.
Today’s Texas Fever refers to the desire to be in Texas, to be Texan in how you live your life and make money (usually this is in reference to” Texas Gold”.) The other “Texas Fever” pertains to disease, which has a two-part history. The modern use of the term Texas Fever in reference to health refers to Babesiosis, a disease brought about by a protozoan that causes malaria like symptoms in its victims. The name for this protozoan is Babesia microti. The Texas Fever that is the topic of this page refers to another disease born by cattle, one that was spread by cattle drives during the late 1800s. The first time the term “Texas Fever” became popular for something relavent to Texas Cattle drives occurred some time between 1840 and 1845, when cattle raisers in Missouri lost the majority of their stock just a few days following the passage of a herd of Texas cattle feeding on the local range.
The popular opinion for the time was that Texas Cattle carried with them a disease, either in the form of contagion in their body or some form of effluvium or miasma they released by spending a few days in the immediate area eating the local hay and prairie grass. This suspicion did not sit well with Missourian cattle raisers and of course it was contested every step of the way by Texas cattlemen. According to Texans, the Missouri stock were weak herds. It wasn’t that they couldn’t tolerate the results of Texas cattle feeding on their pastures as much as it was the inability of Missouri cattle to adapt to the Midwest. Unlike Texas cattle, which were raised in the Midwest, mostly in Mexico, Missouri cattle were only a few generations into surviving as Midwest stock. Like generations before, this gave some cattle raisers a sufficient argument to claim that some form of the survival of the fittest was taking place following the herding of Texas cattle across Missouri prairielands. To Missourians, the death of so many heads just a few days apart from each other following departure of Texas livestock said there had to be more to this than just a result of nature.
The result of this experience was the passage of some of the first laws on animal migration for public health and animal health related reasons. Texas Fever provided us with important insights into the ecology of disease, the mechanisms by which certain diseases can be born, and the need for better quarantining practices with the goal of preventing the spread of animal born diseases. Our basic knowledge of animal versus human diseases, the roles which animalcules played in disease development and propogation, and the importance of understanding endemic and epidemic disease behaviors and patterns, all enabled physicians, farriers and farmers to come up with adequate laws to prevent the loss of important farm-derived food stores.
.

Before the cause for Texas Fever was known, its environmental requirements were already understood. Even after the bacterial theory for disease patterns was accepted, epidemiologists researching Texas Fever remained focused on the ecological and natural history of the disease and its victims, the cattle. Once the microorganism related to its cause was discovered, this better understanding of the disease was over time minimized. Quarantine practices were developed with the assistance of the United States Department of Agriculture, but for the most part we never learned about the biology and ecology of this disease or its organism in contemporary writings.
Texas Fever is an example of a disease that has the potential of creating significant impacts on human health and disease due to the manner it which it enters the human dominated food web. The cause for Texas Fever is limited by the distribution of its vectors, the ticks that exist alongside cattle born and raised south of the latitude separating its current endemic region from its potential epidemic region. To illustrate this method of disease modeling, several methods of interpreting zoonotic and anthropic disease are applied to this review of the geography of Texas Fever. These same methods may be employed to research other animal borne or environmentally related diseases to the human experience for these non-anthropocentric disease patterns. The work of Gerald Pyle and Russian medical geographers/disease ecologists like Pavlovski and Voronov are the focus of this approach.
The ever-evolving disease patterns related to pathogen ecology, and the more recent concerns regarding bioterrorism and the infection of people, animals and crops are the basis for engaging in this kind of research. Instead of beginning the ecological study of disease patterns from a new point of view, primarily epidemiologically based focused on the organism first and the more complex environmental relationship second, this method recommends that first an ecological and environmental approach be taken to studying an zoonotic or zoonotic-anthropic disease behavior. Such methods of interpretation were brought about by medical geographers worldwide throught the early 1800s, but allowed to remaina part of the more modern ways of modeling diseases mostly by Russian geographers from 1930 to the 1980s. It is only in very recent years that American geographers have been able to catch up to some extent with these other interpretations of spatial epidemiology, unfortunately perhap, with too much focus upon recent and contemporary focus once again on people and microbiology, instead of the more applicable views of natural ecology, absent of the focus mostly on just human involvement and interventions.
.
Murrain
Before Texas Fever came to this country, there was murrain. Murrain was the fifth of seven plagues that struck Egypt, just prior to the freeing of the Jewish population led by Moses. This term, ‘murrain’ over the years has been used to refer to numerous sheep and cattle diseases, but especially rinderpest, erysipelas, foot-and-mouth disease, anthrax, and a number of streptococcus infections. For this reason, throughout the centuries of European history, a number of diseases considered to be murrain had significant impacts on the health and wealth of many of the European farming communities. The most famous of these were the cattle plagues that struck parts of Western Europe and headed Eastward during the 14th century. But other early recounts of this plague refer to its presence in the 16th century and 17th centuries, suggesting the origins for many of these later diseases to be parts of Europe and not just of African or Egyptian origins.
The first epidemic form of murrain of importance to North American and ultimately United States history was born in the mid 1700s, probably in England or Holland. Cattle were an important part of the commercial products transported to the colonies during this time, and murrain was a common problem to the cattle farms in Great Britain. By the time murrain became a concern of American farmers, animal surgeons had learned to differentiate it from many of the other forms of cattle disease for the time. Like human diseases, the cataloguing and differentiation of animal diseases depended upon symptomatology, location and living conditions. With the exception of several worm diseases, there was no knowledge of the causes for these diseases at any microscopic level. Poor sanitation and the environment were usually assigned such blame. The rinderpest, erysipelas, foot-and-mouth disease and anthrax each had their unique presentations and symptoms being documented by the late 1700s, enough to distinguish many of them from each other by 1800, but determining where the animals were most susceptible to these diseases required a unique set of skills and experiences.
There were also a number of cattle diseases that were unpredictable during this time. They were difficult to distinguish from other illnesses with similar symptoms such as fever, drooling, scabbing and scaling of skin accompanied by depilation. The cattle-born lung fever or consumption was one such disease that suddenly struck United States cattle around this same time in United States history, ca 1850. The second such disease that made its way into the country during this time was Texas Fever, at first considered to be just another form of murrain common to east coast states. But without the exact knowledge of the causes for each of these forms of murrain, animal doctors, livestock owners, and government officials had a difficult time distinguishing cattle fever from the previous murrains for the next several years.
