Physicians learn to use Indigenous Remedies
In a number of colonial settings, scientists, physicians and scholars tried to document their experiences, either first hand or second hand, pertaining to the use of local plants as medicines. During the earliest years of the 18th century, most of the herbs discussed were presented singularly or just a few at a time. It was commonplace to find descriptions of the plant medicines, as well as others forms of medicine, included as part or a much larger writing on a particular Colony or community setting. Sir Walter Raleigh’s writings on the New Virginia region included stories about the highly valued starchroot commonly found in China (“China-Root” or Smilax sp.), the sunflower, and severally locally identifiable medicinal plants. In early 18th century New York history, Cadwallader Colden discussed in details the values of several medicinal plants growing on or near his land. By the mid-18th century in Pennsylvania, John Bartram, a naturalist, botanist and scientist in that colony, took ample amounts of notes on the uses of local plants by Native Americans and even the African slave cultures residing nearby in the tobacco-growing regions.
These early experiences with local plants are most important to American medical history in that they helped to define the importance of local plants as medicines in the decades ahead. It wasn’t until the cost for buying medicines made with plants from other lands became too high that the use of the much cheaper local substitutes came to be appreciated. By then, many local communities already had their trained specialists in this type of practice. Late 18th century and early 19th century American plant medicine was a limited specialty when it came to teaching regular medicine.
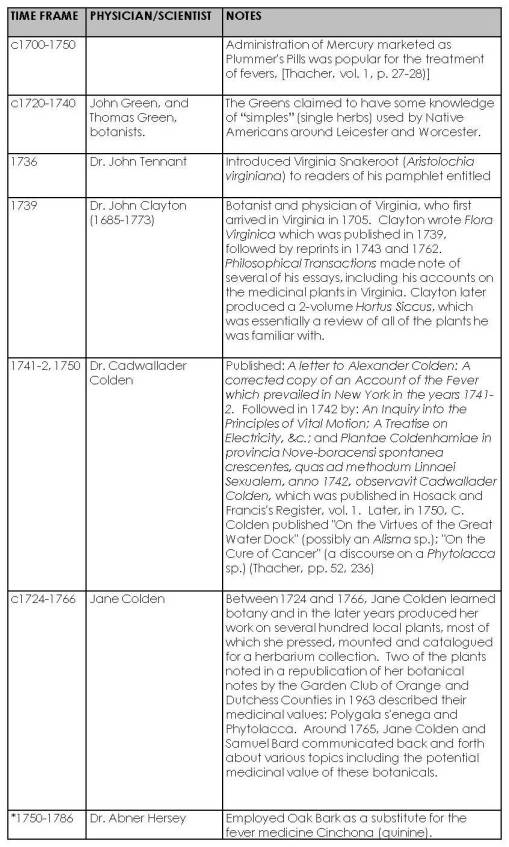
The following tables details some of the people contributing to this phase of American herbal medicine history in the North American Colonies.
1750s and 1760s
From 1750 to 1760, a Native American-derived medical discipline was being practiced by poorer colonial families in New Britain. During this period, substitutes for the South American herbal medicine of high repute, cinchona, were sought out due to the high cost of herbal medicine imports. During the upcoming years, the use of oak bark as a substitute for cinchona was published and then popularized by Dr. Abner Hersey (1721-1787). According to Dr. Cornelius Osborn’s recipes in his vade mecum, the bark of Cornus florida (Dogwood) may have also been used as a cinchona substitute, although this may have remained a use of the bark not accepted into the pharmacopoeias for quite some time. By the 1770s, Oak has become an acceptible substitute for Peruvian Bark, which Dr. Abner Hersey included in his regimens consisting of prescribed milk diet, mercury, the antimony-based Lockyer’s Pills, Plummer’s Pills, emetic tartar, Turpeth mineral, ipecauanha, contrayerva, calomel, camphor, chalybeate medicines, and Sydenham’s liquid laudanum recipe. (Thacher, vol. 1, p. 293-294)
In 1750, a fairly small document was produced detailing the local herbal remedies by John Bartram of Philadelphia. The important contributions Bartram made with this short treatise was the inclusion of African slave herbal medicine use (3 species) and the value of Lobelia inflata, a plant that would later change medical history due to its popularization by one of the United State’s most successful instigator of alternative medicine during the early 1800s. [For more on John Bartram’s medicinal plants, 1750, see related blogpage.]
