Adulthood ICDs
Late Childhood/Early Adult, or Young to Middle Adulthood
The teenage-young adult years are usually the healthiest years. The more common ailments during these years are going to be socioculturally caused or predicted, physical ailments linked to social activities and the body’s state, and at times early or continued onset of a chronic disease that impacts these years of life. Those diseases specific to these years, demonstrating a tendency to go away, are infrequent in the ICDs. These are also not included much in the standard HEDIS and NCQA study options reviewed elsewhere during the course of this work, and are only on occasion included in regional and state-requested or overseer-recommended studies of Medicaid and Medicare patients.
The following are two very strongly gender-linked STDs, meaning that they show a tendency to favor one sex or the other in the clinical setting. We know from other STD studies that some gender-related diseases and gender-favoring STDs are tested for specifically in just one population or the other. These diseases are cross-gendered and treated and tested for in both genders, but with tendencies to demonstrate tendencies to present clinically for one more than the other.
[Figure 1: Male dominant ICD with age peak at 24 yo, descending but still high in prevalence until 45 yo; 2nd figure is of female dominant ICD with age peak at 13 yo, and male peak at 26 yo]
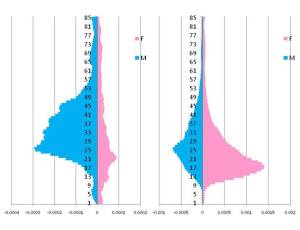
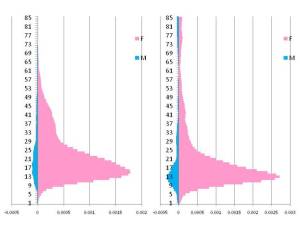
The following pair of conditions common to and strongly linked to late teenage-early adult years are as follows. They are very closely linked to each other, are strongly gender linked and behavioral in nature, with one demonstrating a more aggressive behavior with tendencies to appear into the later post-early adult years. These are examples of two purely sociocultural conditions induced by personal behavior changes, with minimal linkage attributed to genetic cause (although this will no doubt change due to increasing biomolecular technologies).
[Figure 2: two female dominant diseases, with prevalence peaking at 12-13 yo, descending prevalences into 57 yo, F:M ratio of about 100-150:1. Male peak is also at 12-13 yo, but very small.]
The numbers of male cases for both of these conditions also suggest that it is unlikely a genetic cause exists. The possibility of genetics causes is not totally eliminated from the possibilities, but based on the previously described examples of genetic onset diseases, we expect genetic diseases to become progressive once they develop (some do develop or get diagnosed only at later ages), and either cause a mortality that results in reduced prevalences for older patients, or continues to show increasing prevalence as the older age groups are evaluated. The narrow age band for prevalence in males for these two ICDs suggests a culturally-induced change occurs–these people no longer have that medical problem once they reach their late 20s and are required to be ‘more productive members of society’ (using the common paradigm and lingo). The first condition, the worst of the two, has a malingering age-related incidence curve; the second has a very narrow band, again link to sociocultural definitions, interpretations and related human behaviors.
.
Middle to Late Adulthood
The middle to late adulthood years should be interpreted behaviorally and socially as the peak periods of cognitive behavior, physical and mental work productivity, high rates of healthy or recreational as well as unhealthy behaviors, and high stress related disease like consequences due to the lifestyle decisions that have been made are actively and regularly engaged in.
The diseases that present themselves during this age band can be interpreted as socially defined events, often even outweighing the biological nature of their onset. This could be interpreted as the psychosomatic period of life, with peaks for those ages and disease patterns most often linked to psychosomaticism (as defined especially in the 1940s and 1950s, and perhaps early 1960s). The contemporary medical philosophy relates many of the contemporary diseases with established pharmacological therapies recently developed. These unique neurochemical explantations did not exist during the 1940s to 1960s when a lot of the diseases we see with this midage peak had a link to some sort of psychosomatic origin.
For each of these conditions there is a peak age followed by a drop in prevalence (remember, relative prevalence rates use a formula that automatically corrects for this annual mortality rate). This drop in prevalence is due to reduction in psychosomatic behaviors, perhaps as a result of age-specific sociocultural changes expected with the post-retirement years.
