November 2014
Monthly Archive
November 12, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on Can/Should we use maps to monitor socially sensitive issues?

These four maps demonstrate one of the most controversial things about disease mapping. Sickle Cell is a disease strongly linked to Slavery history. It is less correlated with other African or African American cultural features such as Muslim in-migration communities, international African missionary program locations (some ICDs are strongly associated with these due to special humanitarian programs) and contemporary African American cultural behaviors and features.
This begins my discussion of examples of how to apply these maps to contemporary research, using the Mixed Model or combined qualitative-quantitative research approach to evaluating population health.
The two cultures most in need of this Mixed approach right now are the Hispanic/Latino and African American/black/negro groups.
There is a very important argument that population health monitoring leads many of the critics to. When, if at all, does this procedure violate HIPAA?
How does grid modeling actually correct for this problem through a change in spacial parameters and region or place definitions?
Traditional GIS using standard base maps enables zip codes, towns and census and voting blocks to be linked to the data–this link is expressed in the data used to produce the map.
When grid mapping is used (like my NPHG method), you eliminate that ability to link a diagnosis to a particular site as we know it. To know a particular case is from a particular town or hamlet, you have to know as well that the areas next door are lacking these cases. No healthcare professional or expert in a disease knows with absolute certainty where every case resides in a region, not matter how much he/she thinks the program knows, since it is the "expert" in the field.
In other words, the likelihood for a "mile away" example, that people often forget, is always there.
The two maps on the left depict a special formula I used to evaluate Sickle Cell carrier identification. (The IP process converts the numbers to relational concepts, a method more useful today when analyzing certain disease patterns and mimics the prevalence methods always in use). When IP maps and numbers maps are close together, the result is a very strong spatial association in terms of magnitude.
The maps on the right depict where the African Americans were residing during the slavery period in U.S. history, and how African American households are distributed today.
There is a mid-Atlantic density for carrier traits situated along the densest population density region in the U.S.. This is either due to population density itself or the primary in-migration routes for slaves early in U.S. history. Virginia, the heart of slave trade and in-migration early on in U.S. history, remains the center of the carriers for this genetic trait.
The isolated high peaks along the west coast demonstrate a more recent outcome due to socio-cultural behaviors, situated in fairly small, perhaps even isolated African American communities.
This map brings up two ideas for a qualitative-quantitative research of African American diseases patterns. Are the East coast social aspects or variables similar to the same for the west coast?
If we were to select several small communities on the east coast, and compare each to the single isolated community on the west coast, will latitude (north versus south) differences be detected that are distinct when compared to the west coast patterns?
We know that the southern belt, stretching from Mississippi to Florida, has social, cultural and health and human behavior differences when compared with the Atlantic states. Do statistically significant differences exist between these two regions as well?
For researchers and students – – my mixed methods pages are :
https://brianaltonenmph.com/biostatistics/grounded-theory/combined-qualitative-quantitative-methods/
https://brianaltonenmph.com/biostatistics/grounded-theory/combined-qualitative-quantitative-research-methods/
See on Scoop.it – Medical GIS Guide
November 11, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on 6 Historic Disease Maps of the U.S.

These are historic disease maps of the United States, depicting its natural disease patterns based on the local climate, latitude and topography. These maps were produced by Heinrich Berghaus, 1846, Adolph Muhry, 1856, Alexander Johnston, 1856, William Aitkin, 1872, John C. Peters, 1877, and Robert W. Felkins, 1888.
These six maps represent a period in medicine when the philosophy for disease began with the notion of climate and topography, an easy to imagine offshoot of the traditional "miasma" theory often ascribed to diseases during the antebellum history period (a period of perfecting medical climate and topography mapping ca. 1825, to the advent and final acceptance of the bacterium and bacterial theory ca. 1890.)
I produced extensive reviews of each, the links of which are in the paragraphs or brackets below.
UPPER LEFT: The earliest of these maps is Heinrich Berghaus’s ‘Planiglob zur Übersicht der geographischen Verbreitung der vornehmsten Krankheiten, denen der Mensch auf der ganzen Erde ausgesetzt ist’, (Camerini, 2000, translation – ‘Planisphere toward a survey of the geographical distribution of the principal diseases to which man is exposed over the whole world’. Heinrich Berghaus (http://wp.me/Puh6r-7DG 😉 was a geographer and atlas illustrator rather than a physician. He applied many of the teachings of his important predecessor Friedrich Schnurrer, the first regional disease cartographer (‘Charte Uber die geographische Ausbreitung der Krankheiten’, 1827; at http://wp.me/Puh6r-9dj ), and Dr. Carl Friedrich Canstatt, author of ‘Handbuch der medicinischen Klinik’, and producer of the first comprehensive disease taxonomy focused on climate, weather and the natural elements as causes (http://wp.me/Puh6r-9lB ).
