taken to be took metaphysical and therefore unbelievable in nature.
As a comparison of the old and new ways of interpreting Sal Ammoniac use, consider the use of thse smelling salts on two patients–the first so ill that he needs to be revitalized after a surgery in order to stay alive, versus a weakened individual in need of blood-letting in order to activate the flow of her energies from head to toe. The first is a soldier wounded in battle, now with a partial amputation of the limb due to gangrene development, the second a women whose menstrual period is late or has been absent for mroe than a month for unknown reasons. To the first, the Sal Ammoniac serves as smelling salts and awakens and revitalizes the weak patient. For the second, the Sal Ammoniac, with the help of bloodletting at the ankle, serves to energize her vital spirits and strengthens the flow of her essence of venus (ens veneris) throughout her body, regenerizing her womb and thereby reinitiating a menstrual flow. The first is a Revolutionary War use for Sal Ammoniac, the second is a local apothecarian use of Sal Ammoniac for the Fishkill area.