Geography played an important role in helping doctors and farmers tell these disease apart due to their very unique symptoms based upon regions. In Kentucky, Tennessee, and the Carolinas there was the traditional murrain. In Nebraska, Missouri, Ohio, Indiana, Illinois, and even New York there was this dry murrain that developed, characterized by the obvious– dry mouth instead of drooling. When the Texas Fever became a part of the murrain story, its differences from the other two murrains, in place not necessarily in signs and symptoms, told some of the scientists and farmers that this was a new disease, a murrain true to its name as a part of the Mosaic history of murrains told in the Old Testament. This murrain was fatal in large numbers and in just a few days, like the fifth of the seven plagues.
So, the first task of midwest livestock owners and doctors became distinguishing the three forms of murrain common to their settings. The traditional European form of murrain, Nebraskan Corn Fever and Texas Fever all had to be differentiated. The mapping of transportation routes, cultural migrations, the environments where these fever struck, and the various topographic and climate features of the most disease prone areas had to be differentiated. This medical geographical process for reviewing Texas fever enabled Missourians to define a means for its prevention. It took other veterinarians, cattlemen and politicians another decade or two to learn that the Missouri way of managing Texas Fever was not only accurate, but the most correct way to initate an animal-focused quarantine process.

The Differential Diagnosis
A minimum of three kinds of murrain struck the cattle during the late colonial years in North American history: traditional murrain, dry murrain and Texas fever.
The traditional murrain was a kind of fever that struck the cattle and later led to the deterioration of their body both inwardly and outwardly. Some of the first symptoms noted for this plague were the catarrh along with a fever. In time, this also came to be known as the bloody plague due to the expression of fluids from the body. In some parts of the world this bloodly plague was considered endemic to the region, like in England. The bloody murrain from England and Holland is the main plague to strike North American livestock farmers during the late 18th and early 19th centuries. Its diffusion into the interior of this country occured by way of east coast wharfs and railways. It is known to have reached Ohio by the 1830s, if not a decade earlier, thus setting the stage for a sense of confusion to develop when Texas Fever later struck the midwest.
This form of murrain–bovine tuberculosis–is more completely reviewed in the two essays preceding this page. The first page reviewed the 1797 case of bovine tuberculosis in Connecticut. This original murrain referred to as “Bloody Murrain” in Western Europe. The U.S. farmers sometimes used this term to differentiate it from the “Dry Murrain” that infected lower and upper midwest cattle, displayed by a very different set of symptoms. The Bloody Murrain became the first murrain to migrate into the United States and have a major influence upon the United States cattle industry. Originally considered deterimental to the livestock industries in western Europe for more than a century, especially during the 1800s following the war of 1812, it was also considered proof that nationalism and separatism were important to survival in North America. Our livestock meats and farming goods were healthier and more important than any European imports.
During these very early years of the U.S. “murrain” epidemic history, other epidemics at times were referred to as possible examples of murrain. The horn disease or anthrax is the most known of these although enough understanding of anthrax was developed by 1810/1815 to allow for adequate differentiation of this disease from other cattle diseases. But anthrax is not at all related to murrain and was easily differentiated from the murrains farmers were concerned with during the early 1800s.
.
The second murrain to strike the midwest was “dry murrain”, commencing some time around October 1843. This murrain lacked the catarrh so typical of traditional murrain, and was especially associated with corn-fed cattle. Also known as corn-fever, it was especially prevalent in the western states like Nebraska. Like the eastern murrain (bovine tuberculosis) from Europe, this murrain was fatal to cattle whereever it prevailed. Until it’s true source was discovered–the fungus responsible for corn smut–this cattle endemic disease pattern was attributed to many of the same causes for traditional murrain, including environmental features like humidity, miasma, putrescence, and other forms of natural poisons and pathogens.
In spite of the increased watch on European imports like cattle and other foods following a resurgence in murrain cases, watches had little effect upon the import of Texas Fever into this country. Fortunately, a number of advances in science and scientific observations prevented physicians from associated the Western European and dry forms of Murrain from the newly discovered Texas version, enabling inspectors to improve their surveillance skills over time.
The third murrain to strike this country is the topic of this review–Texas Fever. The following article noting it presence was published in 1855, and probably marks the initiation of a second surge of this disease, perhaps imported from Mexico.
Newspaper announcement of the arrival of the epidemic, murrain. This term originally referred to the fifth plague in the Bible [Exodus 9:3]. It later became a term used to refer to sheep and cattle epidemic diseases like rinderpest, foot and mouth, anthrax, and a variety of streptococcal infectious diseases ranging from skin rash, scarlet fever and sore throat, to rheumatism, muscle wasting disease, and kidney failure.
During the 1840s, the first cattle drives out of Texas brought hundreds of heads of cattle to New Orleans. The rapidly growing population in New Orleans was the new marketplace for livestock and farmed goods grown and raised in Texas. As these goods made their way from unclaimed territory to Creole and former French lands, the herdsmen working these settings on horseback were mostly African American and Hispanic-Mexican descent. A century or two earlier, these horses and cattle made their ways into the interior of the continents from the new farms established by settlers of New Spain, and the numerous ships sunk unexpectedly just off the shores. As cows made their way to solid ground during this time, they established themselves as a part of the local ecology. Many generations later, the long-horned cattle that defined the Spanish Cattle population of Mexico were common to the region.

Cowboy.com
Raised in the wild, these cattle lived more actively than the domestic raised Angus or brown New Jersey breeds back east. As a result, the Spanish Cow developed a reputation for its beef, and became an important addition to a rapidly growing marketplace along the Gulf Coast.
In 1851, the following article published about the cattle in Texas depicts the general attitude members of the industry had towards Texas cattle.

To farmers in other parts of the country the Texan cattle were fierce, mean, and brutal to the competition. It was the habit of these cattle to make their way onto the prairielands of their competitors, freely grazing for a week or two and then leaving the area for the rest of the season.
Their presence on grazing lands resulted in more in just short grass blades, unknowingly these cattle also left behind flies, ticks and numerous other forms of vermin and “animalcules” aside from their waste, dander, unearthed roots, hide and hair. It was the ticks that had the greatest impact on the local ecology for such places. It was the ticks that enabled Texas cattle to ultimately reduce or eliminate their competitition. The main question this led many to ask was
‘what exactly did these Texas Cattle do to the environment to make it so deadly to local herds?’
This question premained unanswered by local farmers for the next several decades of the Texan Cattle industry.