UPPER MIDDLE: Adolph Muhry’s map, [ http://wp.me/Puh6r-1dv ] Muhry’s map is difficult to read and interpret at first. But par for the time, it is hand watercolored in my version , contained in ‘Die Geographischen Verhaltnisse der Krankheiten oder Grundzuge der Noso-geographie ‘ (The Geographical Relations of Diseases, or Outlines of Noso-Geography). Muhry continues along the line of the first most famous medical geographers like Schnurrer and Berghaus. Isolated from Great Britain’s Alexander Keith Johnston to some extent (due to medicopolitical rivalry and egos to some extent), it is interesting to compare the maps of these two.
UPPER RIGHT: In terms of fame, Alexander Keith Johnston (http://wp.me/Puh6r-6kz 😉 stands alongside John Snow (no personal page links) and William Farr (http://wp.me/Puh6r-8B3 😉 when it comes to advancing the field of medical geography in Great Britain. A geographer and cartographer, not a physician, he had a way of polarizing himself at times with others in the medical profession. He produced the most valuable maps on disease published in English for the time (http://wp.me/Puh6r-9w1 ), and managed to improve upon the past belief that latitude was important to disease patterns and behaviors, by related disease patterns to his global isotherm charts (his portrait and presentation to the Epidemiological Society in London are at http://wp.me/Puh6r-979 ).
LOWER LEFT: Aitkin’s map [ http://wp.me/Puh6r-7Th ] is a product of his work on the outbreak of diseases like typhoid due to poor sanitation during the Crimean War (1853-6) (http://wp.me/Puh6r-abh ). Aitkin, along with founder of the modern nursing professional Florence Nightingale, worked to re-gain the .respect of the Royal Armies by improving our understanding of sanitation and disease and implementing new programs that in turn led to the Hygiene and then sanitation movements. Aitkin referred to himself as a hygiologist, and was an expert in hygiene and medicine.
LOWER MIDDLE: John C. Peters Maps [several pages, but begin with http://wp.me/Puh6r-5TG ], are unique in that Peters was one of the last of the highly devoted disease topographers of the late 19th century. Most curious is the fact that Peters began his career in medicine as a mixed-allopath-homeopathic physician, which was a very common profession during the 1830s and 1840s. He published the most progressive journal on homeopathy, but when he noticed the homeopaths beginning to behave anti-allopathy and against upgrades or changes in the philosophy to better meet the time, Peters detached himself from this class of physicians, about 1846, and headed in the direction of medical topography. He produced one of the most comprehensive works on the mapping of disease, especially cholera, in his life time.
LOWER RIGHT: Robert Felkin’s maps [ http://wp.me/Puh6r-87N ] and related book, "On the Geographic Distribution of most Tropical Diseases", [ http://wp.me/Puh6r-82f ] , focused primarily on the most important regionally defined, parasitic or organismal diseases, spread mostly by vector and/or animal host. Felkins unique attributes included his masonic and strong missionary background, and his philosophy towards African races residing in the less-developed regions of the world (early "scientific racist", see http://www.pinterest.com/altonenb/scientific-racism/ ).
DISCUSSION. An important progression to note here is the slow change from regional diseases, mostly defined by symptoms, which are linked mostly to place and climate (Schnurrer) and later climate and topography (Berghaus and Canstatt), to most climate-defined and occasionally regionally or culturally disease zones (Muhry and Johnston), to very specific epidemic patterns and even regionally defined differences in these patterns based upon climate, topography and peoples’ lack of sanitary behavior (Aitkin and Peters).
Felkins work (1889 – http://wp.me/Puh6r-87N and http://wp.me/Puh6r-82f 😉 represents an early example of disease regionalization based upon organism distribution and ecology (worms, flukes, schistosomiasis, fungi, etc.), vectored disease patterns with unidentified causality (malaria, dengue, cholera), and regional foodways diseases (beri beri, scurvy), to name a few. His claim to fame however was his belief in the magnetic force of the earth as a possible cause for inexplicable diseases, a theory developed and promoted by Robert Lawsen, Esq., Deputy Inspector-General of Hospitals (http://wp.me/Puh6r-8a5 ).
