The study of plant medicines is what we make of it. Phenomenology is the objectification of something that is very subjective in nature. Science uses its underlying theories to validate a process engaged in by researchers. Quite often it is just theories, not facts, that are responsible for guiding the research process.
Our perception of a situation, our intentions with doing the research we do, that part of our experiences that we are most conscious of—all of these play a role in the conclusion we draw from our observations. This is why a phytochemist who is searching for why something works often finds a reason for how it works, even though this reason is in conflict with other theories found elsewhere in the professional science world as well, be these new theories written at about the same time, or a few years later. We can apply this Occam’s razor phenomenon to the research setting for plant medicines.
Two chemists, searching the same plant, for the same use, are very likely to find two different and unrelated reasons as to why it works–for Pokeweed for example, the high-tech expert relying upon electrophoresis and bioengineering could deduce the reason it works has to do with lectins, the classic chemist would say it is due to the anthraquinones extracted using chromatography. This dilemma regarding the research of plants comes about due to the complexity of their chemistry, and how much scientists know at the time regarding plant chemical groups. Some simple groups like the iridoids have been known to exist for decades, but it wasn’t until recently that they began to be the focus of some studies, because prior to this we had nothing to assign a previously unexplainable and unique plant use to. When I began work on the benzylisoquinoline alkaloids back in 1987, those with well-defined forms of toxicity were well-known, such as the opiates, the hydrastine of goldenseal (and most ironically, never fully studied by plant researchers), and certain cancer drugs and antivirals like the homochelidonines and sanguinarine. The remaining alkaloids were ignored for much of the time, until about a decade ago when someone decided to classify these alkaloids as metabolic agents, producing a new range of studies in phytochemicals and plant use–now we can as scientists understand and define to our content why some plants work as “tonics”, based upon our own philosophy as phytochemists and our own set of philosophical traditions.
Another interesting phenomenon with plant medicine is that when a new reason for why something works is found, scientists have a habit of signing off the old theory in exchange for jumping on the band wagon with the new theory out there. This newer theory then drives most of the experiments that are made, with new scientists hoping to find further proof of this new theory. I have already demonstrated how this is done by early writers defining a use for a medicine, and then testing that use in the lab environment or clinically, to find it to be a success, and then report on these discoveries thereby propagating further use. Then, a generation later in this Pavlovian approach to the science of plant medicines, their hypotheses underlying the mechanisms for success are found to be wrong, and so are changed, although the use of the plant does not change–just the reasoning as to why it works. The plant is still used to treat the same thing, but is provided a new theory as to how and why it is working, updated into a philosophy with more modern terms and concepts. In the classes I taught for nearly 20 years, I referred to this as “Transformation of Common Belief” (TOCB). People change their explanation for something so that they feel more comfortable with making their claims.
Going through the same process but in a different setting, for example a lab, we can develop a theory as to how to identify what kind of illnesses a plant treats or what kinds of bugs or “germs” that plant may eliminate from the body. We can then test that plant for that effect on the organisms, and then separate out its parts and components and test each one of these for their specific effects, and come up with a conclusion as to what part of the plant, or chemicals, appear to have the most influence upon the organism considered a pathogen. We can go into this scenario with expectations, which influence what parts of the plant or plant extract we expect to test. This also influences how we extract the chemicals we are interested in the first place, how we prepare them for experiments, and what kinds of experiments we apply them to, such as a muscle cell, a sarcoma cell, a leukemia cell, mouse skin tissue, etc. We never completely test a plant for all of its parts, just those that we anticipate could be medicinal.
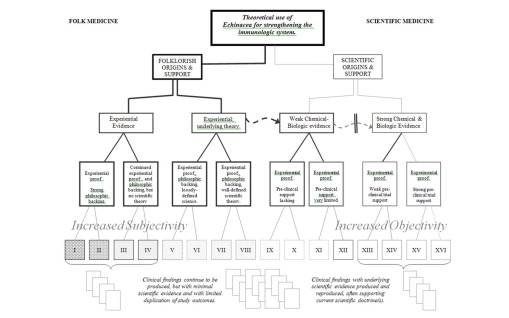
Now there are some special ways that skilled plant chemists engage in their extraction processes, to try to avoid this type of criticism. They separate out the various chemical contents of plants based on particular solubility features, such as ethanol, butyrol, benzene, water, each with neutral, acidic and alkaline versions when applicable, all in order to find out what part is actually working the most. Likewise, there is a way that skilled anthropology researchers and researchers of the soft-science forms of medicine out there have a way to document their own evidence as well. Such evidence is usually experiential and can take the form of qualitative information in the form of stories or tales, descriptions of how a particular event developed, or pre-post forms of proof used to provide substantial evidence to base your final claim upon. In recent years and decades, the proof of “something” is simply just the documentation that “something” happened and that “something else” happened due to this initial “something.” Going back to my two favorite examples, echinacea and plantain, echinacea is what it is because the original cure was nearly eliminated during the early 1800s–Ratibada; as a result, someone researched the same uses for echinacea, but with a new theory in mind based on the assumption that this plant does work. For such a reason the researcher speculated, proof that it works will be found, and in order to market this new plant as a substitute for Ratibada, this researcher gave the plant the claims that exist to this day.