It wasn’t the competition that Eastern Cattle raisers were worried about. It was the aggressiveness of the cattle and the deadly effects of their miasma or effluvium on local cattle. This argument between Texan Cattle raisers and east coast cattle raisers only had the effect of making it less likely for the underlying truths about of these zoonotic epidemics to result in any progress. To Texans their cattle were safe, and since they were constantly travelling and not staying in any one place for too long, they were not considered a threat to health as much as eastern cattle residing on the same land for long periods of time.
.
It would take another several years for public health workers to monitor the progress of Texas Fever, and ultimately see the proof needed to suggest that these animals and their rancheros were unhealthy to the overall country’s economy. To Missourians, Ohioans, Kentuckians, and numerous other east coast cattle raisers, Texans were the next risk of east coast health and financial stability. Meanwhile, it was up to local sheriffs and political leaders to make the first moves needed to secure their hometown region. The fact that Texas Fever infected local animals, not people, only paused the first political actions that would be ultimately taken. One of the most important observations made during this time about Texas Fever, was that it pretty much hugged the long trails crossing an otherwise wilderness range and field setting. Anyone residing just a short distance from these routes never suffered the demise of Texan cattle fever, unless these Texas Cattle made it onto their grazing lands.

In the initial years, trails brought the Cattle into the heart of this country. A number of well-known trails were established over the years that led from Texas to the center of the United States. The most commonly travelled routes during the very first years of this industry were the trails to Sedalia and Abilene. The first provided the east coast populations with Texan meat, the second served large towns in the Midwest.
Between 1850 and 1861, a number of railways were built enabling westernmost towns to interact more with east coast cities. It wasn’t until after the Civil War however that these railways became the major routes for people to take. The effects of the improvements in technology and industry related to the railways ultimately led to the first rapid spread of Texas Fever from Texas to Ohio and Texas to New York in just a few weeks. The combination of horse and cattle migration, and the availability of both commercial train and commercial shipping lines turned a once very regional business into a national industry, along with whatever disease patterns accompanied its products. Between 1866 and 1870, this turned Texas Fever in a nationwide epidemic that threatened the entire United States cattle industry, and along with that one of the primary sources of foods for this entire country.
Whereas it took nature decades to centuries to turn the Mexican born tick related diseases of cattle into a small regional endemic problem, it took the development of the various new forms of transportation and the establishment of east coast livestock trade and slaughterhouse industries to make Texas Fever a threat to the United States.
The manner in which Texas Fever was spread made little use of the environment itself, focusing mostly on just the cattle. Warm climates helped, but were not necessary during the summer months of these outdoor activities. The warmth of the southern states enabled the major carrier of this disease, the tick, to survive the winter. Further north, extremely cold climates became a limiting factor for the conversion of this disease into an endemic problem.
The primary effect of this disease upon cattle was the damage of the gall bladder. This very specific organ effect was lacking from Texas Murrain. The fever was there, and many of the other symptoms were so generic in nature that to many they seemed to mimic the murrain of the past, but the bloodiness of some of the original murrain epidemics was lacking in cattle influenced by Texas Fever. Following the Civil War, the autopsies of the victims of Texas Fever revealed that their spleen demosntrate the most important patterns of deterioration, not the gall bladder. This told many physicians that the Texas or Splenic Fever was its own entity, unique from previous bovine epidemic patterns infecting the Carolinas and Kentucky region.

Complicating the understanding of Texas Fever’s origins and sources was the manner in which Murrain made its way to Kentucky by the late 1830s. This resulted in the publication of a number of articles detailing the murrain as a continuation of the European version of this condition, and soonafter considered to be the reason and source for Texas Fever. However, there was a large disconnect between the mid-Atlantic region with Kentucky and the Carolinas and the Texas origins of the other cattle fever. In the years prior to the Civil War this probably delayed any understanding of Texas Fever even further, as livestock farms tried to prevent any chances for diseases erupting further west due to westward migrating cattle, not the northward migrations from Texas. Were it not for the gap that developed between the time when Kentucky Murrain was a problem and the period when Texas Cattle Fever first struck, there may have been even more of a delay in the development of a geographical understanding of Texas Fever. The Civil War gave these early veterinarian epidemiologists the chance to take a breather during the war, in order to regroup their thoughts and come up with a better way to research this kind of public health problem.
Time and nature led the way to introducing this disease to the United States during the 1850s. Texas became a part of the United States in December 1845. Before this time, cattle and other livestock animals from Mexico survived in those parts of the western edge of the Great Plains for centuries. Families of Mexican descent managed to occupy those lands between Mexico proper as far north as Colorado and even Wyoming. Any breeds of cattle adapted to Mexico managed to make their way northward along with the most traditional of these families, who today consider themselves neither Mexican nor United States in descendency.
This fusion of wild cattle of the Tex-Mex area with the domestic, more acculturated way of being of communities just east of this Far west environment had an impact upon the farmsteads established in States like Oklahoma and Missouri, northern territories lacking any familiarity and history of adjustments made to the consequences of a more southern way of life. In particular it was the ecology of the then southwestern territory that ultimately led to the production of new diseases in the more northern states and territories of the midwest as these herds made their way into territories virgin to the diseases bred in hotter climate settings and livestock ranges.
Quarantining. If we view this disease pattern like the inhabitants in Missiouri did, we might conclude that in 1852 this disease made its way into Missouri due to the cattle migration from Texan-Mexican territory. Once these cattle made their way into the southwestern corner of the state they introduced some sort of contagion or “poison” to the state. In every case, the cattle only stayed there for a short while, about 3 to 5 weeks, and then left to continue their journey. One or two weeks later, the local cattle became lazy and then ill and within just a few days died.
Locals had no other way to interpret these events than to consider the deaths a result of either some form of miasma bred and released as effluvium from the Texas breeds, or as some unique form of contagion eminated from their bodies. Many blamed these events on the warmer climate settings. But sunshine was also to blame, with the argument that this light made for a fatigued, much lazier herd.
In a very short time, this perception of the healthiness and infectiousness of Texas cattle led to the development of an animal quarantine policy. This need for quarantine was at first defined and promoted only by local farmers and breeders, and caused a debate between Texan cattlemen and the locals. But soon, the evidence spurred on the support of local leaders and government officials, leading to the passage of local and state laws on this matter. From this point on, Texas cattle and cattlemen were no longer welcome to Missouri. Any serious attention paid to market Texas meat to local restaurants and merchants required a complete inspection of any and all sources for that meat, ranging from the remains of the carcasses left behind at slaughterhouses to the inspection of cattle about to be slaughtered. By 1857, Texas Cattle were famous for their temperament and aggression and even when slaughtered were still considered very healthy due to the putridityof their flesh. This did little to appease ranchers who lost thousands of cattle in just a few weeks in Missouri.