For another helpful site on medical cartography history, see the Princeton site: http://libweb5.princeton.edu/visual_materials/maps/websites/thematic-maps/landmark-thematic-atlases/landmark-thematic-atlases.html
RESEARCH NOTES
John Snow’s map is not a world maps, so is not covered here. For more on Snow, the following sites are recommended:
Medical Journal Article.
Howard Brody, Michael Russell Rip, Peter Vinten-Johansen, Nigel Paneth, Stephen Rachman. Map-making and myth-making in Broad Street: the London cholera epidemic, 1854. THE LANCET • Vol 356 • July 1, 2000
http://www.uio.no/studier/emner/matnat/ifi/INF5761/v12/undervisningsmateriale/map_making_myth_making.pdf
Why did he have such an impact?
http://www.theguardian.com/news/datablog/2013/mar/15/john-snow-cholera-map
Edward Tufte’s take.
http://www.edwardtufte.com/bboard/q-and-a-fetch-msg?msg_id=0002Je
UCLA site with one of several versions of his map as jpg.
http://www.ph.ucla.edu/epi/snow/snowmap1_1854_lge.htm
Images (so many people have duplicated his work!)
https://www.google.com/search?q=john+snow+cholera+map+1854&source=lnms&tbm=isch&sa=X&ei=IWNhVNeAMvSOsQTK14LQAQ&ved=0CAgQ_AUoAQ&biw=1248&bih=675
See on Scoop.it – Medical GIS Guide
November 10, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on Steinberg: Ebola ‘quite likely’ will hit Chicago, Cook Co. – Chicago Sun-Times
Richard Preston’s “The Hot Zone: A Terrifying True Story” has sat on my shelf for the past 20 years. And though I haven’t cracked it since reading it last in 1994, I knew exactly what I would find when I opened the book again Friday.
Source: www.suntimes.com
Just an observation . . . .
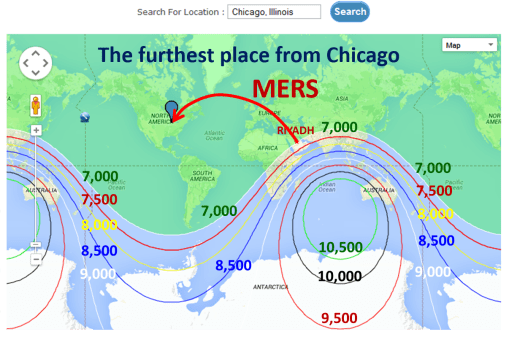
When Middle Eastern Respiratory Syndrome [MERS] made its way into the U.S.in early May 2014 (http://www.cdc.gov/media/releases/2014/p0517-mers.html ), it only traveled about 7000 miles as the bird flies. That doesn’t include any side routes the planes and passengers took.
As the bird flies, the longest route from a foreign country (that is occupied) to Chicago is approximately 10,500 miles, heading from Western Australia to Chicago.
Many of Australia’s little know diseases are those that are animal born. That animal might be livestock in nature, marketed as a pet, or present as a refugee on board. The common Australian diseases to strike the US tend to be like Australian Equine Fever.
When we consider the Ebola distribution, the distance it has to travel is very close to that of MERS. Ebola however is more latitude-defined, its ecology more limiting than the same for MERS.