This is how researchers gave birth to the current Echinacea claims. The popular use of Enchinace is a by-product of the once nearly extinguished Ratibada. The uses of Echinacea have been proselytized and hypothesized by the more recent generations of herbalists now for more than several generations. This early 20th century redefinition of the uses for Echinacea were then followed by supporting scientific advances and the non-scientific phenomenological evidence posted out there to back up such claims. Back in the 1980s, some these claims had to be reversed later due to their inherent contradictions and the fact that the idea that Echinacea could boost immune system activities could in fact imply that it will make some serious medical conditions worse. For example in 1983/4 Echinacea was promoted at a national herb school I sat in on as a medical student as the ideal treatment for AIDS, by one of the field’s top notch herbalists who stated that this herb stimulates immune disease responses, the last thing you want to do with an AIDS patient. This meant that this “expert” did not know the mechanisms of diseases which he claimed Echinacea could be effective against. It took herbalists a couple of years to change this teaching to better relate to the mechanisms by which autoimmune diseases work–they chaged their paradigm on how it works and thus kept this belief system alive.
Likewise, the people today who propose a plant for use as a cancer cure, such as plantain, base their documentation on some sort of plant use that does not even pertain to cancer. These people too are guilty of relying upon phenomenology to developed their line of reasoning for why plantain works. Elsewhere I review this interesting history of the plantain and its uses, demonstrating that Erasmus’s non-medical discussion about plantain as a parable in life, was converted into a story with a medical basis by herbalists unaware of the original intent of the story. They misread and misinterpreted Erasmus’s work, saw only its superficial meaning and used that to relate to their take on the world asa a whole in a medical sense. Suddenly this enabled doctors to claim that plantain could be used against spider bites (the toad’s original use was nothing more than as a shelter with the leaf touching its back), then any bite or swelling, then some sort of swollen and infected wound, abscess or cyst, then some form of canker or cancer, since the two were considered pretty much identical except in severity, and then cancer itself, which was never really understood until about 1912 (50 years later), and in modern terms, as a source for iridoids assisting in fighting the terrible cell with uncontrollable replication. With each state of change, all of these transformations of common belief represent a significant change in “faith” regarding your teachings. The initial medical use of plantain was as a passive sanative cure–place a poultice over an abscess and make it erupt. Somehow in a century it has become to some a plant that can aggressively chemically treat tissue and cause it to stop its normal processes and die, a hypothesis completely opposite of the original medical beliefs, a paradigm shift that we believe in just for the sake of believing.
Not that there are no scientific reasons out there to explain why some plants do work very effectively as medicines. Some plant will in fact work for very valid reasons. But once we add that human component to our arguments for why something works, we set ourself up for being discovered as having misinterpreted and misused past historical information in later generations. This can happen in such a way that it can be rather embarrassing to the practitioners and teachers. Presently, the best way to go about making a discovery and arguing its value in medicine is to use hard science to make your discovery and substantiate your claim. Experiential evidence is interesting and often impressive, but is completely humanistic and subjective in nature. We need only go in reverse mode and turn to the historical documents to determine if the sources for such claims are in fact culpable of the same misguidance and errors one should be trying to avoid by supposedly employing the scientific process.
The following illustrates the approach to researching plant medicines when you take a move forward in history. We first find the early mention of the medicine and search for experiential evidence for its validity. If there is some sort of logical reasoning for the events being witnessed, we add even more validity to the situation. We then go through some experiments to validate these claims, and try to work towards producing scientific proof of such claims. The more humanistic the approach to this is, the less reliable the results can be. But to simply test the remedy in a double-blind clinical setting can also produce very unreliable results. We believe this latter case with science is rarely possible due to the strictest of rules and requirements usually attached to performing such studies. So by nature of we default to a semi-blind study or an unofficial double-blind format that doesn’t cost us too much money, and go about testing for results and then validating them objectively and statistically, we risk professional arguments against our findings. The more we can attach “scientific theory” to the findings, the more validity we can assign to it and the medical claim that caused this study to happen in the first place. Even a humanistic study has results which we can attach science to, which is what we do in today’s day and age of herbal medicine study.