Source: The Revised Statutes of the State of Missouri. pp. 1104-5. 1856.
Transportation and Disease. As was the case for many diseases introduced to the country during the 19th century, this 1853 epidemic of cattle fever in Missouri was only a hint of what was about to happen. Laws did little to prevent the Texas cattlemen from bringing their products to the eastern marketplace. A fairly effective transportation route was established by 1860, enabling the investors in this industry to use numerous ways to bring Texas cattle into the Eastern states.

Improvements made in transportation included the development of new methods to bring cattle back east. It also allowed for the invention of flatbottom ships rigged specifically for the transportation of cattle from one side of a large river to the other, and even from one port of departure to numerous receiving ports located dozens of miles away. This latter invention was the product of a Military Surgeon, who was more a cattle doctor than a soldier’s surgeon. His invention turned the cattle business into an overnight success during the late war of the Union and Rebellion years. The full impact of this invention would ultimately be the spread of a western murrain illness into the eastern states, resulting in the deaths of large numbers of eastern breeds, from both the Ocean ports sites westward, and the eastern Great Plains raillines eastward.
Once again, Texas fever was making its way into the heart of the heavily settled eastern United States. Once the war was over, these practices continued and as the businesses and marketplaces recovered, the transportation of cattle into the interior and over to the east coast became a standard industry for western settlers. The notion of the “cowboy”, a term first applied to cattle raisers in New York nearly one and a half centuries earlier, was now a commonplace name and occupational title for anyone willing to engage in this occupation.
Wagon Roads, 1860
As a result, along with the cowboy came herds of beef-producing Texan Cattle, and with these cattle came the Texas Fever once limited to just the midwest. Medicine as well had changed its interpretations of disease by the end of the Civil War. More details underlying the science of medical topography and climatology were now known and understood. By the closure of the Civil War, the notion of what caused diseases like the fever had changed from a simplistic interpretation of contagion, to claims that natural sources for miasma and human sources for effluvium could be the cause, ranging from animalcules native to the local setting to the various theories on how toxins and other natural pathogens were produced. The notion that poor sanitation was just as much a cause for disease as local winds, water ways, soil types, landforms, mineral types and chemistry defined how to interpret the most important physiographic feature of a region, and how these related to the human diseases common to these settings.
Early Spatial Theories.
Nineteenth century medical geography depended heavily on the role of latitude in disease theory. Epidemic disease patterns were born in the tropics, and became epidemics when they made their way into the temperate and frigid zones. Endemic diseases existed naturally within a given region, regardless of latitude, weather, windflow patterns, and animal and human migration behaviors. With epidemic diseases, the people resided in a given area where the disease was introduced through a migration or diffusion process. For endemic diseases, the cause for the disease was always there, and only when humans migrated into this region did disease problems commence.
For zoonotic diseases, those illnesses experienced and propagated by animals, local causes existed in enzootic and epizootic forms. Enzootic diseases were natural to the region and were transmitted locally by natural weather, wind and water flow, with their routes defined by local topography. Epizootic disease were foreign or imported and were carried into a region by way of natural events linked to weather, wind, water flow, and at times human migration behaviors. Natural disasters assisted in some of these processes, in the form of such things as storms, heavy winds, meteoric events, volcanic effluence.
One of the first observations made of these Spanish herds was that southern cattle always infected the northern species and not vice versa. This observation was directly linked to three popular observation-based geographical theories for disease. More than fifty years earlier, the latitude theory for disease became popular. The fact that Texas Fever and Texas livestock could migrate northward and infect new territories, but the reverse not true for the migration of northern beef suggested that latitude did play a very important role in the diaease behavior being observed. For most of the nineteenth century, medical topographers also believed that epidemic diseases like Texas Fever were bred in the Torrid or Tropical Zones of the earth, whereas most endemic diseases were bred locally. The fact that Texas Fever appeared to behave very different from the other forms of murrain provided additional support for the possibility that Texas Fever was very different from the Bloody Murrain that cattle back east were experiencing.
Another spatial concept related to Texas Fever geography made use of isotherms to define the nature of the disease and its behavioral patterns. Isotherms did not always match latitude, enabling some flexibility when it came to defining the northern most edge of these places this diseases tended to remain persistent in. With this theory, tropical requirements were still an important requirement for the epidemic, but it also allowed for similar patterns to occur in places were tropical-like temperature and weather patterns existed. The warm, humid portions of the Great Plains, regions where severe thunderstorms and heavy wind patterns prevailed, were also locations for the Texas Fever to erupt.
Finally, Texas fever demonstrated the proximity to people and livestock that normally was associated with contagion as a possible cause. Observors of the cattle trails leading from Texas to Kansas and Missouri had this disease prevalent only within a short distance of the route taken. Even though regions more than hundred of meters away appeared to be identical in geology, water geography, ecology and plant and animal presence, these regions did not have the ability to propagate Texas Fever. This was perhaps the most important observation of the behavior of this disease that was not only accurate, but also important for the future of disease prevention techniques developed in realtion to cattle drive laws and the establishment of animal quarantine policies.
These three spatial observations meant that fortunately, if you resided far enough north to exclude Texas Fever as a possible endemic disease, that you also might have the ability to prevent its return to the local settings. If accurate and continuous observations concerning temperate, precipitation and humidity were taken, this meant that climate and temperatures could be used to tell you when to expect this disease to return by making its way across the southernmost state border. This was how the first quarantine measures were taken to prevent Texas Fever eruptions in Missouri, Illinois, Ohio.
Other methods applied to trying to understand disease patterns during the third quarter of the 19th century include detailed analyses of local topography, soil features and hydrology. Perhaps one of the most important observations observed time and time again regarding disease focused on the role of calcareous rocks on epidemic and endemic disease distribituion. In Texas, a similar interpretation was made of Texas geology.
The notion that diseases born from tropical zones tended to be very deadly was supported by the observations made about how Texas Fever impacted the Missouri cattle. The fact that any transfer in the opposing direction did not occur suggest that disease transmission across the globe was more likely to occur in one direction versus another. This ideology was adhered to for generations between 1790 and 1860. The behavior of Cattle Fever only further promoted the belief that such as theory was very much correct and in line with the e xpectations. This meant that the disease theory based on zonal patterns could be used to predict livestock and human disease patterns and behaviors.