To better understand disease flow patterns in the Chicago area, I developed some videomaps on common diffusion patterns for a disease. See:
Chicago Disease diffusion patterns — https://www.youtube.com/watch?v=BAmftXNEahE (four ways that diseases theoretically diffuse in and around Chicago)
African Disease patterns around the Great Lakes — http://www.scoop.it/t/an-episurveillance-researchers-guide/p/4027597103/2014/09/07/african-in-migrating-disease-patterns-around-the-great-lakes-region
African Disease Patterns, entire U.S. — https://www.youtube.com/watch?v=Yb4P_QM-Rjc (other global migration diseases, from other parts of the world, are covered on this page as well)
Australian Disease Patterns, entire U.S. — http://www.scoop.it/t/national-population-health-grid/p/4021930885/2014/05/25/australian-disease-in-migration-patterns-youtube
The EMR records of all diseases from other countries, merged onto one dataset- – https://www.youtube.com/watch?v=Nh7iU04GNXg
See on Scoop.it – Medical GIS Guide
November 9, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on Historical Medical Geography and Disease Mapping – Visitors Stats
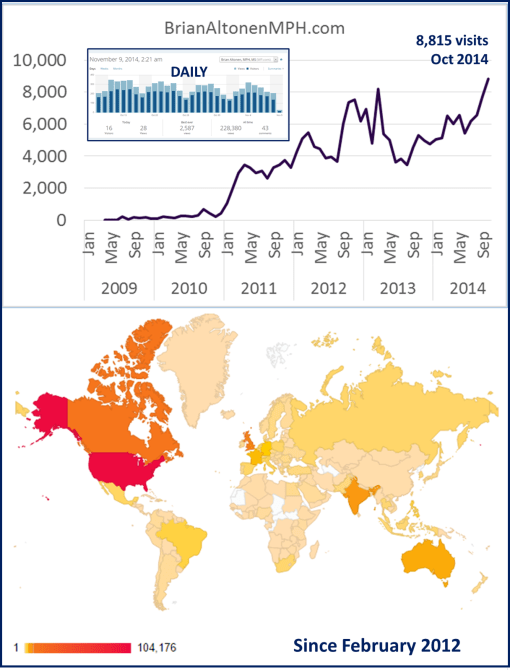
Stats on visitors at my Blog site.
This site began as my CV while searching for work. I converted it to the site where I post my past work, research findings, and teaching notes on medical geography, historical medical geography, managed care, cultural medicine managed care design, qualitative-quantitative research methods, medical history, the history of plant use in medicine, medical anthropology, etc., etc.
Total views since 3/2009 = 228,380 — total viewers, about 142,250 (1.5 page views/viewer).
58.2% of these Visitors were for the Medical Geography pages.
My most frequently visited page is my home page – – 13,017 views, 67 months.
The most views on a single day ever was 2,587.
Top 5 Countries are: US, Canada, UK, India, Australia
In terms of the hexagonal grid method I developed . . .
During the past four years, 4,684 have explored the descriptive page on this methodology and reviewed the algorithm (mostly students).
About 48.5% of them downloaded the spreadsheet with the formula, for use in GIS exercises, projects and teaching. Several sent emails of thanks and are now in the work place.
Canada geographers are more exploratory with the hexagonal grid method than US geographers, based on numbers of visitors and emails received.
More stats below.
RANK — TITLE OF PAGE VISITED — Number of visits
1 — Central Mexico Disease Geography (ca. 1880) — 5,578
2 — 1851 – 1917, Cattle Drives and Texas Fever — 5,432
3 — Small Pox and the Cree — 4,755
4 — Hexagonal Grid Analysis — 4,684
5 — Combined Qualitative-Quantitative Research Methods — 4,372
6 — The Coldens’ Flora – A Taxonomic Review — 3,752
7 — Caribbean and African Medicine in the Hudson Valley — 3,692
8 — Late Trapper Medicines (ca. 1825-1850) — 3,519
9 — Rituals and Sainthood — 3,229
10 – Cholera on the Oregon Trail (Thesis) — 3,048
11 – THE ECOLOGY OF NATURAL PRODUCTS — 2,795
12 – Early Western Travels, 1810-1850 — 2,727
13 – Four Prussian Diseases (ca. 1880) — 2,570
14 – “The James Way” of Raising Turkeys — 2,538
15 – DOWNLOAD Hexagonal Cells Excel Spreadsheet — 2,276
16 – Explorers and Plants, Part 2, Assigning Meaning — 2,221
17 – Pinta, Yaws and Bejel (ICDs 103, 102 and 104) — 2,116
18 – History of Discovering New World Plants — 2,029
19 – Historical Disease Maps — 1,929
20 – 1890 – The 1890 Census Disease Maps — 1,901
RANKING OF COUNTRIES – TOP 25 (descending)
1 — United States — 104,176
2 — Canada — 9,354
3 — United Kingdom — 8,160
4 — India — 5,567
5 — Australia — 3,753
6 — France — 3,272
7 — Germany — 3,185
8 — Philippines — 2,071
9 — Brazil — 1,983
10 – Italy — 1,598
11 – Netherlands — 1,492
12 – Mexico — 1,376
13 – Spain — 1,316
14 – Poland — 1,269
15 – Russian Federation — 1,248
16 – South Africa — 1,177
17 – Indonesia — 1,092
18 – Thailand — 1,090
19 – Malaysia — 1,028
20 – Korea, Republic of — 937
21 – Pakistan — 893
22 – Turkey — 853
23 – Sweden — 745
24 – Belgium — 674
25 – Denmark — 670
TOTALS
Total Number of Visits from 3/2009 to 10/2014 = 228,388
Views per Visitor = 1.5
See on Scoop.it – Medical GIS Guide
November 9, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on REGIONS, HEALTH & the NEW Managed Care — the Pacific Northwest as an Example

[This figure is a depiction of changes in popular culture, medicine and health care practices over time in the Pacific Northwest; a variation of the same from my 2000 thesis]
WHAT IS REGIONAL HEALTH?