The first sizeable review of Native American herbal medicines ending up with a single document was produced by Aeneas Munson/Monson (1734-1826). Born in New Haven, Dr. Munson/Monson attended classes at Yale and graduated in 1753, after which he entered a study of Divinity, due most likely to his declining health during the early 1750s. This professional decision led him to learn medicine under John Darly of Easthampton, enabling him to begin his practice as a physician in 1756, in Bedford, New York. A year later, after removing New Haven in 1760, he produced a review of his findings on the value of the local herbs. According to Thacher, Darly was one of the founders of indigenous medicine as it would be practiced by regular physicians in the United States: “…he procured and studied the most recent and celebrated works; obtained specimens of new and important substances; made many experiments in pharmacy and the kindred branches of physical science, and allowed no valuable improvement to escape his observation. He first introduced many indigenous articles of the materia medica into regular practice, and laid the foundation for the study of that important branch.”
The next learned scientist and academician to strongly influence the local medicine was Alexander Garden (1728-1792). Born in Scotland, Garden removed to South Carolina about 1750 and from there to New York in 1754, where he held a professorship in the local college. During the upcoming year, he established a formal connection with Cherokee Indians beginning in 1755, during which time he discovered a form of earthen material sufficient to make pottery with. Removing to Charleston about 1760, he soonafter documented and introduced the medicinal value of Carolina Pinkroot (Spigelia marilandica L.), which was published by 1764. Alexander Garden would later contribute to Jane Colden’s work, leading up to her discovery of a plant which was originally named Coldenia by her. This plant later be known as a species of Gardenia, followed by Hypericum sp., its actual name. (Thacher, vol. 1, p. 269). Since garden and Jane Colden were known primarily as botanists, making occasional notes as to the ethnobotany of these plants, their work helped to set the stage for later identifications of plants considered highly important as medicines. During the upcoming years, more theses would have to be produced by the local medical school students and more dissertations published on the local indigenous remedies before substantive amounts of evidence could be used to define an actual materia medica or pharmacopoeia making use these plants.
During the remaining 1760s, the Bard family made the most important contribution to native plant knowledge, both locally along the Hudson river as well as throughout numerous other parts of the Colonies. Thacher recalls one note he read in which physician Samuel Bard inscribed for his father John Bard, the following note in 1765: “From the Author to Mr. Bard, as a small tribute of respect due to his success in cultivating botanical knowledge.” (dated ‘Edinburgh, May 15th, 1765’). By 1765, John Bard had changed his place of residency to Hyde Park on the Hudson.
About 1767, Dr. James Hurlbut (1717-April 11, 1794) of Berlin, Connecticut made a series of indigenous botany related contributions to regular medicine. Book-read under a Dr. Osborn of Middletown, Hurlbut (like Cornelius Osborn of Fishkill, NY) was well acquainted with the works of Hermann Boerhaave. Hurlbut also had some knowledge of indigenous plants, which Thacher refers to as follows: “Dr. Hurlbut’s knowledge of our indigenous materia medica was probably superior to that of any other physician of his time. The blood root, geranium, the asclepias, the cornus, the trillium, and other native articles were in common use in his practice. He often directed the potentilla norvegica in strangury and other affections of the urinary organs under the common name of dropwort, and from repeated trials the writer is of opinion that it is more useful that uva ursi.” He also makes mention of the uses for “Dropwort” (Spiraea spp.?, and in another materia medica discussion noted the value and uses for alcoholic beverages and opium. According to Thacher, Dr. Hurlbut ultimately suffered the consequences of these two preferences, by becoming addicted to Opium during his later years (Thacher, vol. 1, p. 307-309).