For those people engaged in the soft-science approach to validating their remedies, the main steps to take into consideration are those which drive you backwards in time from the testing phase when “Experiential Proof” and scientific reasoning are being sought out. We can always come up with some speculative theory used to drive us forward. The hardest thing to do is look back and see whether or not there are any counterarguments or findings that work against the theory already in the field, which we used defined this cure in the first place. Historical plant medicine in the United States is a fairly hard field to trace back accurately.
If you were to look at something like homeopathy, and find that Hahnemann believed that mercury helps to treat a particular condition, does this mean you have to administer more mercury to get more of an effect? Of course not. The theory Hahnemann works by is the lesser the better, and the condition may not even need mercury in the first place to be treated. When we look at herbal medicine and see that a herb is used to treat a particular condition, is it because that herb is working against the condition, for the body and its own sense of metabolic balance, both? Is the plant medicine sanative–i.e. do you give cayenne to someone with a fever to theoretically spur on that fever (sanative)? or do you make them take a cold bath to bring down that fever (not sanative)? The answer to this question is typically not investigated by the scientist trying to prove that some plant may be useful for a particular drug use. He/She is interested in science, not philosophy.
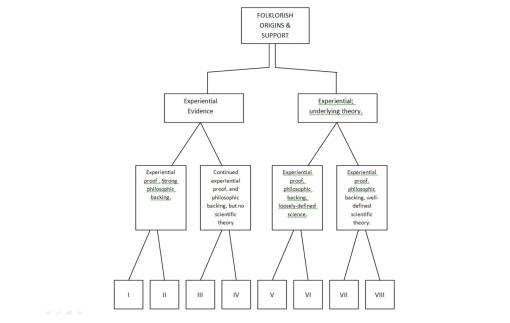
Folklore or Experiential Remedies
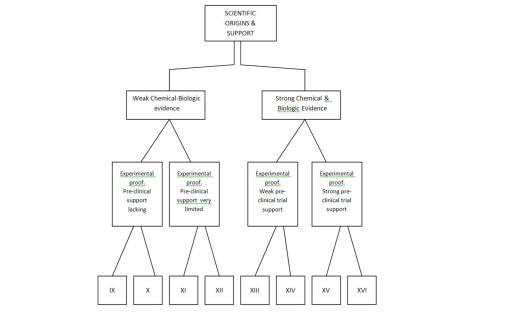
Scientific Remedies
We cannot really detach folklore from science or vice versa. That is really a strong statement to make, but it is pretty much true. Science becomes a folklore when the theories it bases its claims on become invalid, or in the worst of situations, falsehoods, replaced by newer more valid ideologies. So science can overlap with folklore, and in some cases folklore can become integrated into the science world, like the repeated acceptance of acupuncture by medical scientists, at least four times in medical history, due to totally different lines of reasoning based on the understanding of science at the time these acceptances existed and were promoted. Around 1670, science accepted acupuncture for some 4-elements, 4-humours line of reasoning (it worked by fire), then because scientists felt it worked via the “Great Sympathetic Nerve” (18th C) and animal magnetism or electricity, ca. 1800-1840. Throughout the later 1800s acupuncture worked due to assorted vitalism and electricity-magnetism related theories. After all, many scholars speculated, the voltaic and subsequently Faraday machines worked in producing a cure (1860s -1880s), why not the acupuncture needle? This line of reasoning even led the French to lead the study the first methods of treating people with electric acupuncture, a method of treatment very popular beginning in the late 1830s, but continued on and off for decades to come.
Then, science took some major steps in better understanding physiology and the body around the turn of the century. Because scientists could now better understand the nervous system, especially due to the studies on the nerve and muscle, some physiologists probably felt they had finally cracked the theory regarding acupuncture. But then came the theory that acupuncture had an effect on adrenalin (ca. 1890s), and that there might be some effect occuring with the endocrine system and nervous system have some sort of interactions taking place. This argument used by some doctors only lasted as long as it took to make the next important discovery, in what was now a new study–psychosomatic medicine. This was also a very popular theory as to how some remedies work, for which we had no explanations, followed by yet another related to the hormones and psychomotor phenomena (1940s-50s), followed by endorphins (1970s-1980s, due to the missionary visits of Mao Tse Tung’s hospitals in China and Congress’s follow-up on this “discovery” ), and then the whole notion that there could be some sort of psychoneuroendocrinology events taking place, something involving all of the above.
Chances are the theories that are out there now for medicine, are just good for now. They are just theories serving as guiding lights for the western medical profession. Each time this guiding light is blown out, another candle is lit and another new theory generated with a new philosophy to introduce. No only do the medicines we use and have change often over time, so too do the theories upon which these new medicines are based. The reasons they work after all is just that–a theory, waiting for another theory to take its place and a new name to be attached to these “more modern” discoveries.