Can a standardized healthcare system and attached insurance program developed by the insurance industry meet the needs of a population as unique as that of the Pacific Northwest?
Regional health is a term I apply, as a spatial epidemiologist, to parts of this country where specific sociocultural patterns exist that make this region stand out from the rest of the country.
Regionalism has a long history in the field of geography. In the 1950s and 1960s it became disliked due to its “deterministic” like nature.
For the past thirty years, my experiences living in the Pacific Northwest region as an academician and another decade of reviewing its public health history ever since, I can say with certainty that the answer to this question is ‘No!’
The needs of people and families in a region as unique as the Pacific Northwest are not met by the current programs that exist.
This is a link to my work and series on regional health, finished ca 2009 – – Regional Health Planning and the Pacific Northwest Medical GIS and Regions series .
The Pacific Northwest is unique in that its population fends for its beliefs, sometimes as a people, sometimes as unique individuals each with their own demands. The public health and healthcare needs for this region require a careful evaluation of its traditional allopathic medical needs, followed by a review of the non-allopathic medical traditions, a focus on local cultural diversity requirements, and individual (per patient/member) healthcare needs.
A combined qualitative-quantitative research method is the best way to do this.
Source: brianaltonenmph.com
Portland is where the field of naturopathy matured into the accredited field that it is today (my page on its history – http://wp.me/Puh6r-4if ). [see also the map https://brianaltonenmph.com/wp-content/uploads/2011/02/naturopathicmap25.jpg?w=510&h=641 ] Unfortunately, there are other naturopathy education programs out there that are not accredited. As an applying student you’ll know this because they lack federally insured student loan programs.
Like osteopathy and chiropractics, there are just a few official schools in this country. But before you merge naturopathy with those other two non-allopathic professions, realize that unlike chiropractic and osteopathy professions, many of the teachings of naturopathy ultimately make their way into the common mindset in allopathy (the traditional MD).
Before there was physical therapy today, there was "physiotherapy" taught as a part of naturopathy. before we had nutritional specialists looking at diseases in ways other than by dietary recommendations, a core specialty in naturopathy schools focused on nutrition, food content and nutritional supplements use. Today’s geriatricians who recommended common herbal blends for women with menopause problems or men with prostate concerns, every one of these OTC recommendations existed for a century or two before in the naturopathy world, and its botanical or eclectic medicine predecessors. The use of a fat-rich diet to control intractable epilepsy in children was discovered in the 1920s by osteopaths, as a result of the nutritional treatments they recommended for kids.
The different forms of physiognomy, cultural physiotyping (eugenics), and electrotherapy we so heavily promoted due to Harvard and Yale professors, a stable way to treat psychological health patients in the 1800s and 1890s, by allopaths, individuals who we believed were born to become doctors due to their own family genetics history (Galtonism, see http://www.pinterest.com/altonenb/human-faculty/ ). Are today’s gene therapy and gene modification therapies coming into play as controversial and troublesome as the eugenics teachings of pre-WW2 years?
The cultural respect many patients have from their other care givers comes from their acceptance of traditional practices. We see that especially with herbalism, nutrition therapy, mindbody healing practices, and exercise therapy, but we also see regular medicine taking it in limited ways, such as through color and music therapy (new teachings in allopathic subspecialties), imagery (or cancer and psychology patients), past life counseling, meditation (taken seriously by allopathy only after 1980), prayer, yoga, exercise, and numerous other forms of mindbody therapy.
In the 1960s and 1970s, allopathy was in stiff competition with the "alternatives," whom later became the "complementary", and then the "integrative" and now the mixed integrative-allopathic forms versus the complementary non-integrative medical philosophies and faiths. Prayer and touch therapy remain around because the patient has to defines his/her treatments, not the MD.