The following is a basic form these kinds of conditions produce when evaluated using the new statistical method.
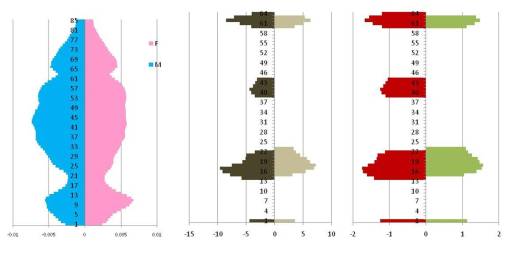
[Figure 3: bimodal peaks: 13 and 42 yo, M and F. Very rounded curves directed towards peaks. Application of new statistical formula used to compare and contrast prevalence and counts statistically using new methodology, demonstrating stat sig in three narrow age bands, per gender, for — M: 14-22 yo, 38-45 yo, and 60-65 yo; F: 14-23 yo, 60-63 yo, 38-45 yo peak for stat sig prevalence not produced. The first pyramid is N, the second a stat sig/sig diff evaluator, the third formula relies upon the second and smoothens out results to define max-min for intervention age ranges used to initiate focus groups and targeted intervention plans.]
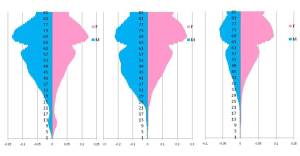
The following are examples of the types of outcomes generated with this formula and methodology (just relative prevalences are displayed):
[Figure 4: varying multiple peak graphs with distinct age-gender behavior differences. Fig A: F >> M but otherwise symmetric, Fig B: F>>M at all working age backs, and M decreasing significantly by mid 20s; Fib C: F >> M, with disease progressively worse with age, indicated by prevalence peaking around 47 yo, versus M peak at approx. 32 yo.]
Notice how the first two demonstrate relatively early onset, one with relatively early reduction in prevalence for assorted reasons, the other due to its early mortality. In the second example there is a significant difference in relative prevalence for deaths during the reproductive years, with males more likely to die due to this problem, ten years before the women experience the mortality of their condition. If this was a behavioral psychology form of disease, this would have social implications in needs of further pursuit. If this were a genetically-based disease, such a finding could have tremendous moral implications. If it were some physical disease brought on by health related activities and behaviors, its sudden changes in mortality for men versus women at 20 years of age may be preventable.
The third example above is a disease with primary manifestations in the middle years of life. Like the first its relative prevalence for females is greater than that for males. The question to ask is why the reduction in prevalence from about 45 years of age and older? Since these are prevalence rates based on gender-age-adjustments, it represents a true reduction in mortality rates from 45 years on. This condition is a physical manifestation with possible environmental and mental health related autoimmune related causes, implying the gender differences are complex and hard to define, but result in a reduction in mortality rates in 1-year intervals from 45 on. The slopes for male versus female prevalence rate changes pretty much remain identical and unchanged for the remaining lifespan, until the two rates are once again equal.
The following are life long conditions with age demonstrating a direct relationship to risk. Individual survive a long period of disease, but then due to mortality changes begin to show a reduction in relative prevalence as age increases. These are 3 of the most common causes associated with mortality and quality of life during the midlife and older years. These curves are identical for a number of other similar chronic diseases that exist as well, with similar mortality relative prevalence rate age-gender relationships.
[Figure 5: three ICDs with age of significant onset around 27, and prevalence increasing to peaks shared as approx. 72 yo. Subsequent reductions in prevalence are due to mortality.]
Key to Figures
-
Syphilis, Early Stage, and Chlamydia
-
Bulemia, Anorexia Nervosa
-
.
-
.
-
.
Related Pages
- Preface
- Evaluations based only on Prevalences – Stages in Life
- ICDs related to Newborns and Young Children
- Three Progressive Conditions – Mid to Late Childhood ICDs
- Late Adulthood ICDs
- More on Gender Specificity
- Other Statistical Behaviors
- Psychologic and Psychiatric Disorders
- Conclusion
- Appendix – Exercises

Leave a comment