Again, this is not a criticism claiming that acupuncture does not work. I am simply stating that it is sometimes funny how people, especially scientists, need to explain why it works. They need to crack the shell that surrounds the microcosm of this phenomenon in order to satisfy their own curiosities. They need to have a more comprehensive understanding of their own rendering of their macrocosm, cut down into infinitesimally sized bits and pieces–using their version of Occam’s razor.
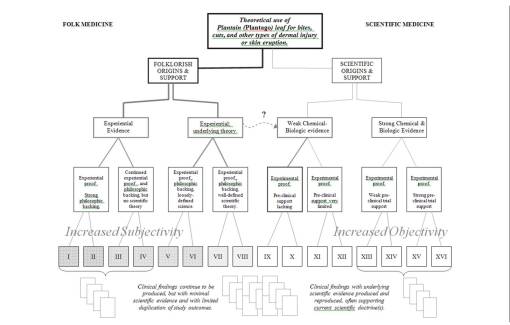
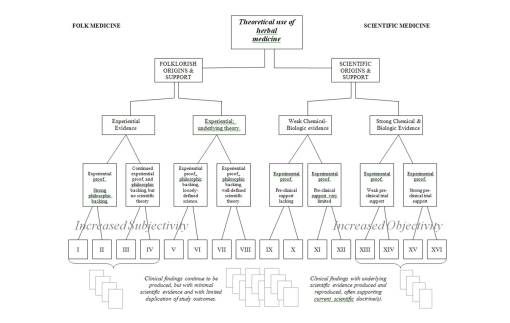
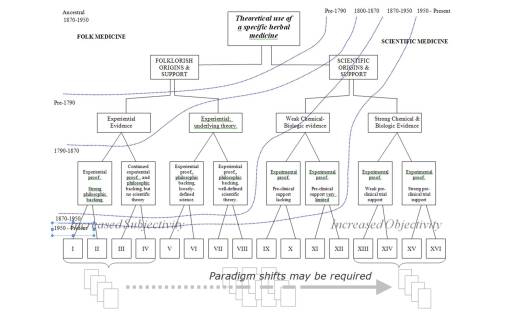
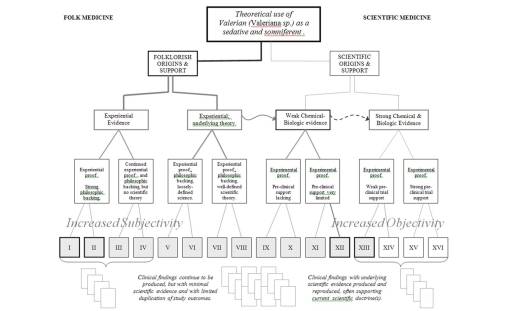
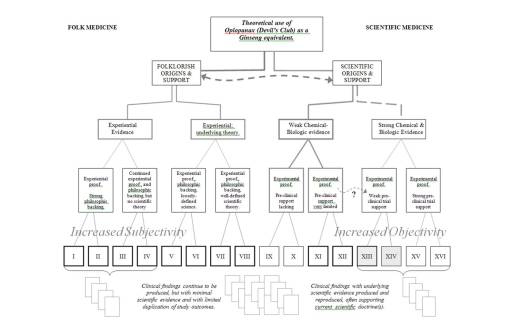
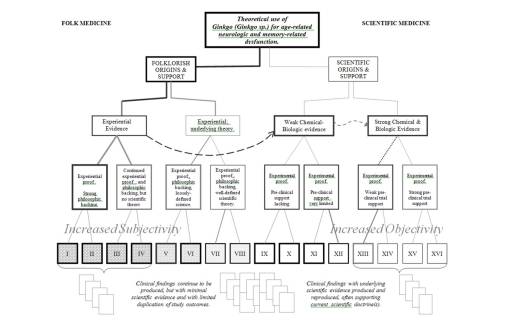
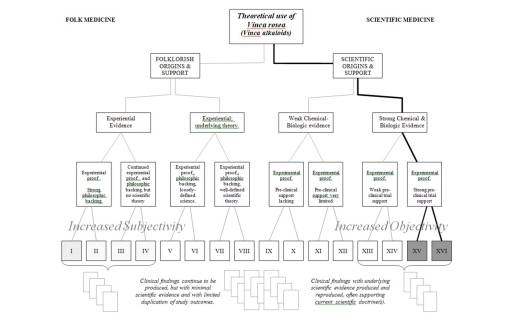
Science has allowed an evolution in our thinking of plants as medicines to proceed along a fairly steady path towards “progress.” We can apply the above two flowcharts into a single chart, and demonstrate how the change from folklore to science is somewhat continuous. With Folk on the left, Science on the right, there is a trending from left to right of methodologies that tend towards increased objectivity as Scientific methodologies become more solidified. The bottom rows (Roman numerals) and vaguely visible compiled results below, represent the arguments each group has to base their premise, claim or theory of success upon. In recent years, we have come to accept some of the more unusual forms of research as evidence for claims and the like, and so methods previously omitted from the studies of the 70s into the 90s, have become more evidence-based, as the scholars like to call it, enabling non-scientific or semi-scientific methods to come into play, ranging from anthropology, sociology and ethnology-based lines of reasoning to non-parametric, grounded theory based methodologies used to assign a numerical value to something otherwise incalculable for quantitative research approaches. These new methods may give us more to do as researchers, and more answers, but not necessarily more absolute findings with which to base out new theory upon.