Homeopathy remains extant due to its inexplicable success in some people–an allopathy specialist might call this some form of mindbody impact; a traditional allopath, unwilling to expect change in the original teachings and even recognize how much they were in error in the ’60s and ’70s, might have called it what is was called 30, or 50 or 70 and 90 years ago, different words for the same disbelief their teachings bore (http://wp.me/Puh6r-9cs ).
Allopathy has had more than a half dozen theories as to how acupuncture might be working, ranging from the first ones published in the mid 17th century, to the early neuroscience speculation of the 18th and 19th centuries, to the very complex and contemporary neurochemical, psychoneuroimmunological proposals published today. (Whenever there is something allopaths cannot explain, they need to extend their old model to find a new model with legitimate explanations.) [See my page http://wp.me/Puh6r-46q ]
Traditional Chinese medicine (TCM), present for sure since the Gold Rush years, is a major form of complementary medicine that is still evolving and developing to meet the allopaths’ needs. TCM in the Northwest also has an accredited multiyear school with L.Ac. and TCM as the main professions.
Hispanic/Latino/a healers (botanica, voodoo, and others) are an important the majority of our Hispanic families and communities in the U.S.
Unanisim (a Middle Eastern/muslim offshoot of Hippocrates’ teachings) is practiced, in very predictable places (on unaniism – – http://www.pinterest.com/altonenb/international-health/ ).
The field of geography has this specialty known as medical cultural geography. The post-modern period of medicine, in sequent occupancy terms, is that period when the culture of medicine goes beyond its emphasis on just allopathy and modern science forms of therapy. In the Pacific Northwest, monoclonal antibody or gene therapy can be just as important to the health of an individual as the different forms of herbal therapeutics options out there, or the availability of a spiritual counselor.
Does an allopath in the Pacific Northwest know the history, makings and consequences of these non-allopathic health traditions?
In a database I developed for this philosophy in 1982 (the toxicity of herbal medicines; at http://www.ouribis.com/ , updated every several years ever since), we can see how much an allopath needs to learn to be an expert in just this one facet of integrative medicine–the impact of herbal medicines on hepatic, renal, intestinal, neural, ocular, immunal, endocrine, dermal and other systems, and their impact upon metabolic pathways for drug breakdown.
To best understand how to develop a broad-based healthcare program at the population health level (institutions, teaching hospitals, insurance companies), there are these studies I developed to help these programs better understand their complex, interdisciplinary patient load. These are the "hot topic" in public health and healthcare administration for the next decade or two. Perfecting the mixed model (qualitative-quantitative methods) for evaluating a health care system is the next way we need to go in the "managed care" and health insurance professions. Combining EMR, GIS and NLP make such a change possible.
*******************************************
Regional Health Planning and the Pacific Northwest Medical GIS and Regions series (sections available for review).
Part I – Introduction — http://wp.me/Puh6r-7TZ
Part IV – 3D Mapping of Health — http://wp.me/Puh6r-8l5
Part V – Pacific NW 3D Mapping. — http://wp.me/Puh6r-8l2
See on Scoop.it – Medical GIS Guide
November 7, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on Culturally-linked diagnoses — geophagia or earth/clay pica
https://www.youtube.com/v/kF40U67U6ps?fs=1&hl=fr_FR
http://youtu.be/kF40U67U6ps dirt eating 0605 5
Source: www.youtube.com
There is a cultural part of the pica behavior we occasionally learn about. During the 1970s and 1960s, we learned about pica behavior in children due to the probmes of lead based paint, a requirement of home-builders in the early 1900s produced by health professionals in order to reduce mold growth in domestic settings–most lead paint used in the early 1900s was a consequence of the Chicago environment and mold infestations in much older homes, part for the course during the sanitation movement.
This new pica problem that is erupting much more slowly in the U.S. pertains to Caribbean and African American cultures. Numerous speculations appear in the medical literature about why this behavior continues, and it is usually linked to diet and nutrition related desires (the need for more iron for example).
Whatever the reason, some culturally-rich regions can be identified by reviewing the spatial distribution of these very unique cultural behaviors, as is the case for this mapping. On my Scoopit! page, you can see two maps conveniently side by side–the videomap of general African American/Caribbean linked diagnoses, culturally bound syndromes, genetic ICDs, Africa-/Caribbean-linked ecological diseases and other codes, in relation to this Pica related behavior.