The other claim about disease geography further supported by this behavior of cattle fever was also a product of the latitude theory for diseases, in particular the behaviors of yellow fever and numerous other fever types. Several types of fever were by then behaving according to their expectation as defined by the medical geographers. The Malaria was bred in the south within the tropics, and able to make its way northward only when tropical climate patterns tstruct the temperate zones. Disease like Typhus and Yellow Fever also managed to abide by these rules. With Cattle Fever prevailing in much the same way, only inland along heavily travelled migration routes, geographers had confirmation that a significant portion of their theories were correct, excluding the part that made it appear as though an inland migration in this case tended to prevail more than the ocean side shipping routes that appears mostly responsible for the spread of malaria and yellow fever.
1884 Quarantine Line relative to 1861 Railroad Tracks
..
The Cattle Trail to Sedalia, which led to St. Louis, in relation to the 1884 Quarantine Line
After nearly a century of tradition, one couldn’t help associating diseases with the latitude of the earth’s surface. The climates associated with latitudes and the impact the rays of the sun were felt to have on local disease patterns were the primary reasons the equatorial region was considered the unhealthiest region of the world to live. In spite of the development of the germ theory for disease during the 1870s, topography and climate often ruled in the philosophy for many disease patterns well into the 1890s. Climate, latitude and sunlight prevailed in the arguments for these claims.
Diseases of the tropical and subtropical regions of the earth were least impacted by the bacterial theory. This is clearly illustrated by the unchanging philosophy assocaited with Texas Fever–an illness suffered by cattle and certain other forms of livestock found to be primarily related to the latitude of their place along the large routes established to bring thousand of heads of beef to the highly demanding marketplace.
.
One way of breaking down the expanding United States into regions defined by Sequent Occupancy Stages. This method is based on local population density, physical geography, economic and transportation features.
An Explanation based upon Sequent Occupancy as a Spatial, non-Temporal Feature
Another way to interpret the above events is to apply sequent occupancy as a means for defining general land use features relative to the place under review and its relationship with other places. The traditional sequent occupancy interpretation of land use defines regions with minimal develop, mostly wilderness-like or ecological in nature, as opposed to the more highly evolved, urbanized settings developed due to habitation. Between these two ends of the time line depicting technological, cultural events are two or more other periods or stages of development. Following the wilderness setting is a pioneer setting where people reside in homesteads and are self-sustaining. This in turn is followed by a stage dominated by small business settings, with many of these businesses established in natural products industries, the production of farming or livestock good produced for the local communities, and the production of some secondary forms of merchandise involving more technological prowess, such as the incoroporation of small lumber, fabric, and paper industries into the production of boards and planks, furniture, clothing items, and stationary goods.
Early to Late Sequent Occupancy in 19th Century Images: Stage 1-Wilderness ** Stage 2-Pioneer ** Stage 3-Early Farming and Industry ** Stage 4-Technology and Industry
The reasons for this way of interpreting a setting are several in terms of medical geography. The first is this interpretation demonstrates how these different stages of development relate to disease patterns. The crowding of living settings, the closer livings associations between wildlife, livestock and people, the modifications in the natural environment along with the conversion of hamlets into villages, followed by villages into townsand the related human and livestock sanitation problems, all of these lead the way to the development of new diseases patterns. Whereas in the pioneer settings, highly infectious diseases like small pox and measles were occasional visitors, dependent on the frequency of travellers making their way through a wilderness or pioneer setting, once the pioneer setting became a hamlet of small village, the likelihood of introduction of a new strain of these and other infectious diseases ensues, and with the crowding of certain buildings settings now the norms (like schools, hotels, restaurants and bars), the likelihood of rapid disease transmission increases, the likelihood that a new epidemic might ensue.

As spatial integration ensues, infectious and living environment diseases become more likely to diffuse across space. An isolated encampment or pioneer cabin disease like measles, during Stage I in the above figure, diffuse more rapidly as village and town development processes taken place followed by industrialization and highly integrated urbanization related features.
Relating this to the establishment of farming and livestock industries, activities more prevalent in Stage 2 Pioneer and Stage 3- Early Industrial settings include animal-born diseases patterns and the likelihood for diseases dependent on sustainable human population density features, such as diphtheria, mumps, certain forms of dysentery, typhus, typhoid, yellow fever and asiatic cholera. This setting makes for the development of rapidly spread influenza epidemics, household scarlet fever cases, and occupancy-linked animal born living animal or carcass-related disease patterns infecting large numbers of people for the first time.
Travel Patterns over Generations. A record of increasing travel over four male generations of the same family, from Great-grandfather (A, 40 km), to Grandfather (B, 400 km), to Father (C, 4000 km), to Son (D. 40,000 km). Each map displays how an individual’s ‘life-time tracks’ increases by a factor of 10 from the previous generation. These diffusion rates related as well to contemporary disease patterns residing within their natural ecological settings in traditional (Stage 1, environmental), developing (Stage 2), developed (Stage 3, early industrial) and highly-developed (Stage 4, contemporary technologically developed) living settings. [CASA Centre for Advanced Spatial Analysis, UCL, urbanTick blogsite, Fabian Neuhaus, urbanTick, CASA, UCL, Gower Street, London, WC1E 7HB. WARNING: This site is unfortunately unstable and linked to crashes; accessing it is NOT recommended.]
Applying Gordon Pyle’s method for applying a given disease pattern to a modeling tool, the following regional descriptions could be assigned to the above map depicting regionalism in relation to Sequent Occupancy.
Diffusion behaviors relative to place and economic development, based on primary transportation methods. Notice as well the possibility that the Quarantine line also depicts the boundary between endemic and epidemic regions.
Whereas Pyle’s modeling defined the changes that take place in an epidemic over time, implying the economic progress for a study region is what defined the diffusion patterns, the above model defines how the type of diffusion process may change over place. A disease migration may commence as a simple diffusion process by mimicking the airborn miasma or effluvium process including a dependence on climatic and topographic features. Over space and time we see this same disease evolve into one that has a migratory pattern less dependent on topographic and climatic features and more dependent on human ecological features. This disease erupts in places with a particular victim type and susceptibility, the spatial distribution of which is dependent on a combination of transportation features, socioeconomic population patterns, and village-town-urban status in relation to its overall economic status.