I have also used this way of separating methodologies used in science and out into groups to illustrate how as science has grown, historical folkloric medicine has it self undergone some sort of conversion process behavioral amongst members of the scientific community. Once this conversion or “paradigm shift” takes place, for whatever reason we cannot be certain, significant amounts of claims, thought and beliefs once avoided now officially become part of the profession in charge. Again, in recent years, this has become known as the evidence-based approach in regular medicine.
.
Applications
The above method helps to provide us with insight into the credibility and reliability of the documentation out there for plant medicines. It tells us where a particular herbal remedy might stand regarding scientific validity, and it puts the background of this information in context with what is already out there for other plant medicines. This method for reviewing plants also enables us to assign a certain level of credibility to the given medical claims. If this method tells us to assign a low-level of credibility due to lack of sufficient scientific findings, it does not mean the plant is unreliable. Instead such a conclusion is telling us just how much more information is needed in order to formulate a half-way decent argument about the claims. It tells us whether or not we have to go back and engage in more research, and it tells us where that special research is lacking in substantial findings.
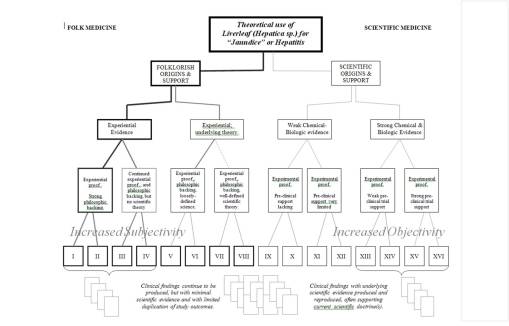
Take for example the classic phytognomics of doctrine of signature plant Hepatica. We know by its name it is associated with liver disease. The form of leaf is triangular like a liver, and the speckling and changing colors on the leaf’s surface resemble the skin of some people with a known liver disease. The following defines where hepatica is distributed in terms of science, pharmacy and medicine.
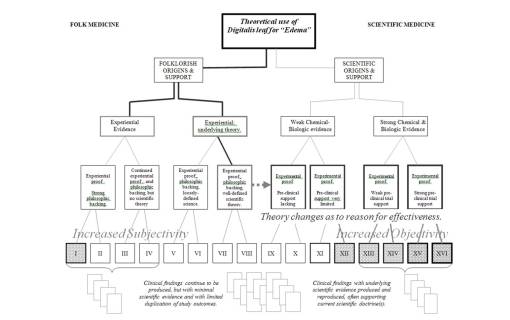
Hepatica is a classic in the Renaissance Herbals. At the time of its publication as a medicine, botanists relied almost entirely on phytogonomics to define their remedies. Hepatica would only remain a liver remedy so long as there isn’t another bit of logic out there to replace Giambattista della Porta’s phytognomics. During the 17th and 18th centuries, when a little more enlightenment in the sciences took place, this enabled experience along with symbols to become more the messenger for doctors on how to use a plant as a medicine. Once science began to take a hold of medicine and there was a little more anatomical and physiological reasoning added to the stories for each plant species, simpler more philosophical methods of identifying plants such as doctrine of signatures became secondary to the other experiences. Since liver leaf rarely demonstrates much of an impact on the body physiologically, it never lost in phytognomic representation, but loses its value in the regular medical system once science began to take over during the nineteenth century. For other plants like Digitalis, the rough and hairy leaves akin to a dog’s tongue (its similar is called hound’s tongue), were forgotten in exchange for trying to figure out why this plant got rid of all the edema in some ailing bodies’ legs. It ends up, these nineteenth century scientists found out, that there is more to a plant than just folklore.