See on Scoop.it – National Population Health Grid
November 6, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on Is Ebola Outbreak Entering New Phase?
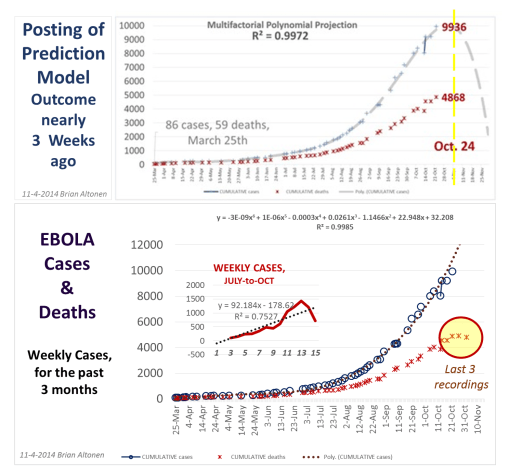
The reports of declining rates of new Ebola cases in Liberia, announced by the World Health Organization on Oct. 29, fueled hopes that the outbreak response is working, but experts are cautioning that it is too soon to believe the epidemic has entered a new phase, with slower growth. Liberia has been one of the hardest-hit countries in the current Ebola outbreak, with more than 6,500 cases and 2,413 deaths reported in that country alone as of Oct. 31. In addition to the perhaps positive news that the rate of new cases in Liberia is not growing, WHO officials said the total number of new cases in all three affected countries — Liberia, Sierra Leone and Guinea — also may be leveling off.
Source: news.yahoo.com
On October 24th I posted this graph with an outcome prediction I had been working with for more than a week. Back in September or early October, October 15th was a date I had defined for needing to see how the Ebola outbreak was behaving, based on the equation I developed.
The best mathematical model for Ebola, produced using non-supervised classification methods for the potential variables involved (an IDRISI GIS-RS term here), demonstrated the possibility that these numbers might begin to decrease. This didn’t really make much sense mathematically, but biologically and in terms of population density, and other numerous geographic requirements, I could accept the sensibility to it, at least from the way the computer was modeling the data.
The non-supervised classification system is opposite of what most other (even myself) like to do with outbreaks, try to define this behavior based on specific well define features, ranging from spatial density patterns to possible barriers, forms of resistance or friction to flow, etc. etc. We like to know what we are measuring and then see how that variable impacted the model. This tends to result in heterogenous, heteroscedasticity in our modeling, something we try to ignore.
The polynomial models developed without predetermining factors do not show these complicators of the equation. They tell it like it is, so to speak. This polynomial says there will be a sudden stop or reversal, and if that happened I would sooner or later need to know why (still haven’t really attacked that issue yet.)
Like others I am curious which way to outbreak is going. Is it ecologically decreasing due to seasonal, environmental and organismal-host-vector-victims change? Or is it decreasing due to saturating the population and impacting the most potential victims, having run out of more victims in the same region?
There is also that spatial behavior in which the organism and disease patterns begins "nesting" in its natural setting once again (staying active where it is most "comfortable", in an ecological sense.) Reducing the size of area it has spread into, concentrating on its best environmental settings in the 3 countries it is currently remaining active in.
See on Scoop.it – Medical GIS Guide
November 4, 2014
Posted by Brian Altonen, MPH, MS under Uncategorized
Comments Off on Florida for the winter? Perhaps not this year.

From the news story titled – – – “Health workers miss Louisiana medical conference over Ebola warning” – – – by Jonathan Kaminsky, NEW ORLEANS (Reuters) – A healthcare worker in Liberia is among those staying away from a tropical medicine conference in New Orleans after the state of Louisiana warned of quarantining attendees potentially exposed to Ebola, Doctors Without Borders said on Monday. Amanda Tiffany, an epidemiologist with the humanitarian aid group, was one of at least 10 people blocked from attending the annual meeting of the American Society of Tropical Medicine and Hygiene (ASTMH) on threat of quarantine, conference officials said, adding that they oppose the policy. … Tourism travel to Africa is now limited; will the same travel south for the winter soon be impacted?
Source: news.yahoo.com
The sections of two maps displayed come from a map (the one on the left) that has a very interesting background and history in medicine (https://brianaltonenmph.com/2013/04/ ). These two maps depict a strengthening of the tropical theory for pandemics, a proposal that became popular in medicine during the 1860s and 1870s. It complements much of the behaviors we have today about diseases like west nile, ebola, malaria. Our knowledge base and belief systems may advance and change over time, but human behavior and reaction to natural events typically do not experience much change.