In this model, the more effective the human transportation methods become, the more predictable the disease pattern is. Assuming it follows a standard hierarchical diffusion process, impacting those regions considered most susceptible to infection first, this suggests that some sort of prediction modeling is possible. We cannot predict who will be the next victim of a disease, but we can predict where, how and even why. Cars, buses, trains and ships become the defining means of travel, making roadways, rails and waterways important linear features relating to the disease pattern, in turn suggesting an order in which the eruptions of new disease-ridden areas might happen. This is the exact method for mapping disease that applies to the logic behind the diffusion process for the spread of Texas Fever throughout the United States. Texas Fever began as a Type I disease, changed to a Type II diffusion pattern once the first heavily populations townships were reached, but very quickly became a Type III diffusion pattern as it made its way into the heavily settled regions of the east coast states.
An estimate of Pyle’s Staging of Diseases relative to Sequent Occupance, over space rather than time. Applying this to the previous map, Region I is a regular diffusion process, Region III a hierarchical diffusion process, and Region II an example of Pyle’s Mixed Diffusion Model.
.
.
In the above Regions map, Region I is defined mostly by a lack of developed wagon roads in 1860 (and is even more primitive during the first migration in 1852/3). Region II is defined by the presence of frequently travelled wagon roads, with minimal roles played by railway transportation. Region III is a result of well intergrated wagon roads and railways. Taking this logic one step further, without well defined roadways in Region I, diffusion also presents itself either as a linear procesvery dependent upon human migration patterns, or as a non-linear process, even when human and human-domestic animal contact are required. The utilization of major transportation routes by wagons infers more likelihood for diffusion along these routes, rather than transverse or lateral migrations away from the route in multiple directions. The utilization primarily of railways to move the disease about infers a very rapid transportation and transmission process, with more likelihood for success at the end of that route assuming it neds in the interior of some highly developed urban, economic center.
This model just described allows for the development of predictive modeling methods for transportion-based disease migration patterns. With a review of past epidemic migration patterns, it enables researchers to uncover certain repeated behaviors depicted by past disease patterns. Some of the first disease geography maps produced as annual reviews in part assist researchers in this process of better understanding ecologically based disease migration patterns. On another page at this site, the ten year span of behaviors in the nidus area for cholera presents us with this kind of helpful spatial disease input.

Radcliffe’s Timed Series, also reviewed at this site.
This suggests that it may be possible to predict disease diffusion behaviors based upon how we define the roles played by each of these contributors. It is possible that simpler environmental-ecological and human ecological models can be very predictable due to their definitive routes of travel, unlike the Type I (Region I) diffusion process in which a 360 degree direction for flow is possible.
In the case of vectored diseases involving insecta and other macroscopic animalcules, the ecology of the organism as well as its carriers, hosts and vectors play important roles in determining how to map the disease based on its history. For diseases caused by microscopic organisms, the local ecological role plays a different role, especially if that organism is more important as a pathogen than as a part of the food web. For diseases bred by very small microorganisms, depending upon life cycle behaviors, the likelihood for perpetuation of this pathogen is dependent primarily upon the lifespan and behaviors of its potential hosts. Unlike vibrio, a microorganism that can exist ecologically in specific environments defined by weather, hydrology, geology, water chemistry, and plant and animal ecology, the mesofocus for Texas Fever is very much determined by the movement of its carrier–the cattle–and secondarily by humans should any human-related diseases erupt due to similar carrier activities.
.
.
PRESENTATION/RESEARCH NOTES: Applications of the above to Disease Modeling
By GISing the past we develop a better understanding of the problems related to bioterrorism and the threat to food supplies for the future. Both of these national threats are farm related. To protect the natural resources related to crops and livestock, surveillance is required. In turn, to effectively monitor these important natural resources, we require a database that documents normal and irregular patterns and activities related to these industries.
Researching the past endemic and epidemic zoonotic and phytologic disease patterns provides us with unique insights into how the geography of farm disease patterns and zoonotic problems of the past related to the more complex examples of the same that could exist today. Past epidemics and epizootic disease events are important subjects in need of effective medical geography tools. This is currently one of the primary responsibilities for future medical geographers.
It was during the time that the knowledge of the microorganism, in particular the bacteria and virus, became more focused on the organism and patient, not the environment, that much of our experience in environmental epidemiological surveying was greatly reduced and some of these skills almost lost. The medical geographers of the past however did not have these prejudices getting in the way of their discovery process. Without even knowing the role of the microorganism in certain disease patterns, the medical geographers of the past were able to successfully document the spatial behaviors of many diseases. It is up to today’s medical geographers to relearn these skills. In some ways, the medical geographers opf the past were far more efficient and better at mapping disease that many of the medical geographers of today. This is due to the biasness introduced by the non-geographer’s interpretation of disease that most of medical geography exhibits today. In producing their records of disease patterns, the medical geographers of the past were unhindered by the sudden change in focus and changes in concentration that ensued due to the focus on the bacterial origins of disease.
Whereas the microbiologist in an expert within the lab room, the medical geographer is an expert whenever and where ever weather, geology, vegetation zones, poverty, and place play a role in the overall personal and population health status. With certain diseases, such as the animal-born Texas Fever, a disease that goes unmonitored can spread effectively for more than 750 miles, such as from Mexico to New York in just a season or two. Texas Fever accomplished this diffusion over just af ew months period back in 1845. The association of the hundred to thousands of livestock deaths such activities caused was nearly impossible, were it not for a geographical interpretation of this disease’s natural history.
Geography and the environment played as much a role in the study of this disease as the testtube when it came to understanding the metabolism and microecology of the disease causing organisms responsible for Texas Fever. One specialty cannot survive without the skills and knowledge base of the other.
When we look at natural disaster and large scale epidemiological/epizootical history, we find that nature has a way of duplicating the events of the past. At times these duplications appear to be similar events, recurrences in history, which in actuality are due to different causes. By reviewing the work of medical geographers of the past, merging their evidence and any new takes on this history with the more contemporary work on agricultural disease patterns, we can perhaps get a more accurate, broader picture of the current state, and the background knowledge needed to make better use of what is out there as a part of such a surveillance project. This Texas Fever study is an example of such a study.
In a recent conference on bioterrorism it was acknowledged that the threats to our agricultural and livestock industries constitute a silent threat that never gets much attention from press. The origins of these concerns were far from being Humboldtian and Malthusian in nature. Overpopulation of the earth is not so much a concern as the concern for a potential re-emergence of diseases normally considered to be limited to specific regions of the earth. Most of the time, when the potential for epidemic-related deaths of mass proportion become a part of a conversation, the early 20th century Asiatic flu epidemic is mentioned. When food-relatedcrops and animals are posed as international threats, some of us might recall the lessons taught to us by such zoonotic and phytotic diseases as anthrax and the potato blight. But many of these past epidemics have also taught us that there are specific times and places where certain diseases can erupt. These places can be defined using GIS.