If we apply the above reasoning to medicinal plants the we already know about, we get an idea on the nature of the medical claims being tested, and how they are so different from folklore-generated medical claims. For the first example, consider Strophanthins D and G, two cardiotoxins extracted from the Amazonian plants in the Strophanthus genus. The chemistry of how Strophanthus works, and the physiology and pharmacochemistry behind why and how it works molecularly are very well understood. The proteins these agents work on within the synpatic system are well defined, and the effects of the compound on these proteins responsible for regulating neurotransmitter release and reuptake is so well understood that entire books can be written about the strophanthins, along with the d-tubocurarine, physostigmine, pilocarpine, aconitine, and other plant chemicals that work in similar ways upon other parts of the body’s neurological system. The following depicts the history of this plant medicine from beginning to end, regarding its specific alkaloidal use:
There is a long period of “folk” practice in Amazonia, a transfer of “folk” knowledge to scientists, and an immediately forward progress made in testing and documenting the physiological impact these chemical have at an extremely specific scientific level. Much of the process of verifying the chemistry and its pharmacology is fairly objective, so even if the Amazonian natives had told the scientists that this plant was used for something like leg swelling or stomach pain, the scientific process would have worked out any physiological discrepancies the original claim had. In this case, the original claim was pretty obvious, due to the effects of this substance as an arrowhead poison, so no correction or clarification of original claims had to be made. This was fairly straightforward scientific process, with limited human subjectivity intervening in the final discoveries and resulting medical uses.
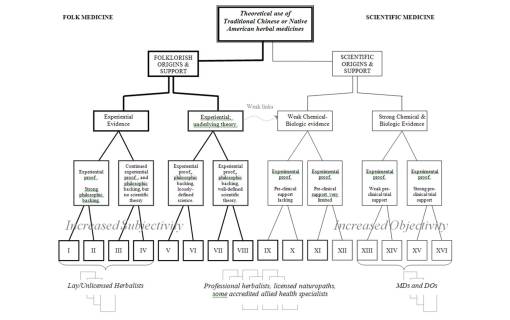
Now lets take a look at this from the other end. If we take a close look at some of the Oriental medical traditions and some of the Native American traditions, we find that many of these plants do not follow the Western Medical or Western Science paradigm. In some cases, a Chinese medicine is professed to work due to its influences upon the Qi (chi) or the methods by which Gu qi is picked up in the stomach, or how the Qi is concentrated down to its “essence” by the kidney. Some of these philosophical perspectives are not as easy to assign a western philosophy to like we could the psychoneuroendocrine or psychoneuroimmunological mechanisms for better understanding how acupuncture works. So, with Chinese medicine, scientists who are not Oriental have a hard time coming up with the scientific reasoning needed for them to continue their review of the medicine. So, they either revert to western traditions and philosophy, and go on to test the medicine, or they drop the topic completely for now, enabling someone else to pick up on this method of treatment perhaps as a psychosocial or mind-body issue. Western minds find it hard to understand the traditional Chinese belief that there is a yin and yang to a mountainside, and that due to this the herb on the east face will have a different pharmacological chemistry than the same herb of the west face of a mountain. Some sign it off as being due to the direct effects of the sun on the plants, others to the different ecological settings that each of these two mountain faces possess. But it is for this reason that a gramina in one setting could be considered important as a medicine, and the other a weak substitute. According to the philosophy, this is due to chi and energy, not chemistry.
Likewise, for Native American remedies, we see a similar mismatch of philosophies at times influencing the kinds of research that are done in with traditional remedies. For the most part, western tradition does take a stronger hold of the information that is presented and transforms it into their way of looking at things (transformation of common belief, which is reviewed elsewhere several times). To the Western European or Euroamerican researcher, the therapeutic philosophy or rationale is wrong, but that doesn’t necessarily mean that the action is wrong–so the particular use of the Native American remedy is tested to see if it does or does not work. In this way, one of the most famous Native American snakeroot cures–Caulophyllum–became a uterine muscle herbal medicine–so what if the muscular effect it once had on someone was a little off, and should have been stated to be uterine smooth muscle instead of skeletal muscle? The claim’s the same otherwise, from beginning to end some herbalists might argue. likewise for the snakeroot remedy Scutellaria–which now treats nervous disorder, another symptomatic philosophical change regarding the effects of envenomation.