The left image comes from British military epidemiologist Robert Lawson’s work in the late 1850s on the behavior of diseases like Yellow Fever in the Caribbean (http://wp.me/Puh6r-9s5 ). The right image is from one of his followers in the late 1800s, one of his strongest supporters, brilliant disease mapper Robert Felkin (http://wp.me/Puh6r-87N ).
Lawson was removed to the Caribbean by 1957 due to the failure of doctors at the great military hospital set up to deal with the vast numbers of injured and sick soldiers related to the Crimean War around 1854 (http://wp.me/Puh6r-abh , http://wp.me/Puh6r-9J6 ). This is the war that gave the founder of the nursing profession, Florence Nightingale, the fame that she deserves (http://wp.me/Puh6r-ayD ).
The interesting thing about Lawson’s map is it has rarely, if ever, been reviewed before by medical historians and medical geography historians (if there are any others out there).
Philosophically, I teach in my classes on statistics and spatial math that researchers with paradigms are important to the advancement of knowledge and science. The tussles that exist between the classic epidemiologists of today and the barely acknowledge spatial disease specialists who follow the geographers’ paradigms are perfect examples of these ongoing academic and professional debates.
Lawson in fact performed miserably while serving as Robert Lawson was working as Inspector-General in charge of maintaining British hospital units around the world, including the hospital in Scutari in 1854 (there are hundreds of pages on Nightgale and this epoch event, do your own search–or see for starters http://www.victorianweb.org/history/crimea/florrie.html ).
And Lawson naturally was the last to admit his errors, or accept responsibility for the poor sanitation of the Scutari hospital due to his mismanagement of poorly behaved doctors in Scutari. When Nightgale arrived to inspect this hospital in 1854, instead of retiring Lawson, Parliament sent him to the Caribbean (see Google version of the report on this visit by her, composed by Rev. Sydney Godolphin Osborne, 1855: http://books.google.com/books?id=pDfZAAAAMAAJ ).
In the Caribbean, Lawson almost immediately forgot his dreadful experiences in Crimea. After just a season or two residing in yellow fever bound Jamaica, he invented a new theory for endemic disease patterns — The Pandemic Wave Theory.
Lawson’s new theory was based upon a map of the world that depicts magnetic fields varying relative to latitude lines. This map was produced by Michael Faraday, and in today’s sense of producing scholarly research, a plagiarism of Faraday’s map with new title and new logic.
The fact that where Lawson resided was a rare anomaly in global magnetics behavior–fluctuations in the compass needle never happened in this part of the world–led him to draw his conclusions about disease and the latitudes lines, mostly by onserving yellow fever patterns.
Lawson used the varying magnetic patterns of the world to explain the deviations we see for certain diseases fail to behave according to the earh’s latitude and climate lines.
See https://brianaltonenmph.com/2013/04/25/humboldt-faraday-and-gauss-and-the-development-of-lawsons-law-of-pandemics/ ). The maps are nearly identical.
This reasoning became quite popular for a short while, and was even used to explain other epidemic disease patterns in need of such.
Fairly quickly, this theory became absent from the medical journals. Like many medical "beliefs", it was a phenomenon in human philosophy, behavior and character that lasted just a generation or two.
The numerous theories, speculations, fads, and other fancies posed out there on the internet regarding the current Ebola outbreak are interesting examples of how philosophy (belief) comes face to face with science and medicine at times (Occam’s Razor effect – – see my posting as well, on this – – http://wp.me/Puh6r-8a5 ).
Currently, there are two potential paradigms out there for dealing with the Ebola outbreak. The traditional approach is believing in the traditional science (what some writers call the "scientism approach", claiming science too is a philosophy).
But there is also the counter-theory out there, a sociological, demographic theory about how Ebola behaves and operates ecologically (human ecologically). This approach is dependent mostly on geographic, spatial modeling means for interpreting global disease patterns. It in fact complements our focus on the genetics of these new forms of disease, their evolution and their behaviors. ideally, a dual way of interpreting Ebola should be used–like the dual particle-wave theory of light. Both are right. But unfortunately, only one becomes the focus for the current profession, as their current paradigm.
.
See on Scoop.it – Medical GIS Guide
« Previous Page