1770s
Progress made during the 1770s brought indigenous medical knowledge still closer to the first American physician’s pharmacopoeia. In the years just preceding the Revolutionary War, Marshall Spring (ca. 1742-1818, a 1762 graduate of Harvard, earned the name “quack” according to Thacher who called him “a man professing skill in the nature and cure of diseases . . . [with] his own views of practice.” Thacher claimed that Dr. Spring often applied diet and regimen curing techniques, but made use of very little medicine, “always giving nature fair play.” It is possible that this form of practice was actually the result of a strong religious upbringing on Dr. Spring’s behalf, although Thacher makes no mention of this part of his life. It is also possible that Spring was a practicing Quaker or Quaker-advocate, in which case “always giving nature fair play” is little more than the simple sanative healing practices often engaged in the more strongly devoted religious healers and doctors. In spite of Spring methods of practicing medicine, he never seem that far out of touch with the status quo, for which reason he would later service General George Washington and the American Army during the upcoming Revolutionary War. (Thacher, vol. 2, pp. 98-103).
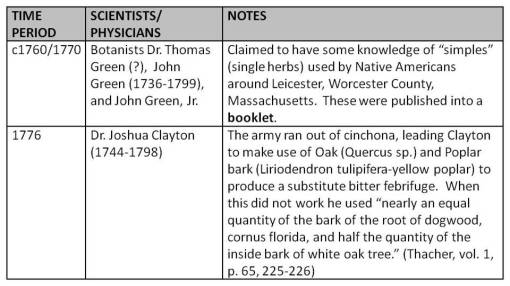
During the late 1760s and early 1770s, Dr. Thomas Green (by-dy?), John Green (1736-1799), and John Green, Jr. (1763-1808) began documenting in writing what they had learned about the use of local botanicals and soonafter produced a booklet on this topic. The Greens lived in Leicester, Worcester County. Physician Thomas Green had a proficiency in the knowledge of simples due to his conversations with the Natives, and may have begun to gather this information as early and the mid-1700s. Ultimately, with the help of his son and grandson, the family was able to produce a small booklet or pamphlet style of writing on this topic. According to Thacher: “By the aid of his book, and the knowledge of simples, a proficiency in which he early acquired by an intercourse with the Indians, he was soon enabled to prescribe successfully for the simple maladies of his fellow settlers.” Thacher, vol. 1, p. 273-274)
One of the most important contributions of the local ethnobotany information made its debut into American history in 1776, following the commencement of the Revolutionary War. One of the physicians serving at this time was Dr. Joshua Clayton (1744-1798), born in Dover, Delaware, on July 20, 1744. Dr. Clayton served during the first wintertime freeze experienced by the troops in Valley Forge. This wintertime was essentially a “miniature ice age” according to some historical climatologists, during which time fever struck the American troops and filled the local hospitals. Quite quickly, the army ran out of the highly valued cinchona bark imported from South America, often by European vessles. This led Dr. Clayton to make use of Oak (Quercus sp.) and Poplar barks (Liriodendron tulipifera-yellow poplar) to produce a substitute bitter febrifuge: “During the late war the Peruvian bark was very scarce and dear. I was at that time engaged in considerable practice, and was under the necessity of seeking a substitute for the Peruvian bark. I conceived that the poplar, Liriodendron tulipifera, had more aromatic and bitter that the Peruvian, and less astringency. To correct and amend those qualities, I added to it nearly an equal quantity of the bark of the root of dogwood, cornus florida, and half the quantity of the inside bark of white oak tree. This remedy I prescribed for several years, in every case in which I conceived the Peruvian bark necessary or proper, with at least equal, if not superior success. I used it in every species of intermittent, gangrenes, mortifications, and in short, in every case of debility.” (Thacher, vol. 1, p. 65, 225-226) It helps to note here that this recipe was produced with a focus on the color white, the matching humour for which was mucous or phlegm. This suggests that the physicians had already been able to differentiate this wintertime fever epidemics (such as from influenza) from the epidemics common to other periods in the years such as the malaria, dengue, and breakbone or yellow fever epidemics, each of which would have required a different recipe bearing different underling colors and matching humours (malaria and yellow fever = yellow; dengue = black(?)).