The possible impact that an unexpected in-migration of disease has on the United States has never fully been analyzed. Unlike people’s disease, animal disease has the ability to make its way into the heart of our country by way of any of numerous animal migration routes. Aside from compass direction based, these migratory routes include the possibility of land and water routes, by way of saddlebacking migratory animals, or any of a number of commercial methods for migration out there alongside the national borders. These routes may be taken by large mammals such as elk or deer, or travelled inconspicuously by much smaller carriers like badgers and woodchucks or even reptiles, birds and rodents.
Thus the questions:
- Can GIS effectively be used to uncover, predict or circumvent any unexpected in-migrations of foreign born diseases?
- Is quarantining an event that can possibly be managed in such a way at the large regional and national level so as to prevent the introduction of new diseases to this country?
- Are there any diseases that have a likelihood of making their way into this country?
- How might a disease behave spatially were we to find that a disease just made its way into this country, either by human transportation means involving animals and crops, or by way of natural migration and dispersal routes?
Knowledge of the behavior of past disease patterns, especially around the turn of the 19th to 20th century, provides us with ways to conceptualize these events should they in fact take place. The late 19th century geographers’ old Sequent Occupance tool has it applications to modern disease diffusion epidemical processes. The same can be said for Pyle’s diffusion behavior models. Each of these needs to be expanded to understand the variations in applicability each of these tools in fact have. As the Texas Fever migration demonstrates with regard to applying both of these tools to this disease migration pattern, we find that a hybridization of these two methods of spatial review, to which is then added the spatial version of interpreting Pyle’s originally temporal tool, in order to understand the regional differences in diffusion patterns that might exist between developed and undeveloped regions, normal or high income urban community settings versus low income, socioeconomically disadvantaged potential disease migration settings.
This particular study of historical epidemic behavior of zoonotic diseases has numerous applications to modern disease mapping and the prediction modeling of diffusion patterns. GIS provides us with the mechanism to employ this method of mapping disease behaviors. Spatial Analyst tools allow for diffusion related behaviors to be defined with GIS. Network Analyst tools enable diffusion pathways to be defined. We can add to these two maps a vector analysis method focused on places where epidemics prevail or re-emerge, assigning specific topographical, meteorologic, aspect and land surface featiures to the model, assigning a priority or weighted value for this information based on Pyle’s Disease model type noted to best fit the pattern at hand.
Since the Texas Fever is a tick-born disease, the effects of wind upon the diffusion process are relatively minimal, compared with true airborn diseases such as those carried by insecta, pollen or spores, and other light objects dispersible by wind. Even with in the most rural parts of the disease zones noted, events born in very rural areas have a dependency upon the overland trail routes. The primary diffusion process is limited in distance from the trail, based on the lifespan of the vector or carrier and the time needed for this insect to mature and lay the eggs needed to further propagate the epidemic. As noted by numerous authors in the historical writings, the diffusion of Texas Fever along the trails was limited in its ability to spread too far away from a trail. In rural regions where there are very few trails and long distances between trails, this meant that the methods by which a hierarchical process could occur were pretty much absent from this setting.
In contrast, once the second zone is impacted, major transportation methods change and the speed of the diffusion process relative to distance traversed increases considerably. The closer to the urban core the disease spreads, the more likely it become to find a new host and victim, with more options for routes to be taken locally. By the time it reaches the urban core, it’s diffusion process spatially stabilizes and the disease begins its stage of re-emergence based on time, climate, population density, and the host-vector-microbe’s need for ecological support. Given the right settings, the disease converts from being epidemic and periodic to occasional in nature or even endemic and recurring.
Relating this to the diffusion of Texas Fever across the United States, we find that the disease began as a Type I disease when it was a part of the natural history of the setting in and around the Texas-Mexico border. The exact method of penetration into Texas is uncertain, and some evidence suggests it may have been present as a normal part of the longhorn disease ecology, due to the residences of regions that later made up New Mexico, Arizona, Colorado and Wyoming, regions settled, occupied and developed in some places by families with more than 250 years (some told me 400 years) of North American heritage. Upon initial diffusion into the United States and its immediately adjacent territories, the disease behaved according to the natural ecological features. Since they depended primarily upon human livestock, progression of the disease into a mixed modle pattern of migration ensued. Once the herds of livestock were directed northward toward Missouri, the disease naturally followed.
In contrast with the natural ecological diffusion methods, New Orleans commercial activities enabled the Texas fever to very rapidly make its way into a range more befitting of Pyle Mixed Model diffusion area [Region II behavior]. The cattle were transferred by human transportation means, by ships traversing the local waterways more rapidly than of by land routes. This same mechanism foir diffusion would later result in east coastward migrations of the disease as well. With the development of railroad train industry, overland routes were also more rapidly crossed, reducing the impact of the longevity of the host-carrier and tick lifespan on the progress of this disease across larger areas.
.
Contemporary Applications
Differentiating the two different forms of murrain–the bloody murrain of the eastern states, from what was first considered to be another version of the same livestock disease only initated in the midwest, west of Tennessee, is a classic example of the role disease mapping plays in diferentiating or identifying two diseases of similar clinical behavior and appearance. An earlier project I engaged in which involved much the same research question and methodology involved the history of cholera on the Oregon Trail. The problem was that historical writers were of the imrpession that cholera existed in certain parts of the U.S. at specific times in U.S. history. The problems were that 1) cholera had a very limited period of presence in the U.S. and could not be present during many of the years it was claimed to exist, and 2) the term ‘cholera’ applied to two or more diseases, which due to the nature with which diseases were defined in the middle-1800s, made it very unlikely the two different forms of disease, with distinctly different clinical presentations and mortality rates, were both due to the same “cholera” that is referred to today.
Natural topographic, climatic and ecological features, along with human population patterns, supported the notion that the Asiatic cholera was very limited in how far it could spread to the western part of North America. In contrast, a model could developed defining regions at risk for this cholera, versus at trisk for less fatal diseases representing cholera but less fatal. This resulted in the following topical map demonstrate the regional differences between Asiatic cholera and various forms of dysentery thought to prevail along the trail.