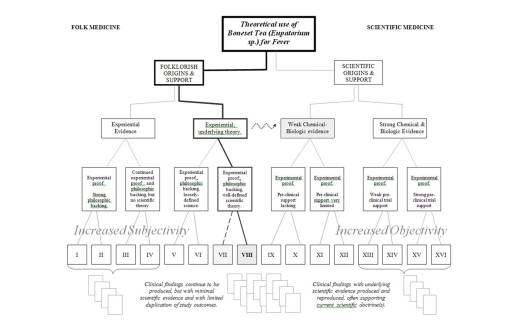
The next example is of a very popular herbal medicine with a significant amount of American history. This herb is documented as being locally important to natives and early settlers, but did not become popular until around 1790/1800 when dengue fever became a problem in the Hudson Valley. This herb known as boneset was used to treat fevers, and has the effect of “breaking a fever” by making person go into a sweat after drinking a tea made from its root or rhizome. Even though it is successful in breaking a fever, the relevance of this use to allopathy since about 1900 is questionable. Fevers came to be associated with many different illnesses, and the use of this herb for treating fevers for whatever reason never became popular to the MD profession during the 20th century. It remains a very popular herbal medicine however, but lacks any substantive scientific proof explaining how and why it breaks the fever. No pharmacological pathway has been defined, such as some mechanism involving the hypothalamus (which I expect someone will come up with–some new effect on the thermal regulatory mechanisms or the like), so no specific drug can be produced and patented based on this herb. So to date it remains a medicine used mostly be herbalists and licensed doctors of various kinds willing to recommend herbal medicines to their patients.
.
Another popular herb with a similar, but somewhat richer more recent history of use is the Echinacea purpurea. A herb that began its current road to popularity with claims that it strengthened the immune system, and in classes given to people on the uses of this plant during the early 1980s, a number of herbalists bragged about its ability to do this. My skepticism towards these claims came about due to the new disease out there for the time–AIDs, (during its first year, it was not yet known as AIDs). These herbalists claimed it would assist in AIDs therapy by stimulating the immune system and therefore could have miraculous effects, but once I mentioned to them that AIDs like numerous other diseases are Autoimmune diseases, in which the last thing you want to do is overstimulate a misbehaving immune system, none of these herbalists caught the drift of this message. This suggested to me their understanding of immune system physiology was not at all there, putting the entire theory into question in my mind from that point on. (Sorry to be so critical to soft science.)
Reviewing the literature, there is limited scientific evidence demonstrating a mechanism for echinacea, although numerous theories are out there about this relationship between Echinacea’s immune stimulating mucopolysaccharides and the ability for a cell to somehow react to a macromolecular substance. Interestingly, this macromolecule has minimal ability to makes its way into the blood due to its size, much less pass through the stomach not at all impacted by the significantly high acidity that is there. These conclusions about the theory for echinacea working on the immune system is still very much open to suggestion and redefinition of course, as science finds another need for us to redefine the theory for this plant’s effects as each generation passes. The following is where echinacea fits in the schema of things regarding plant medicine phenomenology. My conclusion: more evidence is needed.
.
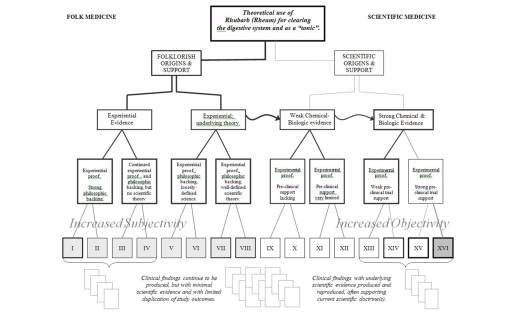
The Echinacea story contrasts greatly with the traditional medicine Rhubarb, a product of China brought to the rest of the world by the explorations of Marco Polo. The effect rhubarb has on the body is fairly basic–it is a laxative, one of many that act by irritating the inner lining of the intestinal tract. This plant has a very strong folkloric background, followed by the early pharmacognostical documentation of its chemistry and mechanism. Its history is typical of many past plants that had true physiologic effects before the dawn of modern medicine, with influences so important they remain acceptable as regular medical practices to this day. Such examples include Senna leaves, Cascara or Rhamnus, and Jalapa, all effective laxatives.
The following example of the Foxglove, which was initially discovered due to its therapeutic effects on patients with edema, provides us with several generations of research experience. This plant with an effective medicine and chemistry provides a fairly solid history regarding it use and effectiveness, thus ending with compete acceptance by physicians. Few plants with a very well-defined folklore history also have very well-defined scientific documentation of their value carried through for several generations. Other examples of plants with such a history could include Cinchona for its quinine, Cephaelis for its ipecac effects, and Caffea for its stimulant effects due to caffeine.
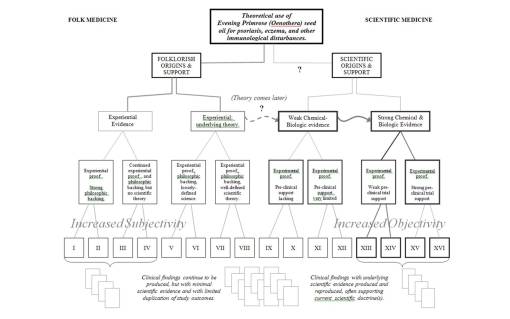
At the other end of the western medical influences are some herbs that are definitely health promoting, but not until recently did sufficient scientific evidence exist to claim and prove this. The following example of Oenothera represents a herb that had a history of cultivation, but no uses at all like those it is currently best known for–immune effects and cardiovascular disease prevention due to its polyunsaturated fatty acid that serves as a precursor to prostacyclins, prostaglandins and possibly leukotrienes. The pharmacological activity of the prostaglandins had to first be discovered before a herbalist could deduce why Oenothera might have some very long tonifying effects–so long in fact that such an association is not really expected in the historical literature.