The Immediate Post-War Era
Immediately following the end of the Revolutionary War (the Peace Tray of Paris was signed in 1783). Rev. Dr. Manasseh Cutler, Hamilton, Mass., Hon. Member of Mass. Med. Soc., presented to the Academy of Arts and Sciences “a valuable account of indigenous vegetables…the produce of New England, botanically arranged…very numerous, and may be considered an honorable attestation of science, at a period when the subject was almost entirely neglected.” (Thacher, p. 41) [Cutler’s writings published as part of the Academy of Arts and Sciences, vol. 1. c.1784]. Reviews of Cutler’s writing and the writings of other early post-War medical botanists are provided on separate pages.
During the post-war period indigenous remedies took several routes to becoming a part of the the now Euro-american, post-patriots for of medicine. During this time frame, several philosophies about health and disease took hold as well. These two series of events and changes in philosophy and tradition crossed paths at times and then separated once again to form individual movements or followings in the original 13 colonies, now states. The philosophy for disease at this time pretty much ignored much of the teachings that William Cullen and his followers the “solidists” were promoting prior to and during the early stages of the Revolutionary War, and the counterforce to this tradition–the brunonians who believed in atomism and something akin the humors–was not faring so well either in terms of belief systems regarding disease and health. The natural forces were better understood by now, with a natural philosophy relating such natural events as lightning, thunder, earthquakes and terrible storms to events that may relate to how the body itself maintains a stable sense of being and health. Medicine had become a philosophy that focused on the natural settings, with climate and weather two of the chief causes for disease, and tha ability of the body to adapt to the environment or be protected from these natural energy linked pathogens the most important concepts in disease preventing activities. Such a natural philosophy was very much extracorporeal in its nature, unlike its parallels confessed to several decades before by some traditionalists, like the three organ system vital energy or vitalism concept (a trinity version of the Oriental pnilosophy consisting of yin and yang and the varieties of chi in the body, so to speak) popular to this region due to the Dutch traditions–the philosophy of vitalist Theophilis Borden.
Philosophy is never exactly parallel to or a part of herbal medicine tradition. Therefore, these exercises in natural philosophy and medicine did not always match up exactly with how herbal medicines were selected and used by people. We see this with the incorporation of local plants into the European-Euro-American-early United States materia medica. Plants become a part of the local materia medica because either they adhere to the user’s natural philosophy and medical-disease belief system, and/or because they have a use that can be rationalized and made into some sort of story that matches the herbalist’s belief system. By knowing the traditional philosophy for their use, healers are faced with the problem of making that belief system match their own. In this way the snake spirit is no longer a spirit, but becomes a doctrine of signatures argument, and the notion that there are important differences between an east facing trunk bark and a south facing trunk bark become a physical appearnace related concept–the darker bark is considered more medicinal due to its color and related chemical concent (chemicals in plants were just beginning to be understood in the late 1790s). This chemical based philosophy also enabled practitioners to detail the differences between stronger remedies like the mienral drugs and the much weaker herbal drugs–the former was toxic and less “natural” to the body than the latter, although at times mineral drugs like Iron were know to be better, only just too toxic at times when it came to symptomatology.
The indigneous remedies came into medicine along a route which allowed them to be used as standalones and substitutes for the increasingly popular mineral remedies regular doctors were promoting. Individual residing outside the economic reaches of regular medicine and its drug sellers made use of the local traditional medicines, adding to this the touch of realism and natural philosophy–God placed these remedies there for you to learn how to use, a very convincing pastoral style of arguing for herbalism and indigneous remedies use. Mineral remedies may be theoretical and “ideal”, but herbal medicines were safer and “real” to many experienced in their uses.
Only later did regular doctors learn more about the indigenous remedies, enough to add their to their pharmaceutical repertoire. In a way they are late comers to this style of practice and its base knowledge, something never fully discussed about regular medicine and its alternatives. It takes regular doctors two or more generations to accept and allow for changes in treatment protocols, even then, the new drugs regular physicians tended to incoroporate into their treatment modalities demonstrate a fairly slow, overly cautious and sometimes stubborn learning curve–cautious only because they themselves did not make these discoveries.