The Sequent Occupancy model provided further support for this theory. The section of the U.S. appearing in the following map covers areas that may be classified as Type I and Type II, and perhaps even fully evolved Type III regions. Since Asiatic cholera is dependent upon regions that contain a significant amount of human population density, much of the region on this map is ruled out from having true Asiatic cholera, aside from the fairly urban jump off sites near Missouri and the parts of the trail immediately after this point of departure, and the western coastal towns of significant population density.
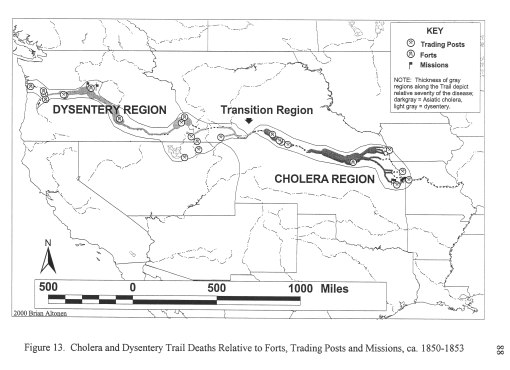
Figure from my thesis (which see)
.
.
.
. . . . across rapidly travelled waterways.
Natural Ecology
Bringing the Texas Fever into perspective with other disease philosophies for the time, we can overlay the above line-boundary-area features for the disease and its relationship to other common disease theory maps already dominating this field of medicine for the time. The most important of these maps to relate to Texas Fever is Alexander Johnston’s 1856-1861 map of medical geography produced prior to his Natural History map book (ca 1956/7), displayed to the Royal Academy of medicine but not published, followed by its next rendering included in a later edition of this book.
Note: The word “Intermittent” in caps is located above the northern boundary of the tropical or torrid zone, which follows the southern edge of Chesapeake Bay, as well as the Types II-III boundary (see next illustration for more).
An initial impression of the above map relative to the regionalism defined by Pyle’s Risk Type method demonstrates that many of these disease patterns tend to have a latitude relationship, which also involved weather and proximity to large water bodies. The Type III hierarchical regions are those involving the megalopolis between Massachusetts and Virginai, along with several isolated urban settings along the souther Atlantic and Gulf shores. The hierachical diffusion process noted for the Great Plains Zone III, includes some very rural diseases but especially Goiter. This goiter would have been classified as an endemic disease pattern with local geographical causes, reputed to be environmental at the time but as time would later show were actually human behavior and socioeconomically related. The presence of Small Pox, Measles and Scarlatina along Appalachia is due again to socioeconomics of this poverty stricken region with Wilderness and Pioneer types of survival engaged in by most of the settlers. Also notice the cold temperate zone [New England] behavioral pattern for consumption relative to the remaining diseases.
With regard to fevers, the intermittent fever is the most northern of the fever types, followed by remittent and then yellow fever. Spotted or Dengue fever also fits into the moderate portion of the Temperate Zone, with yellow fever prevailing mostly in the Torrid or Tropical zone. The distribution of yellow fever however is not restricted to tropical settings, for due to the warm summer months, and as previous medical geographers noted several decades before, the warmer climates of urban settings with significant population density made them more susceptible to tropical originating disease patterns like yellow fever. We thus associated diseases like yellow fever as having an endemic region, where the existence of the disease is persistent throughout time, and the epidemic region where given the right conditions this disease re-emerges either as some form of imported contagion or as a sort of miasma or pre-miasmatic substance (phlogiston or septon according to Samuel Mitchell back in 1800). These would enable the warmer urban centers to re-develop the pathogens or substances needed to cause yellow fever to re-emerge.
This image of Johnston’s map is pulled from my page on the section of Alexander Johnston’s map depicting North America. The Key on the original source page lists the diseases noted on this map; several of these have letters used to indicate their small area locations. L2 is a straightned version of the torrid-temperate zone border. L3 is the Frigid Zone border.
Next, if we relate the above logic to Texas Fever, we find it is within the overall Fever Zones of North America defined by Johnston, and that it is very much akin to the yellow fever, only with an ability to difuse further into the interior of the North American continent. The Texas Cattle Roads were very much akin with the riverway ship routes in terms of appearances, movement across the surface of the earth from tropics to temperate, and in turns of the diffusion behaviors that these geographic features resulted in.
A close-up of Johnston’s Yellow Fever Map, with annual isotherms (only approximated) from D. M. Warren’s book A System of Physical Geography . . . (1860) overlaid along with previously described boundary lines and areas. The quarantine line approximates the 60 degrees Average Annual Temperature Isotherm. Based on the location of the word “INTERMITTENT”, the boundary line between Torrid and Temperate Zones is close to the 55 degrees average annual temperature isotherm.
To the medical geographer for some time between the late 1860s and 1880, this meant that a pattern was being observed that had resemblances to other disease migration patterns. This realization most likely is what led to the intense research of texas fever that ensued and the establishment of the U.S. Department of Agriculture these observations and concerns ultimately resulted in. An experienced observor of the disease at the midpoint in this period of time would have noted the diffusion of disease increasing as it made its way further north, into the more heavily populated regions. It wasn’t influencing people so much as it was influencing animals–the most important feature related to peoples’ foodways and more importantly the economic success and failure regarding any investments made in the rural and suburban livestock industries.
This overlay suggests a similar latitude-related relationship between yellow fever and Texas fever, with the exception of a small mid-Atlantic region on the east coast.
END
The Pavlovski-Voronov Model
From 1937 to 1950, Russian Geographers Pavlovski (shown above) and Voronov defined disease spatial behavior in a unique ecological way. This is covered on another page.
 .
.
.
.
Human Ecology
The two counties in Arkansas displayed, Benton and Washington, are in the upper left corner of the state map. Incidentally, these were also considered the two healthiest counties in the state in 2011 (see http://www.fox16.com/news/local/story/County-health-rankings/W4IWqX9Uvk22xUlUsM9skQ.cspx, accessed 3-20-2012).
.
.
.
.
.

.
..
.
.
.
.
REFERENCES
.
.
.
Map Sources

.
Transportation by railroad
.
.
.
- Rabies Epizootic Area
- Coyote and Gray Fox rabies epizootic area. [ JPG ]
- Plague
- Geographic Distribution of Plague in Texas. [ JPG ]
- Hantavirus
- Geographic Distribution of Human Hantavirus in Texas. [ JPG ]
.
Other historical references to the murrains

.
.













































Leave a comment