Using the above methods of reviewing these charts about plant use, the remaining examples are provided as two sets. The first involves three herbal medicines that are borderline regarding potential pharmacological properties are Valerian, Oplopanax, and Ginkgo. The second set of examples details two cancer drugs, one with a 19th century history as a liver remedy, followed by its discovery in the 20th century of being a truly effective cancer agent, the second example involving a tropical plant with a cancer drug. This plant’s relatives have a long folklore history in Europe none of which related to any sort of cancer therapy. This is therefore an example of a very recent discovery without the fame and glory attached to its earlier use by 19th century writers and patent medicine inventors.
.
.
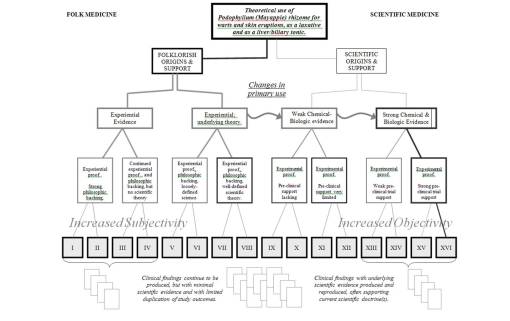
The cancer drugs also demonstrate a reason to take this concept of belief and philosophy into account whenever trying to define a physiologically based pharmacological use for a plant. One theme I like to review time and time again is the cancer drugs phenomenon in plant medicines, and popular remedies for cancer that make heavy use of herbs. The most accurate way to define the status of plant drugs and cancer is to state that post-1960 discoveries of cancer- or tumor-treating herbs are probably more in line with the physiological and pharmacological claims and findings being made than most prior formulas for treating cancer. Prior to 1960, we didn’t know much about DNA, how could we come to understand how a cancer drug that interchelates in the DNA strands possibly work? Drugs that were actually effective cancer drugs, such as podophyllin, were sold as liver remedies (Carter’s Pills), not cancer remedies up until the 1960s. When I was a college kid, I could go to the store and buy myself some podophyllin to treat some recurring plantar warts with. By the 1970s, this use was no longer possible; being a cancer drug, podophyllin had to now be regulated.
Contrast chemotherapeutic podophyllin with the non-chemotherapeutic substitutes out there claiming to be cancer drugs, such as plantago or rheum. The cancer traditionally treated by plantago is not a cancer, it is an abscess, with a use invented in the 1840s or earlier when even cankers due to syphilis or herpes could not be differentiated from an abscess due to staphylococcus. Some scientist today like to believe they are going to find the reason plantago is a possible cancer cure–by identifying that missing chemical that no one else has been able to discover so far. One such phytochemist tried to speculate that the iridoids were why and how the plantago could work. Given a 100% product of that iridoid and placing it directly on a wart or tumor, and shining the right lioght upon it, he could be right–due to free-radical induced destabilization of the biological processes. But this is different than pounding a leaf and using it to form the poultice you are about to treat the growing mass beneath your skin with. Add a little mayapple or meadow rue to that mix and I might believe you.
We know how and why cancer drugs work because of how they work. We were unable to differentiate the true condition that cancer is and its underlying pharmaceutical requirements until the late 20th century. For this reason, cancer drug discovery follows the scientific path, trying to avoid the culturally defined philosophical, misdiagnosed path.
.
.
I should probably mention here once again that I am not against the use of plant medicines in general. Aside from teaching, I spent most of my academic life in the lab devoted to the study of benzylisoquinoline alkaloids distributions for about 60 genera in 15 families, 7 orders, 2 major subclasses. What I am writing this in reaction to is the candor many plant specialists have in and out of academia, in and out of the medical world, in and out of the research lab, about how and why a plant works medicinally or pharmacologically. The phenomenon of the plant’s therapeutic success can be tied to many different things, not just its chemistry. Some plants have a chemical that prevails in its reasons for changing the homeostasis of the body or its physiological process, other plants have physiological effects taking place secondary to other “healing forces” at work. The type of review of plant medicine phenomenology is useful when it comes to putting your work as a scientist or other form of researcher in its proper place. A study of plant medicine is as much a study of the science of folklore as it is a study of the folklore of science.